AbstractThe widespread use of ultrasonography places it in a key position for use in the risk stratification of thyroid nodules. The French proposal is a five-tier system, our version of a thyroid imaging reporting and database system (TI-RADS), which includes a standardized vocabulary and report and a quantified risk assessment. It allows the selection of the nodules that should be referred for fine-needle aspiration biopsies. Effort should be directed towards merging the different risk stratification systems utilized around the world and testing this unified system with multi-center studies.
Risk stratification is the assessment of a patientŌĆÖs health risk status, usually using a score. This assessment assists the physician and care team in recommending appropriate care services [1]. Until the 1980s, palpation alone was used for thyroid nodule detection. The advent of ultrasonography (US) triggered an apparent epidemic of nodules. Although approximately 5% of the general population has a palpable thyroid nodule [2], the rate increases to 67% with the use of US [3]. Thus, there has been a rise in the number of fine-needle aspiration biopsies (FNAs), which doubled between 2006 and 2011 in the United States, and the number of thyroid surgical operations has increased by 31% [4].
Among thyroid nodules, 5%-6% are believed to be carcinomas, representing 62,980 newly diagnosed cases in the United States in 2014 and 3.8% of all new cancer cases. Despite these figures, the prognosis remains excellent with an estimate of 1,890 related deaths (i.e., 0.3% of all cancer deaths) [5]. In France in 2012, newly discovered thyroid cancers represented 8,211 cases among a population of 66 million and were the fifth most frequent cancer in women [6]. Therefore, it has become mandatory to develop a tool to differentiate benign and malignant nodules. The widespread use of US and its low cost places it in a key position to play such a role.
The main aims for a new diagnostic classification system would be to detect the highest possible percentage of thyroid carcinomas, to be able to assert benignancy when relevant, to help select which patients should undergo FNA and/or surgery, and to reduce the number of unnecessary invasive examinations. 1.2 million thyroid US examinations and 93,000 FNAs are performed in France each year. Secondary goals would be to facilitate communication between practitioners and patients and enhance inter-observer agreement on US reports. These aims should be feasible for achievement by the average non-expert radiologist by using an easy-to-use system that is robust and reproducible.
Various combinations of US features have been studied to differentiate benign and malignant thyroid nodules. In 2002, a combination of four features was first reported by Kim et al. [7]; it was then confirmed by other groups [8,9]. The features included microcalcifications, a taller-than-wide shape, irregular borders, and marked hypoechogenicity; assessment of this combination was considered capable of diagnosing 94% of thyroid carcinomas. Mild hypoechogenicity [9-11] and, with the employment of elastography, high stiffness [12-14] have often been added to this list of features. At the other end of the spectrum, simple cysts, spongiform nodules, and various other patterns linked to autoimmune thyroiditis have been classified as characteristic of benign lesions [15].
Taking into account these reports, our team experimented with the thyroid imaging reporting and database system (TI-RADS) suggested by Horvath et al. [16] and found it difficult to apply. We thus decided to design our own TI-RADS [17].
The first step was to create an illustrated atlas of thyroid imaging. It is an e-atlas hosted by the French Society of Radiology, freely accessible online [18]. This atlas is divided into four main chapters: gland, nodule, intermediate patterns, and special cases. Each US feature is documented on one page, including a definition and an illustration (Table 1).
The second step was to create a structured and standardized report (Fig. 1). Interestingly, the same goal was accomplished in the United States in 2014 [19]. Some notions seem indispensable, such as numbering each nodule and locating them precisely (right, left, isthmus, superior, middle, inferior, anterior, posterior, internal, external). Furthermore, the nodules should be drawn and numbered on a diagram. This allows the unambiguous location of each nodule.
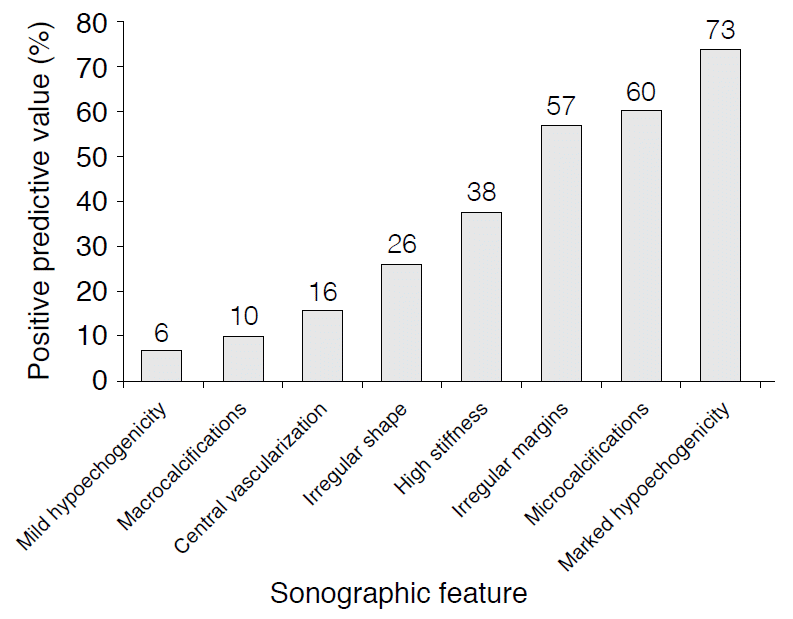
The third step was to test the diagnostic accuracy of the system. The pictures and reports of 500 nodules in 424 patients (341 benign nodules diagnosed cytologically and 159 carcinomas confirmed after surgery, consisting of 130 papillary carcinomas, 14 follicular carcinomas, and 15 medullary carcinomas) were retrospectively analyzed, applying the vocabulary and structured report described above. All patients had been referred for ultrasound-guided FNA of one or more nodules. The score was assigned after analyzing the positive predictive value (PPV) and negative predictive value (NPV) and odds ratio (Figs. 2, 3) of each individual US feature and of some combinations. It was a five-tier system. A score of TI-RADS 5 indicated that the nodule was very probably malignant (risk >95%): one or more suspect lymph node(s) were associated with a thyroid nodule harboring at least one of the four abovementioned signs described by Kim et al. [7]. TI-RADS 4C indicated a high risk of malignancy (risk range, 50% to 95%): there was at least one sign of high suspicion, marked hypoechogenicity, microcalcifications, irregular borders, or a taller-than-wide shape. TI-RADS 4B indicated an intermediate risk of malignancy (risk range, 10% to 50%): there were mildly hypoechoic nodules with macrocalcifications or central vascularization. TI-RADS 4A indicated a low risk of malignancy (risk range, 2% to 10%). There were two subcategories in this score: isoechoic nodules with macrocalcifications or central vascularization and mildly hypoechoic nodules with a thin halo or a mainly cystic composition. TI-RADS 3 indicated probably benign nodules (risk <2%): isoechoic nodules with no macrocalcifications or central vascularization. Finally, TI-RADS 2 indicated with virtual certainty a benign nodule corresponding to six different US patterns (simple cysts with no wall thickening, spongiform isoechoic nodules with no central vascularization, isolated macrocalcifications with no solid component or vascular signal, typical subacute thyroiditis: hypoechoic zone [not a nodule] in a clinical and biological context in favor of this disease, isoechoic grouped nodules hardly differentiated from one another, and ŌĆ£white knightsŌĆØ or rounded, hyperechoic, well delineated, multiple pseudo-nodules in a context of autoimmune thyroiditis [20]).
Two points are essential: if the nodule is partly hypoechoic, it is scored at least 4A and not 3; one sign of high suspicion is enough to score 4C. The sensitivity, specificity, and odds ratio of this version of the TI-RADS score were 95%, 68%, and 40, respectively.
The medical community judged the first system to be fairly complicated because it comprised eight subcategories. This led our team to try to simplify it. The next version was prospectively tested on 4,550 nodules in a 2-year study that included elastography [21]. All patients were referred for FNA. The algorithm used to score the nodules is shown in Table 2 and illustrated in Figs. 4-8. Assessment categories corresponded to a six-point scale: 1, normal; 2, benign; 3, very probably benign; 4A, low suspicion of malignancy; 4B, high suspicion of malignancy; and 5, effectively certainly malignant. Three thousand six hundred fifty-eight nodules were analyzed with a gray-scale score only and 991 nodules were analyzed with a combination of gray-scale and elastography. Final results were obtained with cytology interpreted according to the Bethesda system in all cases and also with histology after surgery in 263 cases. The TI-RADS score was considered exact when its result was benign (scores 1, 2, or 3) and the final diagnosis after cytology and/or histology was also benign (Bethesda II), or when its result was suspicious of malignancy (4A, 4B, or 5) and the final diagnosis was also malignant (Bethesda VI).
Nodules were classified as TI-RADS 2, 3, 4A, 4B, and 5 in 4.2%, 48.3%, 44.5%, 2.7%, and 0.3% of cases, respectively. TI-RADS scores of 4A, 4B, and 5 represented 95.7% of carcinomas (Bethesda 6) and 91.7% of suspicious lesions (Bethesda IV and V). The total number of carcinomas was 204, a prevalence rate of 4.5% (204/4,550). These corresponded to 139 cases asserted by cytological analysis (among them, 68 cases were confirmed by histopathology after surgery) and to 65 cases diagnosed after surgery and initially classified with the Bethesda system as category III, IV, or V. The risk of malignancy found by cytology or surgery for nodules classified with TI-RADS scores 2 to 5 was 0%, 0.25%, 6%, 69%, and 100%, respectively.
There were five signs of high suspicion, confirming repeated findings in the literature of the past 10 years: irregular shape, irregular borders, marked hypoechogenicity, microcalcifications, and high stiffness. These five signs allowed the detection of 74% of all carcinomas. Mild hypoechogenicity had to be added to reach a sensitivity of 98.5%. The specificity, NPV, and accuracy of this TI-RADS scoring system were 44.7%, 99.8%, and 48.3%, respectively.
Besides reducing the number of subcategories from eight to six, the other change was the inclusion of elastography in the list of features of high suspicion; however, this inclusion is debatable. After an initial report in 2005 [22], many studies have attempted to define the diagnostic value of elastography for the differentiation of benign and malignant thyroid nodules. Taken separately, elastography has the best sensitivity-specificity coupling for the detection of thyroid carcinomas, when compared to the other US features [23]. However, in more recent reports [13,14,24], the sensitivity of the method has dropped to 57%-85% and the specificity to 67%-94%.
It has to be understood that elastography can be used for two different purposes: either to raise the sensitivity, or the specificity, of gray-scale US. Raising specificity could be useful when trying to select patients and nodules that should undergo surgery after an indeterminate cytological result [25-29]. Regarding sensitivity, it has been shown in one prospective multicenter study that this could be increased by elastography [12]; however, other reports are contradictory [30,31].
How can one interpret these diverse results? One approach is to classify thyroid carcinomas into two categories. First, irregular infiltrative carcinomas, harboring a fibrous component, usually have one or more of the classical four features described by Kim et al. in 2002 [7], such as irregular shape or margins or marked hypoechogenicity. These correspond mainly to the classical variant of papillary carcinomas. The fibrous component explains the low elasticity, and elastography can be used to detect this. However, the classical US gray-scale features are very efficient diagnostic tools for the first type when applied in specialized centers [32]. This type represents around 80% of all carcinomas. The second type is non-infiltrative carcinomas with a regular shape and borders (mainly TI-RADS 4A), corresponding essentially to the follicular variant of papillary carcinomas. They have high elasticity, and elastography contributes little to their evaluation. The feature that allows for their diagnostic is their mild hypoechogenicity on US gray-scale and the four classical features are of poor value. This type represents around 20% of all carcinomas.
Numerous other features were not included in the TI-RADS score, mainly for reasons of simplification. However, each of these features has a true individual value that can be used in expert practice to refine the risk stratification. For instance, a round shape, an orientation that is non-parallel to the capsule, capsular bulging, or an exclusively solid composition evidence an increased risk of malignancy. In contrast, a flat shape (length >thickness├Ś2.5) or the presence of colloidal deposits evidence a lower risk. In particular, four of these US features were not included in the flowchart: macrocalcifications, central vascularization, presence or lack of the halo sign, and a mainly liquid composition. In our retrospective series [17], we calculated the odds ratio of each sign, which was 3.2, 5.8, 0.3, and 0.2, respectively, for those four. Therefore, a nodule classified as TI-RADS 3 has less than a 2% risk of being a carcinoma, even if it has macrocalcifications or central vascularization. On the other hand, a nodule scored TI-RADS 4A has a risk of 1.2%-1.8% of being a carcinoma if it has a halo or is mainly liquid. In other words, these features do not truly alter the risk of malignancy. In terms of comparison, the odds ratios of marked hypoechogenicity and microcalcifications were 70 and 52, respectively, far above the odds ratios of macrocalcifications and central vascularization. The other reason why we eliminated those four features was that we compared two versions of the TI-RADS score that did or did not use them and studied the inter-observer reproducibility. With the four features, on a subset of 146 patients the kappa value was 0.53 and PearsonŌĆÖs correlation coefficient 0.66. By removing those four features, the results of both tests in another subset of 135 patients were substantially increased, reaching 0.75 [21]. Therefore, we recommend not using those four signs in general practice, or to consider them as minor signs aimed only at modulating the indications for FNA.
The case of Doppler imaging is of particular interest because of its availability and widespread use. Traditionally, peripheral vascularization has been considered to show a predilection toward benignancy and predominantly central vascularization, toward malignancy. However, these criteria are controversial because Doppler sensitivity is highly dependent on the US machine used and because the definition of central vascularization has a low inter-observer agreement. For Moon et al. [33], Doppler imaging had no value, either alone or in combination with gray-scale imaging, whereas for other authors [10,11], it was considered to be significant and was retained in the final model for assessing risk stratification. Our team believes that the significance depends on size and agrees that it has poor inter-observer agreement; we retain Doppler on a case-by-case basis [34]. We have shown that there is no difference in vascularization between microcarcinomas and benign nodules measuring less than 10 mm. On the contrary, the presence of central vascularization becomes significant in nodules larger than 20 mm and even more important in nodules larger than 30-40 mm. The odds ratios for these three groups were 1, 4, and 10 respectively. Doppler imaging is also useful to differentiate thick colloid from hypoechoic solid tissue, especially in mainly cystic nodules.
Four different situations account for most false-positive US imaging cases. First, collapsing benign cystic nodules and scars in solid nodules after biopsy [35-37]: when a cyst grows rapidly under hemorrhagic or cystic transformation it has a high probability of spontaneous healing in the weeks or months following the initial increase. In this process, it will shrink and its initially oval or round shape can become irregular and taller-than-wide. Its borders can also appear irregular and spiculated and its content markedly hypoechoic. Taking a careful history from the patient and confirming a lack of internal blood flow on Doppler can help avoid misdiagnosis. FNA can still be performed; obtaining a colloid-only sample is then concordant and reinforces the probability of benignancy. US follow-up should be undertaken to confirm a decrease in size and the absence of emergence of a solid component. Solid nodules can also mimic cancer after biopsy; the scar produced by the procedure is markedly hypoechoic and has irregular borders. Investigating the patientŌĆÖs history can help.
The second situation is subacute thyroiditis [38,39]. At the onset of the disease, the thyroid can show markedly hypoechoic irregular zones that can mimic a carcinoma. Again, determining symptoms of pain in the patient, examining for accelerated cardiac rhythm, and looking for elevated serum C-reactive protein and thyroglobulin can assist in diagnosis, as can FNA or scintigraphy.
The third situation corresponds to hard nodules on elastography. Not all nodules with low elasticity are carcinomas. In our experience up to 9% of very hard nodules with a strain ratio >4.5 can be benign [21].
Finally, false-positives can occur with hyperechoic punctuations mimicking microcalcifications and corresponding to granular colloid deposits. These two entities are difficult to differentiate when granular colloid deposits lack a comet-tail artifact. Moreover, some hyperechoic punctuations correspond to acoustic enhancement in tiny micro-cystic cavities. This is more often seen with high frequency probes and has to be carefully identified to avoid improper overdiagnosis of microcalcifications.
False-negative results also correspond to four particular situations. The first one relates to histological subtypes. The encapsulated follicular variant of papillary thyroid carcinomas (FVPTC) represents in our experience 20% of carcinomas but 70% of undetected cases. This is known to take the US appearance of a regular solid isoechoic nodule that may or may not harbor a central vascularization [40,41]. During the prospective study [21], among the eight carcinomas classified as TI-RADS 3, one corresponded to an FVPTC. Despite this false-negative case, the sensitivity for the detection of FVPTC by US scanning was 94.4% (17/18 cases). In their report on 27 cases of FVPTC, Yoon et al. [41] showed that only 66.7% were correctly classified as malignant using published sonographic criteria. Follicular carcinomas can also be underestimated. In our retrospective study [17], sensitivity was 100% for the detection of medullary carcinomas (15 cases), 95% for the detection of papillary carcinomas (130 cases), but only 86% for the detection of follicular carcinomas (14 cases). Interestingly, their average size was 31 mm against 20 mm for all carcinomas; 79% were mildly hypoechoic and none were markedly hypoechoic or had microcalcifications. All of them were exclusively or mainly solid. Fifty percent had a predominantly central vascularization.
The second situation is location in the isthmus or in a pyramidal lobe. This makes it more difficult to determine the true echogenicity of a nodule because there is little or no surrounding normal tissue for comparison; these nodules thus appear isoechoic and benign although in reality they are mildly hypoechoic.
The third context is that of autoimmune thyroiditis. The thyroid gland is hypoechoic, and truly hypoechoic nodules are isoechoic compared to the hypoechoic gland and thus lack contrast, which renders them difficult to detect.
Last, some false-negative cases corresponded to mainly cystic nodules and were papillary carcinomas of the cystic variant. The solid portion of the mainly cystic nodules should be studied like a solid nodule in itself and carefully searched for hypoechogenicity and microcalcifications.
However, despite our efforts, at least 3%-5% of all carcinomas will remain unsuspected with US.
The main strength of the French TI-RADS relies on its large-scale prospective testing with a low rate of malignancy, corresponding closely to daily practice. It has high sensitivity and NPV. Compared to the previous French system, there are fewer subcategories and a trend towards simplification, which should enhance inter-observer agreement and ease of use. For further simplification, categories 4B and 5 could be merged into a single category called TI-RADS 5 (high suspicion of malignancy) and category 4A turned into a category 4 (low suspicion). When patients with newly discovered nodules are prospectively recorded and all nodules larger than 5 mm scored with the French TI-RADS system, TI-RADS scores 2 and 3 represent 2% and 66% of all nodules, TI-RADS 4A, 27%, and TI-RADS 4B and 5, 4% and 1%, respectively. Hence, very probably benign nodules are scored as TI-RADS 2 and 3 and represent 68% of all nodules. Since the NPV of these two scores is superior to 99.7%, more than two-thirds of all nodules can be reasonably excluded from further exploration, unless they present with aggressive features such as rapid growth, suspect adjacent lymph nodes or worrisome clinical features. The patient can be reassured of the very probably benign nature of the nodule. On the other hand, nodules scored 4B and 5 represent only 5% of all nodules but nearly 80% of all carcinomas. These are thus at high risk of malignancy and should be systematically explored. Their more rare nature implies that the costs involved should stay low.
US scanning is non-invasive but one of the major concerns is that it remains operator-dependent. Each of a subset of 180 nodules was successively scored in two different rooms, equipped with the same US machine, by two different practitioners unaware of prior scoring. Agreement was measured by taking into account the complete six-point scale and also by grouping scores 2 and 3 and 4A, 4B, and 5. This second procedure corresponded to the theoretical indications for proceeding to FNA. For the total six-point gray-scale TI-RADS score, the kappa value was 0.72 (95% confidence interval [CI], 0.62 to 0.81) and PearsonŌĆÖs concordance correlation coefficient was 0.73 (95% CI, 0.66 to 0.79). When considering only the indication for biopsy, the kappa value was 0.74 (95% CI, 0.65 to 0.84) and PearsonŌĆÖs coefficient, 0.74 (95% CI, 0.67 to 0.80). In both cases, the inter-observer agreement was substantial.
On the other hand, the main limitation is the number of nodules scored 4A: they represent 27% of all nodules. The individual risk of malignancy is low, ranging from 1% to 6% and being very constant among operators, but these nodules still represent nearly 20% of all carcinomas seen with US among all the nodules submitted to FNA. This means that there is a contradiction between the individual risk (low) and the overall risk of the population studied. Neglecting those nodules would lead to misdiagnosing around 20% of all carcinomas, which is of course unacceptable. One consequence is that the four features initially described by Kim et al. [7] are not sufficient and that mild hypoechogenicity should be inevitably added to the score to detect thyroid carcinomas. Another consequence is that studies should focus on these nodules scored 4A to determine whether it is possible to refine the risk of malignancy inside this category, probably by using other signs like composition, vascularization, and stiffness. However, introducing subcategories always complicates the system. Another possible limitation is the real efficacy when the system is used by less experienced operators. Interestingly, this problem was addressed by a report by Ko et al. [42] and received a rather reassuring answer.
In 2005, Reading et al. [20] advocated a pattern-oriented approach, as an alternative to the analysis of individual features. Those authors described eight typical appearances of commonly encountered benign and malignant nodules. The true concept of risk stratification was born in Korea and in Japan in 2007 and by that time was named a grading system [43,44]. It was qualitative, and thyroid nodules were classified into categories related to their US patterns. As in Reading et al. [20], indications for FNA were based on these categories.
In 2009, Horvath et al. [16] published the first study using TI-RADS in 1,097 nodules (156 carcinomas). The grading concept is transposed along the lines of the Breast Imaging-Reporting and Data System (BIRADS): a score of 1 denotes a normal examination, whereas scores 2, 3, 4, and 5 correspond to a risk of 0%, <5%, 5%-80%, and >80%, respectively. The sensitivity, specificity, PPV, and NPV were 88%, 49%, 49%, and 88%, respectively.
The same year, Park et al. [45] defined another TI-RADS in a study that comprised 1,694 patients (364 carcinomas). The value of the four major features of Kim et al. [7] was confirmed and two signs were added: solid and mildly hypoechoic, and the presence of suspicious lymph nodes. They established a mathematical equation with 12 parameters and a five-point risk stratification scale. FNA was recommended for scores 3 and 4, and surgery for score 5. It was a retrospective study, and the diagnostic efficacy was not tested.
In 2011, Kwak et al. [46] simplified the system designed by Park et al. [45] in a multicenter retrospective study of 1,658 nodules >10 mm, 298 of which were surgically removed. The authors showed that the number of features of suspicion could be used to predict malignancy. However, as a main limitation, each suspicious US feature was assigned the same weight despite carrying a different probability of malignancy. In 2013, to overcome this shortcoming, Kwak et al. [47] suggested a new model in which each individual US sign was assigned a risk score according to its odds ratio for predicting malignancy. The risk of malignancy in thyroid nodules increased in parallel with the calculated total score (sum of each score).
In 2014, the drafts of the new British Thyroid Association [48] and American Thyroid Association (ATA) guidelines [49] on the management of thyroid nodules were issued. They both have incorporated risk stratification systems. The British system is named the U score and the American system has no particular name. They both are five-point scales. The U score is qualitative and the ATA system quantitative. The American system shares many common points with the French system and transposition from one to the other is quite easy (Fig. 9), but the British one merges signs of very different values than other systems. Neither of those two systems have been tested, retrospectively or prospectively.
Finally, in 2015, a Korean team, Seo et al. [50], published a four-tier quantitative categorization system and suggested stratifying the risk of malignancy primarily by nodule echogenicity. The value of the composition (mixed, solid, liquid) in risk assessment was also elucidated.
In conclusion, a number of qualitative and quantitative US risk stratification systems for thyroid nodules are now being used on three continents, but no consensus on a single system has emerged.
The selection of the nodules that should be referred for FNA is based mainly on US risk stratification and secondarily on the evolution in size, but also on the context. Certain situations increase the risk of carcinoma and should be taken into account in the indications for FNA: neck irradiation during childhood, at least two familial cases of non-medullary thyroid carcinoma, a family history of medullary thyroid carcinoma or multiple endocrine neoplasia (MEN) type 2, a personal or family history of CowdenŌĆÖs disease, familial polyposis, Carney complex, elevated serum calcitonin, a suspect cervical lymph node or distant metastasis of possible thyroid origin.
Among these circumstances, the last four should be regarded as potentially increasing the gravity of the disease if a carcinoma is diagnosed.
As they are practically always asymptomatic, the sole question is what the benefits and risks of overdiagnosis are versus postponing diagnosis of subcentimetric nodules. Microcarcinomas currently tend to be considered benign a little too readily, and this is probably in part due to confusion caused by the literature: in most reports, the overall survival and recurrence rates are studied independently of the way thyroid microcarcinomas are discovered. However, among microcarcinomas, those fortuitously discovered after thyroidectomy for benign diseases represent 64% of all incidental microcarcinomas [51]. They do not correspond to the index tumor, primarily investigated by imaging, and should not be confused in the discussion of incidentalomas discovered with medical imaging. In a report by Mehanna et al. [52], it is shown that truly incidental microcarcinomas (i.e., those discovered on histology) have a much lower recurrence rate than non-incidental microcarcinoma (i.e., those presenting clinically with palpable thyroid nodules or a metastatic lymph node or identified by radiological investigation). Thus, in the latter case, FNA should probably be performed more often.
In any case, the overall prognosis of papillary microcarcinomas is excellent, and their evolution is slow. The disease-specific mortality from micro differentiated thyroid cancer, when not diagnosed because of palpable lymph nodes, is indeed under 1% [53]. Ito et al. [44], who performed a study that included subcentimetric carcinomas with a mean size of 6.9 mm, found that 6.4% and 15.9% of papillary thyroid microcarcinomas (PTMCs) showed increased size during a 5-year and 10-year follow-up period, respectively. Sugitani et al. [54] investigated PTMCs with a mean size of more than 8 mm; 7% of them increased in size during a mean 5-year follow-up period. However, in a report by Noguchi et al. [55], at 35 years, the recurrence rate of carcinomas between 6 and 10 mm was 14%.
Thus, new US criteria to determine the risk of aggressiveness of small carcinomas could also be used to define which subcentimetric nodules need FNA: nodules located near the thyroid capsule or suspected of extending beyond it [56-58]. The risk of being a pT3 carcinoma and association with central and lateral lymph node extension is increased. Chereau et al. [59] showed that among 178 micro-pT3 patients, recurrence was documented in 7.9% and 14.8% if they were N1. Thus, micro-pT3 N1 patients are at high risk of recurrence and should be treated aggressively. Nodules located at the upper pole of the thyroid also could harbor a higher probability of lateral lymph node extension with an odds ratio of 10 [58].
For subcentimetric nodules, FNA may be indicated for nodules with a TI-RADS score of 5 or 4B independent of the size of the nodule if metastatic lymph nodes are suspected, or for nodules of at least 5 mm if they are located near the thyroid capsule.
FNA can be suggested for all nodules above 10 mm scored TI-RADS 4B and 4A. For nodules scored TI-RADS 3, given the very high NPV of these scores, FNA could be suggested for nodules above 20-30 mm or if the context is at risk of malignancy. The remaining cases could be monitored by periodic neck US, for instance, after one year initially and then after 2 or 3 years. Complete discharge of the patient could be advised when the disease is found to be stable.
The complete flow-chart for FNA indications is shown in Table 3. What is the proportion of all existing nodules above 5 mm that would be submitted to FNA if one follows this flow-chart? TI-RADS 3 nodules measuring more than 20 mm represent 8% of all nodules, TI-RADS 4A over 10 mm, 12%, and TI-RADS 4B, 2%. This makes 22% of all nodules amenable for FNA. For the remaining ones, 11% of them [60-64] will increase in volume in a proven way, which in turn will represent 9% more nodules that will necessitate an FNA. Hence, following the algorithm suggested above, 22% of all nodules will be referred for FNA initially and 9% during a (long) follow-up for a total of 31%.
Efforts by the worldwide medical community involved in the management of thyroid nodules are converging towards US risk stratification systems, which provide a high sensitivity and NPV for the diagnosis of thyroid carcinomas. Many reports have already demonstrated that although this task is difficult, it is achievable. Effort should be directed towards comparing and merging the different systems utilized around the world. This unified system should be tested prospectively with multi-center studies and also outside the specialized world of thyroid imaging using dedicated US machines.
References1. American Academy of Family Physicians. Risk-stratified care management: practice management [Internet] Leadwood, KS: AAFP, [cited 2015 May 3]. Available from: http://www.aafp.org/practice-management/transformation/pcmh/advanced/rscm.html.
2. Hegedus L, Bonnema SJ, Bennedbaek FN. Management of simple nodular goiter: current status and future perspectives. Endocr Rev 2003;24:102ŌĆō132.
3. Ezzat S, Sarti DA, Cain DR, Braunstein GD. Thyroid incidentalomas. Prevalence by palpation and ultrasonography. Arch Intern Med 1994;154:1838ŌĆō1840.
4. Sosa JA, Hanna JW, Robinson KA, Lanman RB. Increases in thyroid nodule fine-needle aspirations, operations, and diagnoses of thyroid cancer in the United States. Surgery 2013;154:1420ŌĆō1426.
5. National Cancer Institute. SEER Stat Fact Sheets: thyroid cancer [Internet] Bethesda, MD: Surveillance, Epidemiology, and End Results Program, [cited 2015 May 3]. Available from: http://seer.cancer.gov/statfacts/.
6. Binder-Foucard F, Belot A, Delafosse P, Remontet L, Woronoff AS, Bossard N. Estimated national incidence and cancer mortality in France beween 1980 and 2012. Part 1. Solid tumors [Internet] Saint-Maurice Cedex: French Institute for Public Health Surveillance, [cited 2015 May 3]. Available from: http://www.invs.sante.fr/Dossiers-thematiques/Maladies-chroniques-et-traumatismes/Cancers/Surveillance-epidemiologique-des-cancers/Estimations-de-l-incidence-de-la-mortalite-et-de-la-survie/Estimation-de-l-incidence-et-de-la-mortalite-par-cancer-en-France-metropolitaine-entre-1980-et-2012-Tumeurs-solides.
7. Kim EK, Park CS, Chung WY, Oh KK, Kim DI, Lee JT, et al. New sonographic criteria for recommending fine-needle aspiration biopsy of nonpalpable solid nodules of the thyroid. AJR Am J Roentgenol 2002;178:687ŌĆō691.
8. Cappelli C, Castellano M, Pirola I, Gandossi E, De Martino E, Cumetti D, et al. Thyroid nodule shape suggests malignancy. Eur J Endocrinol 2006;155:27ŌĆō31.
9. Moon WJ, Jung SL, Lee JH, Na DG, Baek JH, Lee YH, et al. Benign and malignant thyroid nodules: US differentiation--multicenter retrospective study. Radiology 2008;247:762ŌĆō770.
10. Rago T, Vitti P, Chiovato L, Mazzeo S, De Liperi A, Miccoli P, et al. Role of conventional ultrasonography and color flow-doppler sonography in predicting malignancy in 'cold' thyroid nodules. Eur J Endocrinol 1998;138:41ŌĆō46.
11. Papini E, Guglielmi R, Bianchini A, Crescenzi A, Taccogna S, Nardi F, et al. Risk of malignancy in nonpalpable thyroid nodules: predictive value of ultrasound and color-Doppler features. J Clin Endocrinol Metab 2002;87:1941ŌĆō1946.
12. Trimboli P, Guglielmi R, Monti S, Misischi I, Graziano F, Nasrollah N, et al. Ultrasound sensitivity for thyroid malignancy is increased by real-time elastography: a prospective multicenter study. J Clin Endocrinol Metab 2012;97:4524ŌĆō4530.
13. Bojunga J, Dauth N, Berner C, Meyer G, Holzer K, Voelkl L, et al. Acoustic radiation force impulse imaging for differentiation of thyroid nodules. PLoS One 2012;7:e42735.
14. Zhang YF, Xu HX, He Y, Liu C, Guo LH, Liu LN, et al. Virtual touch tissue quantification of acoustic radiation force impulse: a new ultrasound elastic imaging in the diagnosis of thyroid nodules. PLoS One 2012;7:e49094.
15. Bonavita JA, Mayo J, Babb J, Bennett G, Oweity T, Macari M, et al. Pattern recognition of benign nodules at ultrasound of the thyroid: which nodules can be left alone? AJR Am J Roentgenol 2009;193:207ŌĆō213.
16. Horvath E, Majlis S, Rossi R, Franco C, Niedmann JP, Castro A, et al. An ultrasonogram reporting system for thyroid nodules stratifying cancer risk for clinical management. J Clin Endocrinol Metab 2009;94:1748ŌĆō1751.
17. Russ G, Bigorgne C, Royer B, Rouxel A, Bienvenu-Perrard M. The tyroid imaing reporting and data system. J Radiol 2011;92:701ŌĆō713.
18. Russ G, Bigorgne C, Royer B, Rouxel A. Score TIRADS for tyroid nodules [Internet] Paris: French Society of Radiology, [cited 2015 May 3]. Available from: http://pe.sfrnet.org/ModuleConsultationPoster/posterDetail.aspx?intIdPoster=4556.
19. Su HK, Dos Reis LL, Lupo MA, Milas M, Orloff LA, Langer JE, et al. Striving toward standardization of reporting of ultrasound features of thyroid nodules and lymph nodes: a multidisciplinary consensus statement. Thyroid 2014;24:1341ŌĆō1349.
20. Reading CC, Charboneau JW, Hay ID, Sebo TJ. Sonography of thyroid nodules: a "classic pattern" diagnostic approach. Ultrasound Q 2005;21:157ŌĆō165.
21. Russ G, Royer B, Bigorgne C, Rouxel A, Bienvenu-Perrard M, Leenhardt L. Prospective evaluation of thyroid imaging reporting and data system on 4550 nodules with and without elastography. Eur J Endocrinol 2013;168:649ŌĆō655.
22. Lyshchik A, Higashi T, Asato R, Tanaka S, Ito J, Mai JJ, et al. Thyroid gland tumor diagnosis at US elastography. Radiology 2005;237:202ŌĆō211.
23. Bojunga J, Herrmann E, Meyer G, Weber S, Zeuzem S, Friedrich-Rust M. Real-time elastography for the differentiation of benign and malignant thyroid nodules: a meta-analysis. Thyroid 2010;20:1145ŌĆō1150.
24. Bhatia KS, Tong CS, Cho CC, Yuen EH, Lee YY, Ahuja AT. Shear wave elastography of thyroid nodules in routine clinical practice: preliminary observations and utility for detecting malignancy. Eur Radiol 2012;22:2397ŌĆō2406.
25. Rago T, Scutari M, Santini F, Loiacono V, Piaggi P, Di Coscio G, et al. Real-time elastosonography: useful tool for refining the presurgical diagnosis in thyroid nodules with indeterminate or nondiagnostic cytology. J Clin Endocrinol Metab 2010;95:5274ŌĆō5280.
26. Rago T, Scutari M, Latrofa F, Loiacono V, Piaggi P, Marchetti I, et al. The large majority of 1520 patients with indeterminate thyroid nodule at cytology have a favorable outcome, and a clinical risk score has a high negative predictive value for a more cumbersome cancer disease. J Clin Endocrinol Metab 2014;99:3700ŌĆō3707.
27. Choi WJ, Park JS, Koo HR, Kim SY, Chung MS, Tae K. Ultrasound elastography using carotid artery pulsation in the differential diagnosis of sonographically indeterminate thyroid nodules. AJR Am J Roentgenol 2015;204:396ŌĆō401.
28. Cantisani V, Ulisse S, Guaitoli E, De Vito C, Caruso R, Mocini R, et al. Q-elastography in the presurgical diagnosis of thyroid nodules with indeterminate cytology. PLoS One 2012;7:e50725.
29. Lippolis PV, Tognini S, Materazzi G, Polini A, Mancini R, Ambrosini CE, et al. Is elastography actually useful in the presurgical selection of thyroid nodules with indeterminate cytology? J Clin Endocrinol Metab 2011;96:E1826ŌĆōE1830.
30. Moon HJ, Sung JM, Kim EK, Yoon JH, Youk JH, Kwak JY. Diagnostic performance of gray-scale US and elastography in solid thyroid nodules. Radiology 2012;262:1002ŌĆō1013.
31. Unluturk U, Erdogan MF, Demir O, Gullu S, Baskal N. Ultrasound elastography is not superior to grayscale ultrasound in predicting malignancy in thyroid nodules. Thyroid 2012;22:1031ŌĆō1038.
32. Kwak JY, Kim EK. Ultrasound elastography for thyroid nodules: recent advances. Ultrasonography 2014;33:75ŌĆō82.
33. Moon HJ, Kwak JY, Kim MJ, Son EJ, Kim EK. Can vascularity at power Doppler US help predict thyroid malignancy? Radiology 2010;255:260ŌĆō269.
34. Russ G, Rouxel A, Bienvenu-Perrard M, Bigorgne C, Royer B. Do ultrasound and elastographic patterns of thyroid carcinoma vary with their size? In: 36th Annual Meeting of the European Tyroid Association; 2012 Sep 8-12; Pisa, Italy. poster No. P188.
35. Wu HX, Zhang BJ, Wang J, Zhu BL, Zang YP, Cao YL. Conventional ultrasonography and real time ultrasound elastography in the differential diagnosis of degenerating cystic thyroid nodules mimicking malignancy and papillary thyroid carcinomas. Asian Pac J Cancer Prev 2013;14:935ŌĆō940.
36. Kim SS, Kim MR, Mok JY, Huh JE, Jeon YK, Kim BH, et al. Benign cystic nodules may have ultrasonographic features mimicking papillary thyroid carcinoma during interval changes. Endocr J 2011;58:633ŌĆō638.
37. Koo JH, Shin JH, Han BK, Ko EY, Kang SS. Cystic thyroid nodules after aspiration mimicking malignancy: sonographic characteristics. J Ultrasound Med 2010;29:1415ŌĆō1421.
38. Zacharia TT, Perumpallichira JJ, Sindhwani V, Chavhan G. Gray-scale and color Doppler sonographic findings in a case of subacute granulomatous thyroiditis mimicking thyroid carcinoma. J Clin Ultrasound 2002;30:442ŌĆō444.
39. Frates MC, Marqusee E, Benson CB, Alexander EK. Subacute granulomatous (de Quervain) thyroiditis: grayscale and color Doppler sonographic characteristics. J Ultrasound Med 2013;32:505ŌĆō511.
40. Kim DS, Kim JH, Na DG, Park SH, Kim E, Chang KH, et al. Sonographic features of follicular variant papillary thyroid carcinomas in comparison with conventional papillary thyroid carcinomas. J Ultrasound Med 2009;28:1685ŌĆō1692.
41. Yoon JH, Kim EK, Hong SW, Kwak JY, Kim MJ. Sonographic features of the follicular variant of papillary thyroid carcinoma. J Ultrasound Med 2008;27:1431ŌĆō1437.
42. Ko SY, Lee HS, Kim EK, Kwak JY. Application of the Thyroid Imaging Reporting and Data System in thyroid ultrasonography interpretation by less experienced physicians. Ultrasonography 2014;33:49ŌĆō57.
43. Tae HJ, Lim DJ, Baek KH, Park WC, Lee YS, Choi JE, et al. Diagnostic value of ultrasonography to distinguish between benign and malignant lesions in the management of thyroid nodules. Thyroid 2007;17:461ŌĆō466.
44. Ito Y, Amino N, Yokozawa T, Ota H, Ohshita M, Murata N, et al. Ultrasonographic evaluation of thyroid nodules in 900 patients: comparison among ultrasonographic, cytological, and histological findings. Thyroid 2007;17:1269ŌĆō1276.
45. Park JY, Lee HJ, Jang HW, Kim HK, Yi JH, Lee W, et al. A proposal for a thyroid imaging reporting and data system for ultrasound features of thyroid carcinoma. Thyroid 2009;19:1257ŌĆō1264.
46. Kwak JY, Han KH, Yoon JH, Moon HJ, Son EJ, Park SH, et al. Thyroid imaging reporting and data system for US features of nodules: a step in establishing better stratification of cancer risk. Radiology 2011;260:892ŌĆō899.
47. Kwak JY, Jung I, Baek JH, Baek SM, Choi N, Choi YJ, et al. Image reporting and characterization system for ultrasound features of thyroid nodules: multicentric Korean retrospective study. Korean J Radiol 2013;14:110ŌĆō117.
48. British Thyroid Association. Guidelines for the management of thyroid cancer [Internet] British Thyroid Association, 2014. [cited 2015 May 3]. Available from: http://www.british-thyroidassociation.org/Guidelines/Docs/BTA_DTC_guidlines.pdf.
49. Haugen B. Oral communication [Internet] Falls Church, VA: American Thyroid Association, [cited 2015 May 3]. Available from: http://www.thyroid.org/members-only/member11 resources/atadraft-guidelines/.
50. Seo H, Na DG, Kim JH, Kim KW, Yoon JW. Ultrasound-based risk stratification for malignancy in thyroid nodules: a four-tier categorization system. Eur Radiol 2015;25:2153ŌĆō2162.
51. Sassolas G, Hafdi-Nejjari Z, Remontet L, Bossard N, Belot A, Berger-Dutrieux N, et al. Thyroid cancer: is the incidence rise abating? Eur J Endocrinol 2009;160:71ŌĆō79.
52. Mehanna H, Al-Maqbili T, Carter B, Martin E, Campain N, Watkinson J, et al. Differences in the recurrence and mortality outcomes rates of incidental and nonincidental papillary thyroid microcarcinoma: a systematic review and meta-analysis of 21 329 person-years of follow-up. J Clin Endocrinol Metab 2014;99:2834ŌĆō2843.
53. McLeod DS, Sawka AM, Cooper DS. Controversies in primary treatment of low-risk papillary thyroid cancer. Lancet 2013;381:1046ŌĆō1057.
54. Sugitani I, Toda K, Yamada K, Yamamoto N, Ikenaga M, Fujimoto Y. Three distinctly different kinds of papillary thyroid microcarcinoma should be recognized: our treatment strategies and outcomes. World J Surg 2010;34:1222ŌĆō1231.
55. Noguchi S, Yamashita H, Uchino S, Watanabe S. Papillary microcarcinoma. World J Surg 2008;32:747ŌĆō753.
56. Kwak JY, Kim EK, Youk JH, Kim MJ, Son EJ, Choi SH, et al. Extrathyroid extension of well-differentiated papillary thyroid microcarcinoma on US. Thyroid 2008;18:609ŌĆō614.
57. Wang QC, Cheng W, Wen X, Li JB, Jing H, Nie CL. Shorter distance between the nodule and capsule has greater risk of cervical lymph node metastasis in papillary thyroid carcinoma. Asian Pac J Cancer Prev 2014;15:855ŌĆō860.
58. Kwak JY, Kim EK, Kim MJ, Son EJ, Chung WY, Park CS, et al. Papillary microcarcinoma of the thyroid: predicting factors of lateral neck node metastasis. Ann Surg Oncol 2009;16:1348ŌĆō1355.
59. Chereau N, Buffet C, Tresallet C, Tissier F, Golmard JL, Leenhardt L, et al. Does extracapsular extension impact the prognosis of papillary thyroid microcarcinoma? Ann Surg Oncol 2014;21:1659ŌĆō1664.
60. Brander AE, Viikinkoski VP, Nickels JI, Kivisaari LM. Importance of thyroid abnormalities detected at US screening: a 5-year follow-up. Radiology 2000;215:801ŌĆō806.
61. Kuma K, Matsuzuka F, Yokozawa T, Miyauchi A, Sugawara M. Fate of untreated benign thyroid nodules: results of long-term follow-up. World J Surg 1994;18:495ŌĆō498.
62. Cheung PS, Lee JM, Boey JH. Thyroxine suppressive therapy of benign solitary thyroid nodules: a prospective randomized study. World J Surg 1989;13:818ŌĆō821.
Standardized report for thyroid ultrasonography (US).TI-RADS, thyroid imaging reporting and database system; FNA, fine-needle aspiration.
 Fig.┬Ā1.Example of a nodule classified as TI-RADS 2.Axial scan shows a left simple cyst with sediment. The absence of a vascular signal in the echoic part must be asserted with Doppler ultrasonography. TI-RADS, thyroid imaging reporting and database system.
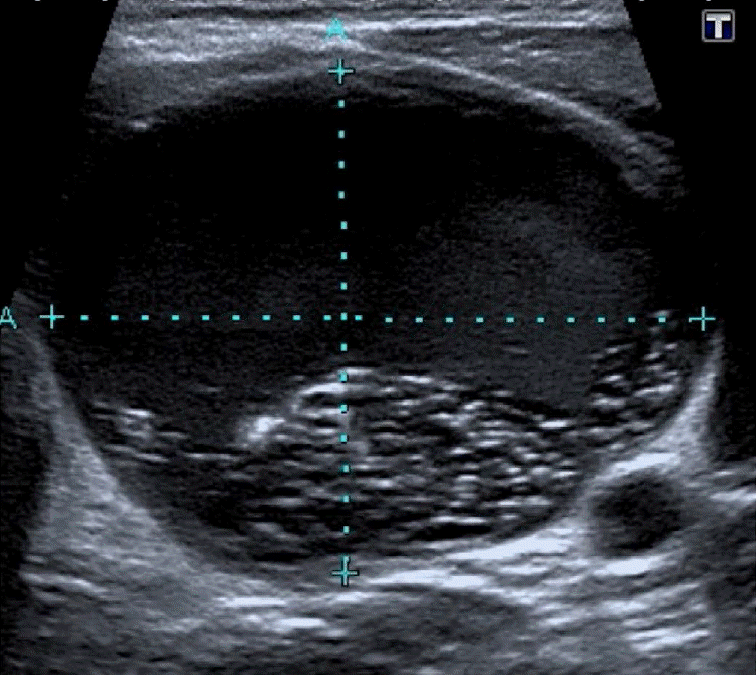 Fig.┬Ā4.Example of a nodule classified as TI-RADS 3.A, B. On the longitudinal (A) and axial (B) sonograms, the nodule has an oval shape and regular borders and is isoechoic for its solid portion. Mixed liquid-solid composition reinforces the probability of benignancy but does not change the score. TI-RADS, thyroid imaging reporting and database system.
 Fig.┬Ā5.Example of a nodule classified as TI-RADS 4A.Longitudinal sonogram shows a nodule with oval shape and regular borders that is mildly hypoechoic (more hypoechoic than the surrounding normal thyroid parenchyma, but no more hypoechoic than the strap muscles). TI-RADS, thyroid imaging reporting and database system.
 Fig.┬Ā6.Example of a nodule classified as TI-RADS 4B.A, B. On the longitudinal (A) and axial (B) sonograms, the nodule has irregular borders. It is solid and mildly hypoechoic. There is one feature of high suspicion. TI-RADS, thyroid imaging reporting and database system.
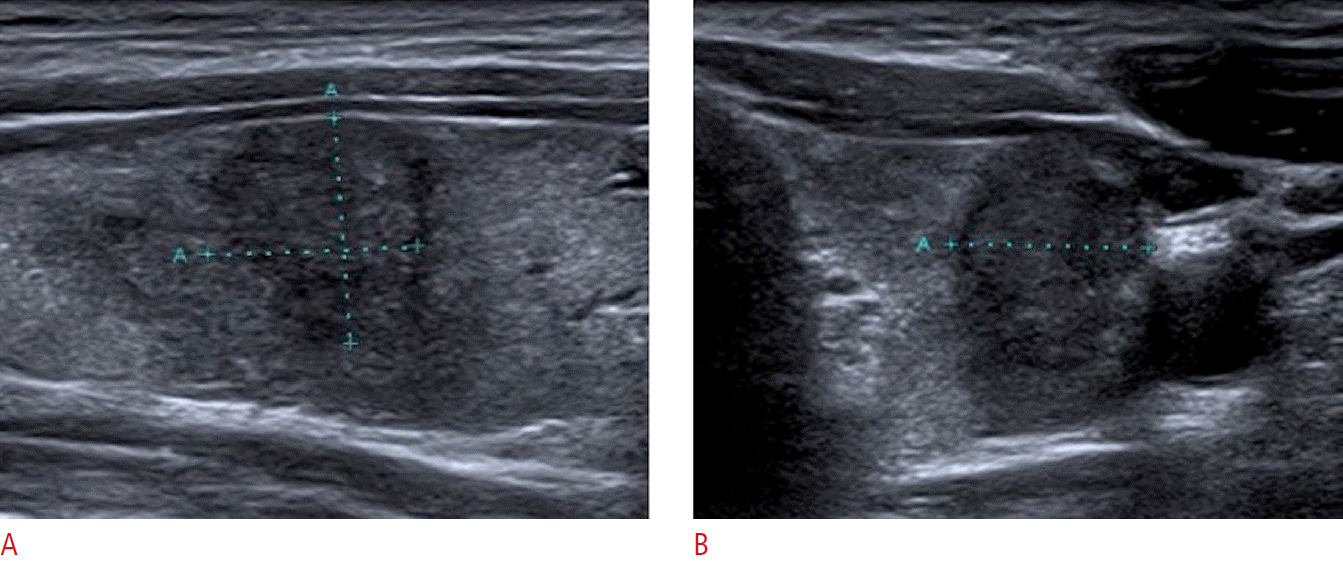 Fig.┬Ā7.Example of a nodule classified as TI-RADS 5.A, B. On the longitudinal (A) and axial (B) sonograms, the shape is irregular and taller-than-wide. The borders are irregular and lobulated. C. On the strain elastography, the nodule is almost entirely blue suggesting high stiffness. There are three features of high suspicion. TI-RADS, thyroid imaging reporting and database system.
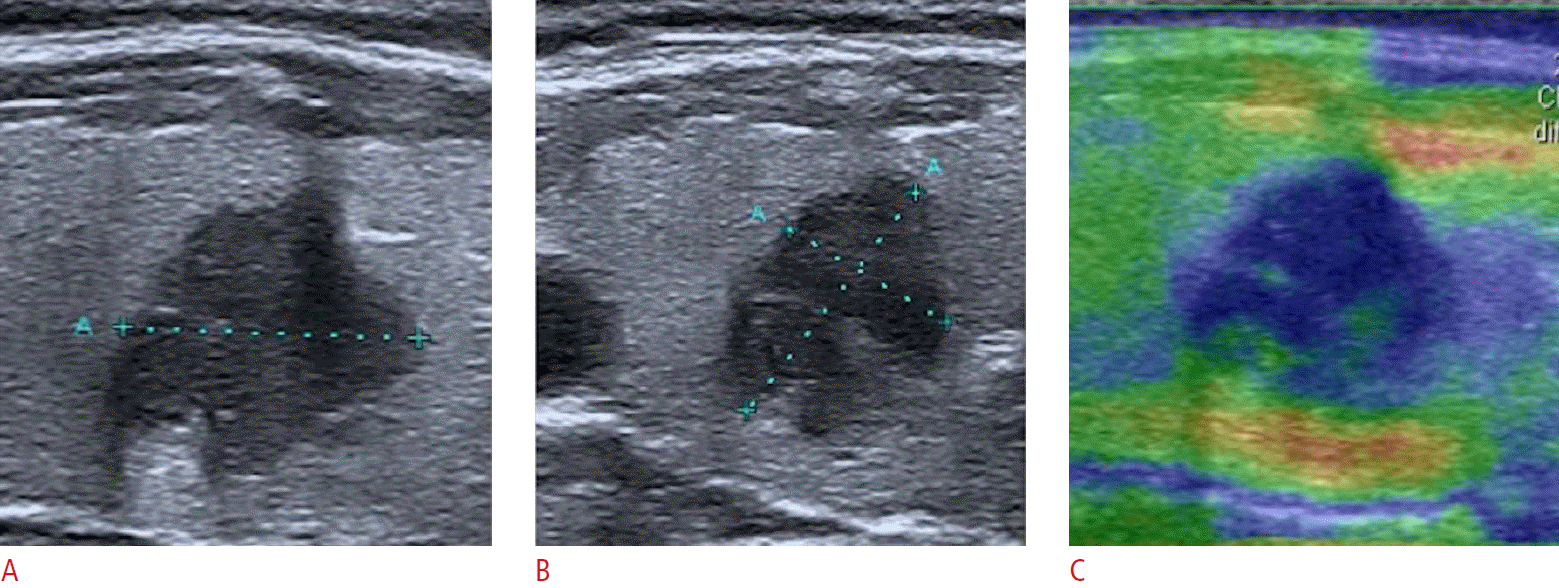 Fig.┬Ā8.Correspondence between the draft of ATA guidelines for risk assessment of thyroid nodules on ultrasonography (US) and French TI-RADS.ATA, American Thyroid Association; TI-RADS, thyroid imaging reporting and database system; FNA, fine-needle aspiration biopsy. a)The estimate is derived from high volume centers, the overall risk of malignancy may be lower given the interobserver variability in sonography. b)Aspiration of the cyst may be considered for symptomatic or cosmetic drainage; US FNA should be considered for lymph nodes that are sonographically suspicious for thyroid cancer.
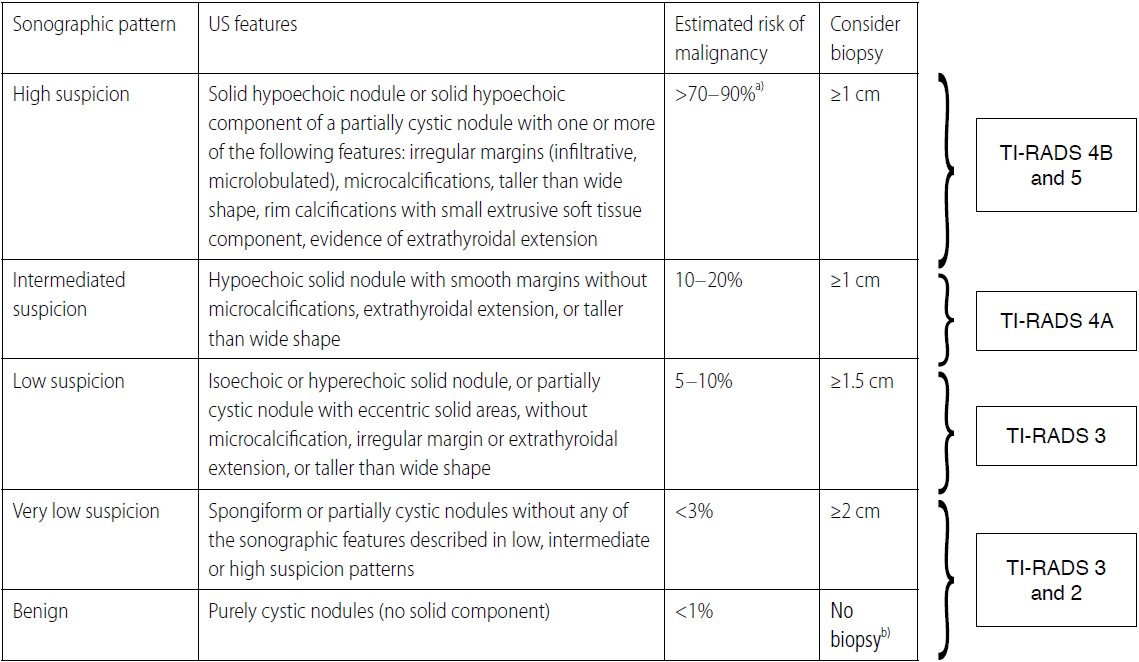 Fig.┬Ā9.Table┬Ā1.Standardized vocabulary for ultrasonography of thyroid nodules Table┬Ā2.Summary of the French TI-RADS categorization system Table┬Ā3.The indications for fine-needle aspiration biopsy (FNA) of thyroid nodules
|



 Print
Print facebook
facebook twitter
twitter Linkedin
Linkedin google+
google+

 Download Citation
Download Citation PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC




