Introduction
Matsuda and Yabuuchi [1] first introduced the concept of contrast-enhanced abdominal ultrasonography (CE-US) in 1986. With the use of an intra-arterial infusion of carbon dioxide as the contrast material, CE-US had diagnostic utility because the signal emitted by the CO2 microbubbles was detected in real time during fundamental B-mode US. Kato et al. [2] first introduced contrastenhanced endoscopic US (CE-EUS) with the use of an intra-arterial CO2 infusion. However, a limitation of these methods was that US was only possible during an angiographic examination. In the mid- 1990s, EUS with a color/power Doppler function became possible, and the development of sonicated serum albumin, injected into a peripheral vein, enabled enhanced US, acquiring images without angiography [3-5]. The development of CO2 microbubbles and the progress of technical innovations, such as harmonic imaging, have resulted in improvements in the visualization of target lesions, increasing the utility of CE-EUS. Harmonic imaging visualizes microvessels and parenchymal perfusion by decreasing artifacts, such as blooming, in US [6].
In general, CE-EUS is categorized into two types: CE-EUS with the Doppler method (CE-EUS-D) and CE-EUS with harmonic imaging (CE-EUS-H). CE-EUS-D helps to distinguish between vascular-rich and hypovascular areas of a target lesion. CE-EUS-H provides a more detailed vasculature image of the target lesion [7]. Due to the differences between the two modes, information about the target lesion can be obtained and characterized depending on the purpose. Furthermore, the contrast-enhanced images acquired with CE-EUS can be subjected to quantitative analyses using Inflow Time Mapping (Hitachi Aloka Medical, Tokyo, Japan) and time-intensity curve (TIC) patterns to objectively characterize the target lesions [7]. Additionally, threedimensional (3D) CE-EUS can provide positive information regarding the relationship between the target location and the locations of adjacent organs and blood vessels via 3D reconstructed images [8-10]. Such progress in the development of CE-EUS has enabled the characterization of microvascularization, which can be used in the differential diagnosis of benign and malignant focal lesions as well as to improve the staging guidance for therapeutic procedures. In this review, we describe the current status of CE-EUS and the direction of future developments.
Contrast Agents
Contrast agents, used in CE-EUS and injected into peripheral veins, are an important factor in enhancing ultrasonograms. Contrast agents generally consist of gas-filled microbubbles, encapsulated by a phospholipid or albumin shell. They are classified into three types on the basis of their capability for transpulmonary passage and their half-life in the human body [7,11]. Commercially available contrast agents are listed in Table 1. The first ultrasound contrast agent (UCA) was Levovist (Bergkamen, Germany), consisting of microbubbles of air, covered by galactose and palmitic acid [12]. When this agent is used, contrast-enhanced harmonic imaging requires high acoustic power to oscillate or break the Levovist microbubbles. However, the EUS instrument is equipped with only a small transducer, and therefore, the transmission signals are too low to oscillate or break the Levovist microbubbles. In contrast, second-generation contrast agents for US, such as SonoVue (Milan, Italy), Sonazoid (Little Chalfont, UK), and Definity (N. Billerica, MA, USA), can be oscillated or even broken with a small transducer [12]. Due to the limited acoustic power of EUS, second-generation agents are more appropriate for EUS [13]. The only third-generation agent currently available is Echogen (Washington, DC, USA), which undergoes a phase shift from liquid to gas at body temperature [14]. The contrast agents that are currently in use are relatively safe, and no severe or long-lasting adverse effects have yet been reported in humans [11].
Clinical Applications: Diagnosis
Through a hemodynamic analysis with enhanced images obtained using contrast agents, CE-EUS can be used in the differential diagnosis of various gastrointestinal diseases. Topics that are being researched in conjunction with various diseases are discussed below.
Pancreatic Disease
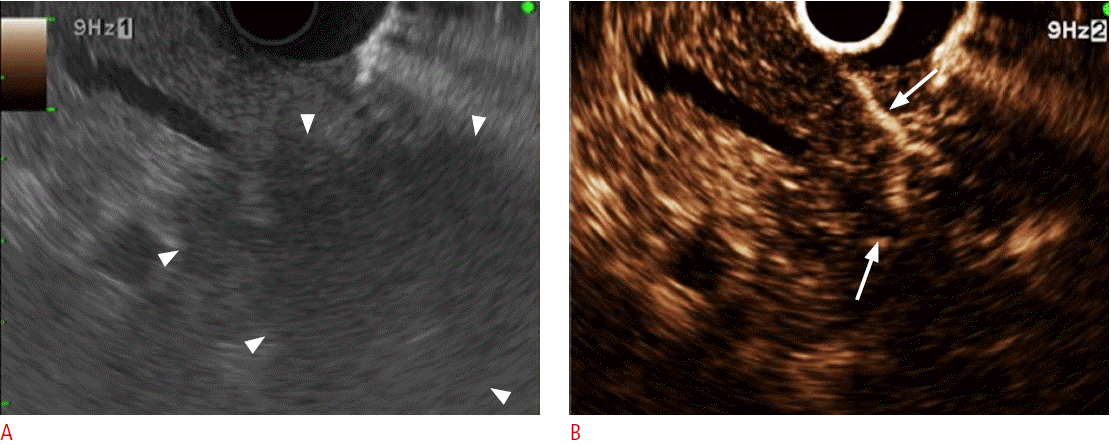
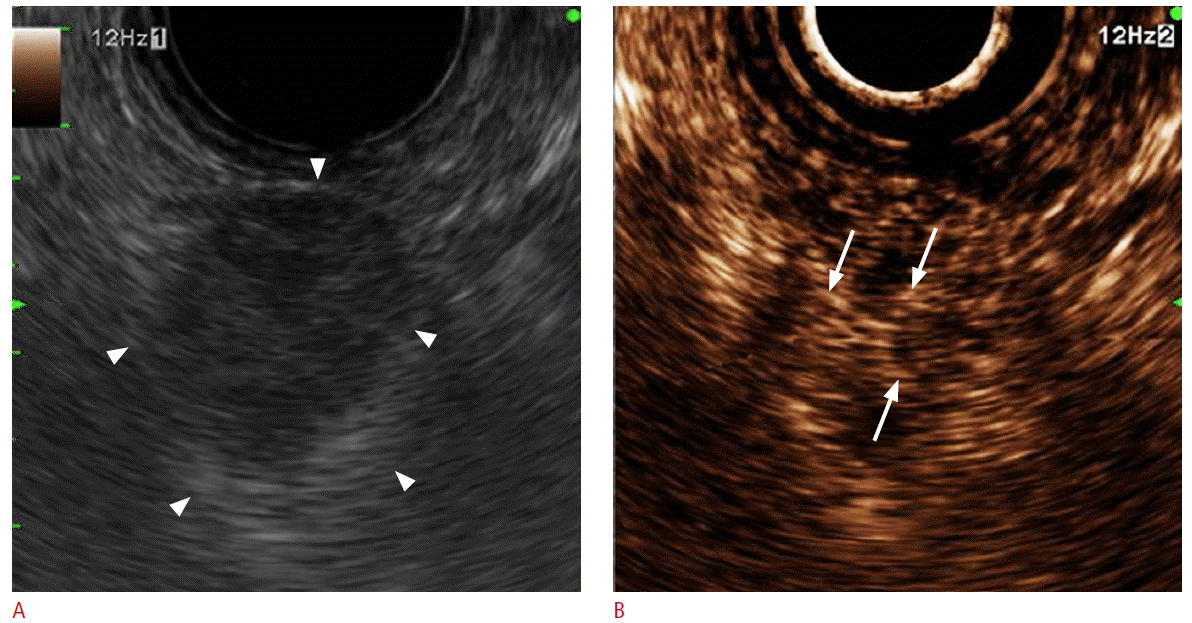
Because EUS can acquire high-resolution images of the pancreas, it is considered a highly sensitive method for evaluating and diagnosing pancreatic lesions, when compared with other imaging modalities [15,16]. However, EUS has limitations in evaluating intratumoral vascular structures or enhancement patterns in the characterization of pancreatic lesions because it lacks enhancing technology. To overcome the limitations of EUS, CE-EUS evaluates vascularity using contrast agents to characterize the lesion(s) [17-27]. In a meta-analysis, the sensitivity and the specificity of differentially diagnosing pancreatic adenocarcinoma using CE-EUS were reported to be 94% and 89%, respectively [20]. CE-EUS helps in visualizing the microvasculature of a pancreatic lesion to permit the characterization of intertumoral structures. This characterization can help in the diagnosis of pancreatic ductal adenocarcinoma in difficult cases by permitting the observation of hypovascularity, one of the signs of ductal adenocarcinoma [6,17] (Fig. 1). In particular, the utility of CE-EUS has been reported to include differentiation of focal pancreatitis and carcinomas [4,28,29], preoperative localization of pancreatic endocrine tumors [30,31], differentiation of mural nodules in intraductal papillary mucinous neoplasms, and detection of malignant transformations [32,33] (Fig. 2). CE-EUS images showed irregular vascularization with only arterial and no venous vessels in pancreatic cancer but regular vascularization with the detection of venous vessels in focal pancreatitis [4]. This difference may be attributed to the relatively high pressure inside a ductal adenocarcinoma of the pancreas due to the surrounding fibrous tissues. Pancreatic cancer has been shown to be a hypoperfused lesion, in comparison with the surrounding normal pancreatic parenchyma, but an inflammatory mass has been demonstrated as a hyperperfused or isoperfused lesion in CE-EUS [28]. Furthermore, various approaches have been proposed for differentiating between pancreatic adenocarcinoma and pancreatic disease. Vascularity can be analyzed quantitatively by generating TIC while performing CE-EUS [7,18,34,35]. Maximum intensity, accumulated intensity during observation, intensity reduction rate, and the ratio between the uptake by the mass and the uptake by the surrounding parenchyma are measured through quantitative analyses, using TIC, and are useful in differentiating autoimmune pancreatitis, pseudotumors, neuroendocrine tumors, and carcinomas [18,34-36]. The maximal intensity and the maximal accumulated intensity (peak intensity minus base intensity before contrast injection) of pancreatic carcinoma were significantly lower than in autoimmune pancreatitis [35]. The echo intensity reduction rate from the peak at 1 minute was greatest in pancreatic cancer, followed by mass-forming pancreatitis, autoimmune pancreatitis, and neuroendocrine tumor [34]. The contrast uptake levels in pancreatic adenocarcinoma and chronic pancreatitis were significantly lower than in the surrounding tissue. However, the contrast uptake ratio compared with the surrounding tissue in a pancreatic ductal adenocarcinoma was significantly lower than in chronic pancreatitis [18]. In another study, the signal intensity compared with the parenchyma and maximal intensity in pancreatic adenocarcinoma was lower than in chronic pseudotumoral pancreatitis, while the time to peak was significantly greater in pancreatic carcinoma than in pseudotumoral pancreatitis [36]. CE-EUS can also be used for T-staging of pancreatobiliary carcinomas by observing the invasion at the portal vein more accurately than with EUS [37].
While EUS-guided fine-needle aspiration (EUS-FNA) has assumed an important role in the pathological diagnosis of pancreatic masses, it sometimes fails when used to identify diffusely infiltrating pancreatic carcinoma, particularly in patients with chronic pancreatitis or a recent episode of acute pancreatitis [38]. In such cases, CE-EUS can be useful for observing the lesion and finding a suitable target lesion for EUS-FNA [25,27,39]. In certain studies, CE-EUS has been reported to complement EUS-FNA by assisting in the differentiation of a pancreatic adenocarcinoma that had been overlooked as a false negative while using EUS-FNA. However, there is disagreement as to whether CE-EUS can serve sufficiently as a complete replacement for EUS-FNA [17,27]. CE-EUS may serve as a complementary tool for EUS-FNA in difficult situations due to an intervening vessel or anticoagulation therapy.
Gallbladder
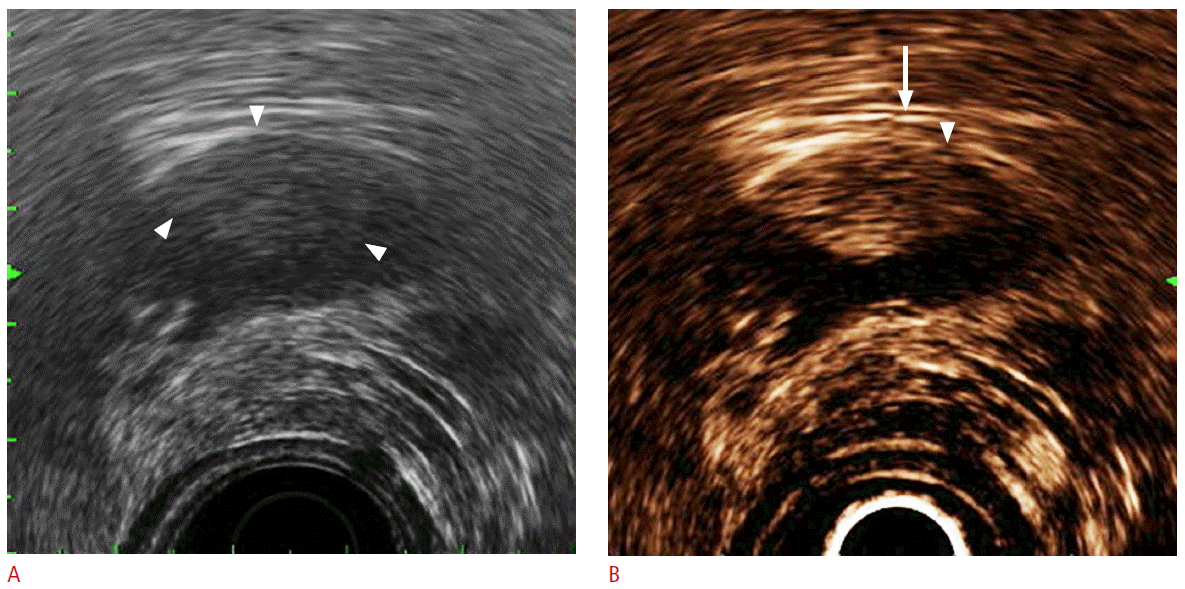
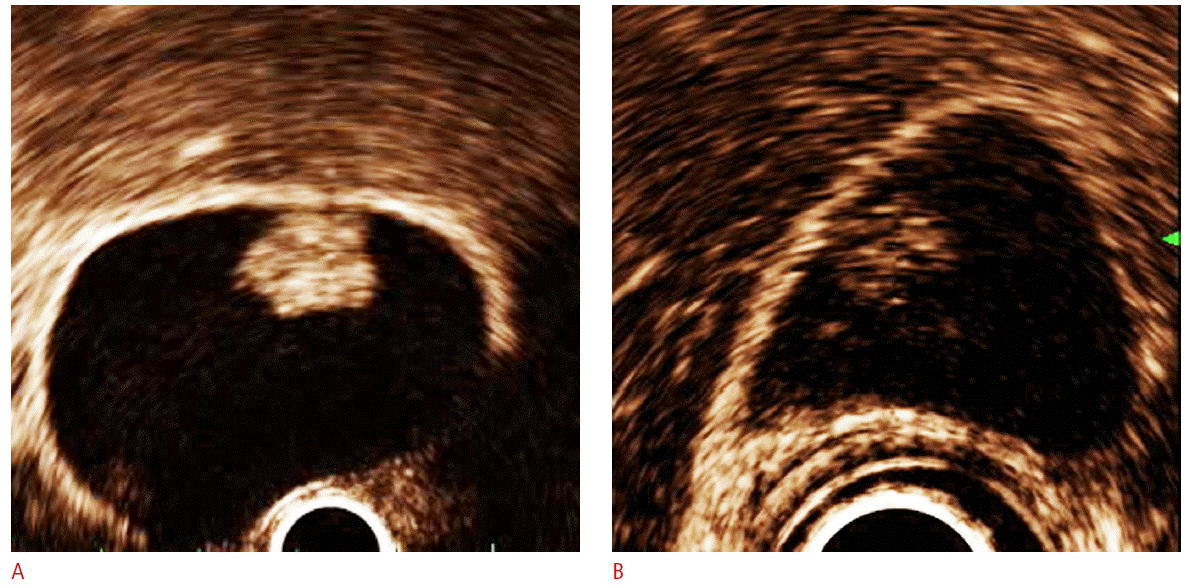
CE-EUS can facilitate the identification of the depth of cancer invasion in the diagnosis of gallbladder (GB) cancer. By enhancing the first and the third layer of the GB wall, we can improve the resolution between the GB wall structure and a cancerous lesion, assisting in T-staging by differentiating between T1b and T1a tumors with greater accuracy [7,40] (Fig. 3). The depth of tumor infiltration was determined according to the TNM classification, as follows: T1, hypoechoic tumor invades the first (T1a) or the second layer (T1b); and T2, hypoechoic tumor invades the third hyperechoic layer with no extension beyond the third layer or into the liver. CE-EUS can show a three-layer structure consisting of hyperechoic, hypoechoic, and hyperechoic layers from the GB luminal side. The echogenic first and third layers are enhanced and the intactness of the three-layer structure can be distinguished by CE-EUS. In one study, the accuracy of EUS in depicting the depth of tumor invasion was 78.6%, which is lower than the 92.9% accuracy of CE-EUS [40]. Furthermore, CE-EUS can not only differentiate between infiltrating and exophytic GB cancer but also between benign GB diseases, including chronic cholecystitis, which exhibit three intact GB layers, and cholesterol polyps [3]. Moreover, CE-EUS can facilitate the differentiation of GB adenoma and cholesterol polyps according to the homogeneity and size of the GB polyps and their enhancement patterns [41] (sensitivity, 75%; specificity, 66.6%) (Fig. 4); most adenomas show homogeneous enhancement, while the cholesterol polyps show heterogeneous enhancement patterns.
Gastrointestinal Tract Disease
Through the enhancement of the third and the fifth layer of the esophageal and gastric walls, CE-EUS can assist in the evaluation of the depth of invasion of esophageal and gastric adenocarcinoma, with greater accuracy (90%) than EUS (76.7%) [42,43]. Furthermore, in terms of CE-EUS with TIC, the echo intensity of gastrointestinal stromal tumors (GIST) can assist in differentiation because their values are higher than those of other benign tumors [44]. Additionally, with the use of CE-EUS, irregular vessels that enter from the periphery to the center of the GIST can be visualized for highgrade GISTs; thus, CE-EUS can be used to evaluate the malignant potential of GIST [45].
Lymph Nodes
CE-EUS plays an important role in the detection of lymph node (LN) metastasis. Although EUS-FNA is useful in the pathological confirmation of LN status, CE-EUS can be useful in cases of mediastinal and abdominal LNs that do not approach the aspiration yield [46,47]. CE-EUS can detect a filling defect, which is a typical sign of malignant lymphadenopathy, with a sensitivity of 100% and a specificity of 84% [46]. Furthermore, CE-EUS can be used to clearly observe the microvasculature of intra-abdominal lesions of undetermined origins, which can facilitate the differentiation of malignant from benign lesions, because of the homogeneous enhancement of benign lesions [48]. As such, it is expected that CE-EUS with respect to the LN status can be used for the N-staging of digestive tract tumors.
Other Diseases
Various clinical applications of vessel visualization by CE-EUS are being implemented. Color Doppler EUS and CE-EUS can be combined to evaluate the morphological and hemodynamic characteristics of visceral vascular diseases, which can be useful for the diagnosis of splanchnic artery disease [49]. It can also be used to determine the appropriate treatment of isolated mesenteric artery dissection [49]. In this report, it was suggested that the intimal flap and blood flow within the true lumen in patients with celiac artery dissection be evaluated with CE-EUS; further, it was reported that this information is useful in deciding the medical treatment or surgery. Enhanced vessels and the third echogenic layer of the esophageal wall can be visualized to detect perforating veins and periesophageal varices [50]. Cholecystoduodenal fistulas have also been detected by means of an enhancement of the gastrointestinal tract using CE-EUS [51].
Clinical Applications: Treatment Monitoring
Although no direct therapeutic procedure can be performed with it, CE-EUS serves as a monitoring tool for a range of disease entities. Many studies are being conducted to expand the role of CE-EUS in the evaluation of the effects of treatments of such diseases. One of the greatest strengths of CE-EUS, the visualization of vessel function, makes this possible. For the treatment of focal pancreatic lesions, EUS-guided pancreatic tissue ablation has been used [52-54]. CE-EUS with microspheres monitors the altered pancreatic perfusion of an ablated pancreatic lesion, allowing the detection of the vascularity at the necrosis site, which can be useful in follow-up with a post-ablation treatment [55].
Tumor blood flow is generally associated with metastatic potential and poor prognosis [11]. The quantity of vascular signals, measured with CE-US, has been reported to be useful in the early assessment and monitoring of the efficacy of antiangiogenic agents for pancreatic ductal carcinoma before morphological changes occur [56]. The quantity of vascular signals detected from pancreatic ductal carcinoma by CE-US correlated with tumor characteristics and vascular endothelial growth factor (VEGF) expression [57]. The rate of hepatic metastasis and the VEGF expression were significantly higher in patients with high vascular signals than in those with almost no vascular signal. Furthermore, CE-US may be a feasible technology for molecular imaging of the expression of VEGF receptor type 2 (VEGFR2) [58]. After UCAs conjugated with an anti-VEGFR2 monoclonal antibody or an isotype control antibody were randomly injected into breast cancer cells implanted in athymic nude mice, the sonograms were analyzed by calculating the intensity amplitudes, and the tumor samples were harvested for the analysis of VEGFR2 expression. The mean intensity amplitude caused by a backscatter of the retained VEGFR2-targeted UCA was significantly higher than that of the control UCA. This study showed that targeted CE-US may enable in vivo molecular imaging of VEGFR2 expression in the tumor vascular endothelium and may be used for non-invasive longitudinal evaluation of tumor angiogenesis in preclinical studies. It is expected that CE-EUS will be used to assess the efficacy of antitumoral agents in pancreatic cancer because of the feasibility of these new technologies using CE-US.
One study reported the usefulness of CE-EUS in predicting the efficacy of chemotherapy in patients with inoperable pancreatic cancer prior to the actual chemotherapy [58]. Using images from the early image phase (10-40 seconds after injection of the contrast materials), researchers considered the vessel sign to be positive when large (diameter, ≥1 mm), irregular subepithelial intratumoral vessels flowing from the periphery to the center of the tumor were detected by CE-EUS. Patients with a positive vessel sign showed significantly longer overall survival and progression-free survival than patients with a negative vessel sign.
Discussion
Through technical innovations in EUS and the development of contrast agents, the use of CE-EUS has been expanded to many diseases. The various applications of CE-EUS include differentiating benign from malignant lesions of the pancreas, GB, LNs, and other gastrointestinal lesions, as well as assessing the depth of invasion of esophageal, gastric, and GB cancers for tumor staging. Additionally, CE-EUS can indicate tumor neovascularization using contrast agents. CE-EUS imaging is useful in assessing and monitoring the efficacy of antiangiogenic agents, and allows molecular imaging by quantifying tumor perfusion.
CE-EUS is significantly more sensitive and accurate than conventional EUS in detecting the relatively hypovascular ductal adenocarcinomas of the pancreas due to its enhancement ability [4,5,25,28]. CE-EUS imaging improves the depiction of pancreatic tumors, enabling the detection of small lesions that may be uncertain in conventional EUS because of biliary stents or chronic pancreatitis [25]. In terms of the efficacy of CE-EUS and conventional EUS in preoperative T-staging of pancreatobiliary tumors, CE-EUS is more accurate than conventional EUS (rate of misdiagnosis: CE-EUS vs. EUS=7.6% vs. 23%) [37].
Additionally, the efficacy of CE-EUS in the differential diagnosis of small pancreatic tumors was superior to that of contrast-enhanced multidetector-row CT (MDCT) in two comparative studies [5,27]. Although CE-EUS and MDCT did not differ significantly in diagnostic ability with respect to all pancreatic masses, CE-EUS exhibited the highest sensitivity in differentiating between pancreatic ductal carcinoma and other tumors in pancreatic masses <2 cm in diameter (CE-EUS, 83%; EUS, 11%; MDCT, 50%) [5].
Occasionally, CE-EUS can differentiate small pancreatic carcinomas that cannot be detected by other imaging modalities [15,27]. In one study, seven ductal carcinomas and two neuroendocrine tumors showed hypoenhancement and hyperenhancement, respectively, on CH-EUS in 12 neoplasms that were not detected by MDCT [27]. CE-EUS may be a promising method to detect and characterize small pancreatic tumors that cannot be identified by other imaging tools [59]. Enhancement patterns demonstrated by CE-EUS during the subsequent vascular phase (e.g., arterial and venous phases) can be similar to MDCT [60].
An advantage of CE-EUS is its ability to assess the contrast enhancement patterns in real time with a substantially higher temporal resolution than other imaging modalities without the need to predefine scan time points or perform bolus tracking [60]. Furthermore, repeated administration of contrast agents during CE-EUS is possible due to the excellent patient tolerance of such agents.
However, although CE-EUS further improved the efficacy of EUS in terms of the characterization of target lesions by allowing visualization of microvessels and parenchymal perfusion, the analysis of the enhanced images is subjective and operator-dependent. To overcome these limitations, Inflow Time Mapping has been proposed as a new tool for an objective quantitative evaluation [7]. Three-dimensional CE-EUS may also be useful in reducing operatordependence because the enhanced images are obtained by the freehand movement of the endoscope during CE-EUS [8,9]. However, the clinical applications of these new techniques are at present restricted to case reports and a few studies; further large-scale studies are needed.
In conclusion, conceptual innovations and continuous technical developments have enabled CE-EUS to be used as a supplementary or additive tool with other cross-sectional and dynamic imaging modalities like computed tomography and magnetic resonance imaging.



 Print
Print facebook
facebook twitter
twitter Linkedin
Linkedin google+
google+
 Download Citation
Download Citation PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC




