Introduction
The common femoral artery (CFA) has a relatively large diameter, is located superficially, and can be easily compressed to achieve hemostasis; therefore, the transfemoral arterial approach is the most common mode of vascular access for angiography, percutaneous coronary interventions, or various endovascular therapies such as transcatheter aortic valve replacement. The incidence of femoral puncture-related complications has been reported to be 0.44%-1.8% during diagnostic angiography and up to 4% during interventional procedures [1]. Although there are various factors that can cause complications, such as old age, female gender, lower body surface area, type of procedure, status of the peripheral vasculature, or use of anticoagulants, the most common causes of puncture-related complications are inadequate access and anatomical variability [1]. To reduce the risk of procedure-related vascular complications, the recommended puncture site is the middle segment of the CFA (Fig. 1) [2]. If the puncture site is too low, the incidence of pseudoaneurysms, hematomas, arteriovenous fistulae (AVFs), or limb ischemia is increased, whereas the incidence of retroperitoneal hemorrhage is increased if the puncture site is too high [3]. Other complications such as thrombosis, aortic dissection, or extravasation may occur after transfemoral arterial interventions. Fluoroscopic guidance can help to localize the ideal puncture site of the vessel, which is over the lower half of the femoral head.
Duplex ultrasound, which consists of gray-scale and color Doppler ultrasound, has proven to be an excellent noninvasive modality that provides not only anatomic but also hemodynamic information [4]. Although ultrasonography has limited utility for evaluating patients with a poor echo window due to obesity or a large swelling, it should be used to establish a preliminary diagnosis, especially for patients with a palpable mass or an audible bruit. This article examines the findings from gray-scale and color Doppler images of various transfemoral puncture-related complications, including thrombosis, hematoma, pseudoaneurysm, AVF, or arterial dissection. Radiologists should be familiar with the characteristic sonographic findings of the entire spectrum of transfemoral puncture-related vascular complications for early detection and proper treatment.
Hematomas
A perivascular hematoma is the result of a local hemorrhage of an injured vessel into the adjacent soft tissue. Clinically, it presents as a nonpulsatile mass or ecchymosis at the puncture site. Gray-scale sonographic images of a perivascular hematoma show a softtissue mass with varying echogenicity in the inguinal area, adjacent to the femoral artery [4]. The echogenicity of a hematoma may vary depending on how long it has been hemorrhaging; therefore, it can be mistaken for a cyst or solid mass (Fig. 2). Sometimes, in cases where a hematoma is of an intermediate age, it may be difficult to detect because the border is unclear due to ill-defined infiltration and an isoechoic echogenicity that is similar to surrounding tissue (Fig. 3). Color and pulsed Doppler ultrasound examinations typically demonstrate no internal blood flow, which allows it to be definitively differentiated from a pseudoaneurysm [4]. A hematoma usually resolves in 2-3 weeks, although sometimes it can take much longer. Therefore, serial follow-up ultrasounds and a history of recent transfemoral approach may be helpful for distinguishing a hematoma from cysts or solid masses.
Pseudoaneurysm
A pseudoaneurysm, also known as a false aneurysm, is defined as a collection of blood that forms between one or two outer layers of an artery (media or adventitia). This is distinct from a true aneurysm, which involves of all three layers of the arterial wall. The trigger event is usually a laceration of the arterial wall due to trauma during cannulation. Although the clinical presentation of pseudoaneurysms varies depending on their size and location, including pain due to increased pressure from swelling or nerve compression, pulsatile masses with a thrill or murmur or groin expansion are the common clinical manifestations. The incidence of pseudoaneurysms is estimated to be 0.05%-0.50% of all patients treated with diagnostic and therapeutic percutaneous arterial and coronary catheterizations [5]. Despite the low incidence, pseudoaneurysms may cause significant morbidity due to an increased risk of rupture, thromboembolism, extrinsic compression of nearby neurovascular structures, or necrosis of overlying skin and subcutaneous tissue [1,5]. The risk factors for pseudoaneurysms are a lower femoral puncture site, larger sheath size, anticoagulation or antifibrinolytic therapy, older age, and arterial hypertension [5].
Gray-scale sonography can reveal a pulsatile anechoic saccular lesion with variable echogenicity, depending on the presence of an intraluminal thrombus. When there is no thrombus, it is anechoic; when there is a partial thrombus, it is echogenic but varies according to the age of the thrombus (Fig. 4). In addition, if the pseudoaneurysm is completely thrombosed, it may be difficult to differentiate from a hematoma. Real-time ultrasound images can reveal swirling or fluid-fluid levels within a pseudoaneurysm. Color Doppler imaging shows a bidirectional, turbulent, swirling blood-flow pattern known as the ŌĆ£yin-yangŌĆØ sign within a pseudoaneurysm. This sign is also noted in large aneurysms with a partial thrombus, because large aneurysms and pseudoaneurysms tend to thrombose, and blood may fill only part of the lesion [6]. Therefore, the sign is created when blood on one side of an aneurysm or pseudoaneurysm travels toward the probe (red-colored blood) and blood on the other side travels away from the probe (blue-colored blood) (Fig. 4). Although this sign is helpful in differentiating aneurysms or pseudoaneurysms from hematomas, cysts, or solid masses, it is not specific to partially thrombosed aneurysms or pseudoaneurysms because some neoplasms, such as solid and papillary neoplasms, also may show the yin-yang sign [6]. With spectral Doppler interrogation, the characteristic ŌĆ£to-and-froŌĆØ pattern in the communicating neck between the arterial vessel and pseudoaneurysmal sac is revealed (Fig. 5). The ŌĆ£toŌĆØ represents the arterial blood entering the pseudoaneurysmal sac during systole, while the ŌĆ£froŌĆØ represents blood flowing away from the pseudoaneurysmal sac during diastole [7].
Treatment options for pseudoaneurysms are observation, ultrasound-guided compression, surgical repair, and percutaneous thrombin injection. If a patient has a pseudoaneurysm that is 2 cm or smaller and is asymptomatic, observation is recommended to watch for spontaneous thrombosis [8]. Ultrasound-guided compression is used for effective compression of the tract connecting the native arterial lumen and the pseudoaneurysmal sac in asymptomatic patients who have a small pseudoaneurysm (usually less than 3.5 cm in diameter), because it has low complication rates and is cost-effective [9]. However, it is time-consuming and labor-intensive for the practitioners, and it is more likely to fail in patients undergoing anticoagulation therapy, with large or chronic pseudoaneurysms, and who have undergone a relatively long [9]. Surgical repair was the standard of care for pseudoaneurysms, but it usually required general anesthesia and resulted in perioperative complications, such as bleeding, wound infection, lymphocele, and radiculopathy [8]. Recently, percutaneous ultrasound-guided thrombin injection has become the treatment of choice for pseudoaneurysms because the technique is simple and has a high success rate of 96%, in comparison to the 74% success rate of ultrasound-guided compression [10]. A large neck diameter (>1 cm) is a relative contraindication for thrombin injection because of the higher risk of distal embolization. Under continuous ultrasound imaging, the thrombin is carefully injected in 0.1-mL increments using a thin-caliber needle (21-22G). The tip of the needle should be located in the sac, as far away from the neck as possible. Thrombi begin to form around the tip of the needle within a few seconds after thrombin injection, and then the remainder of the sac is progressively filled with thrombi (Fig. 6). When the pseudoaneurysm is filled completely, the color signal is no longer observed within the sac. During thrombin injection, it is very important that the native CFA should be assessed using ultrasound to avoid the risk of distal embolization.
Arteriovenous Fistula
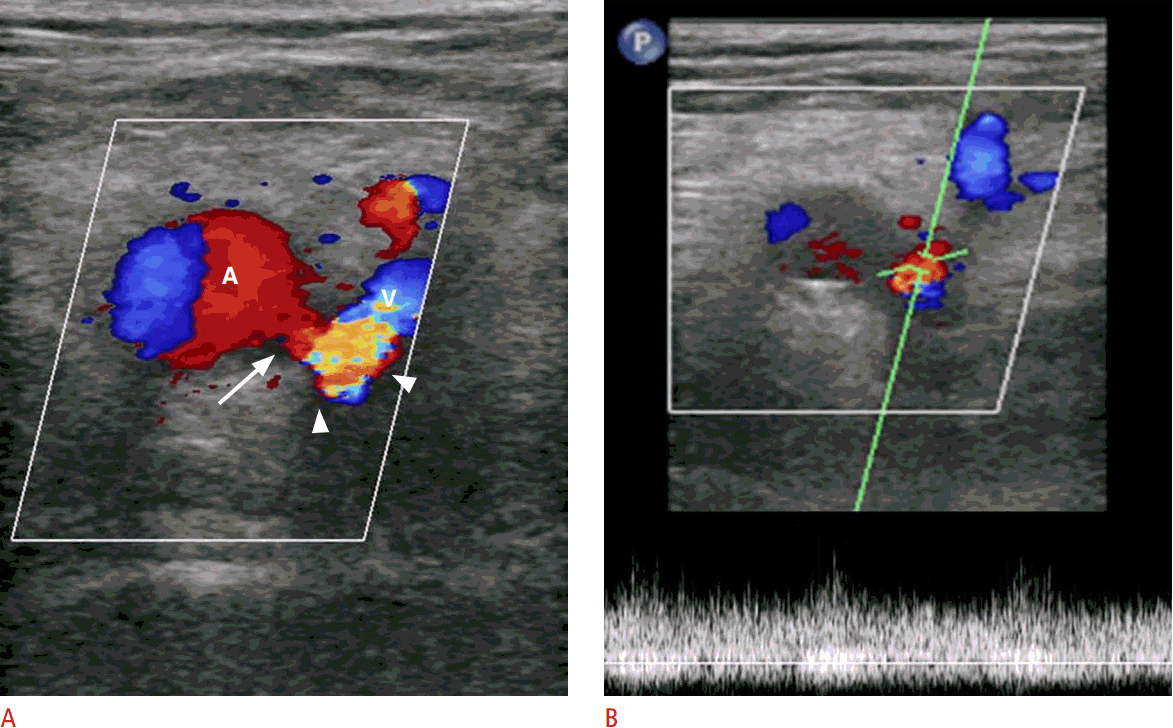
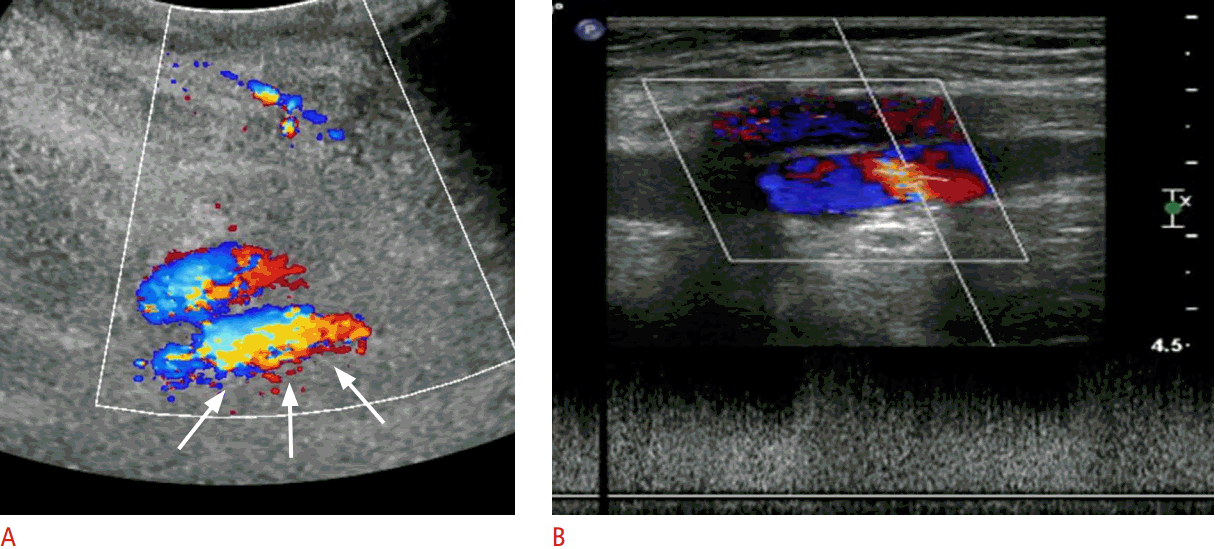
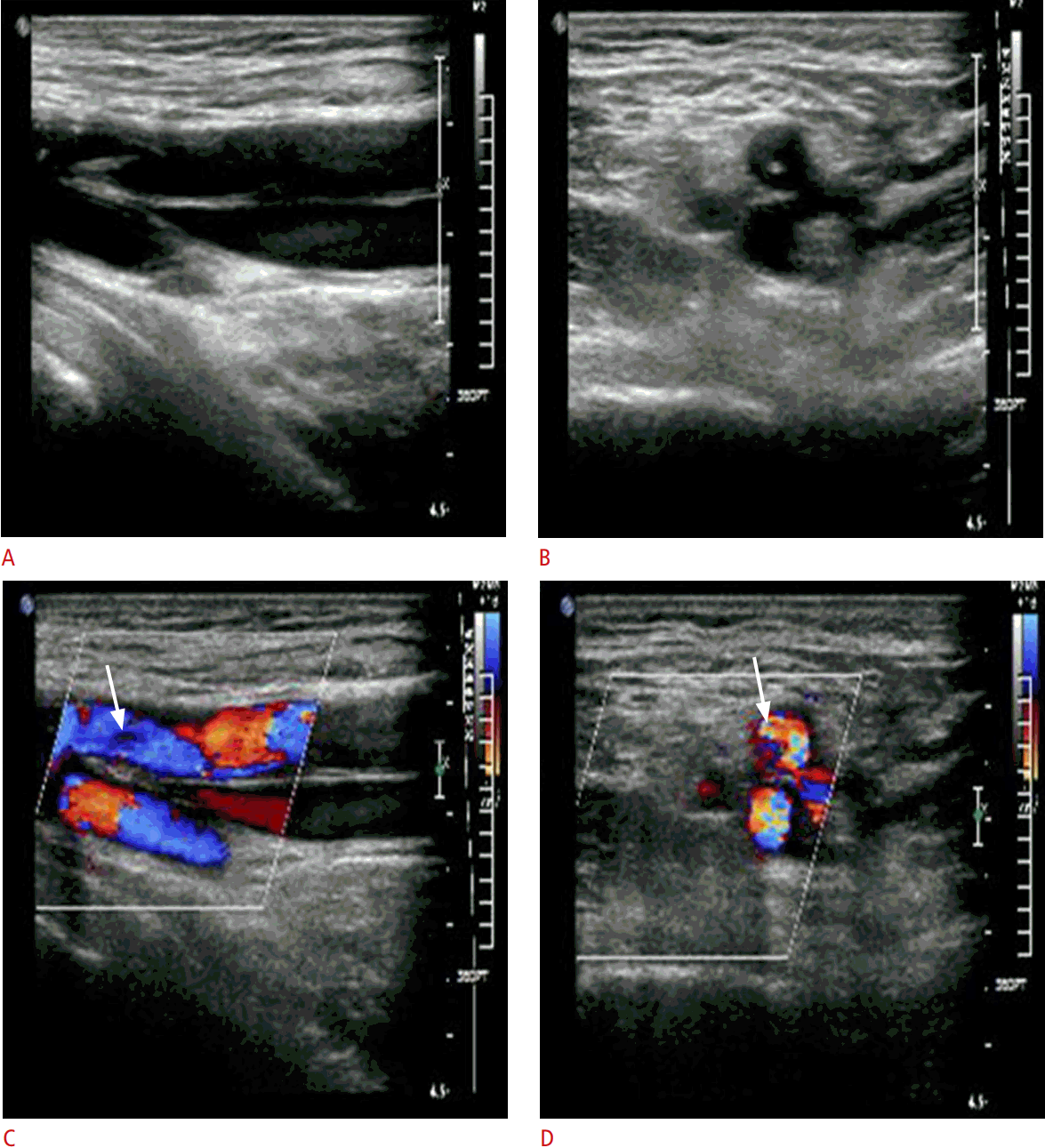
An AVF is a vascular channel connecting an artery with an adjacent vein that is created by simultaneous arterial and venous injury from needle tract trauma. Multiple puncture attempts, posterior arterial wall penetration, or the use of a large puncture needle increase the risk of an AVF [3,4]. Clinically, AVFs may present with a palpable thrill over the access site and an audible bruit. Unless the communicating tract between the artery and the vein is large, it is difficult to diagnose with gray-scale ultrasound. However, color Doppler with spectral sonography can show its characteristic features. The major diagnostic criteria of AVFs include a junction of low- and high-resistance flow in the supplying artery, a high-velocity arterialized waveform in the draining vein, and a turbulent high-velocity flow spectrum at the junction of the artery and the vein (Fig. 7). The minor diagnostic criteria of AVFs are visible direct communication between the artery and vein, a significant change in the diameter of the supplying artery, a focal point of venous dilatation, and a focal perivascular color artifact [11]. When the fistula is large enough to cause arterial steal, however, the flow in the distal artery may be reversed. The high-velocity flow may also create an adjacent softtissue color bruit characterized by perivascular speckling of color Doppler signals (Fig. 8). Rarely, an AVF may occur in association with a pseudoaneurysm (Fig. 9). Usually, the pseudoaneurysm is initially created at the arterial puncture and then a second channel is created by the needle passing through the pseudoaneurysm and the adjacent vein, resulting in an AVF [4].
The management of an AVF is determined by the symptom or size of the AVF. Patients with a small AVF who are asymptomatic should be observed, as they are prone to spontaneous occlusion. Other treatments are ultrasound-guided compression, endovascular repair, and surgical ligation.
Femoral Artery Dissection
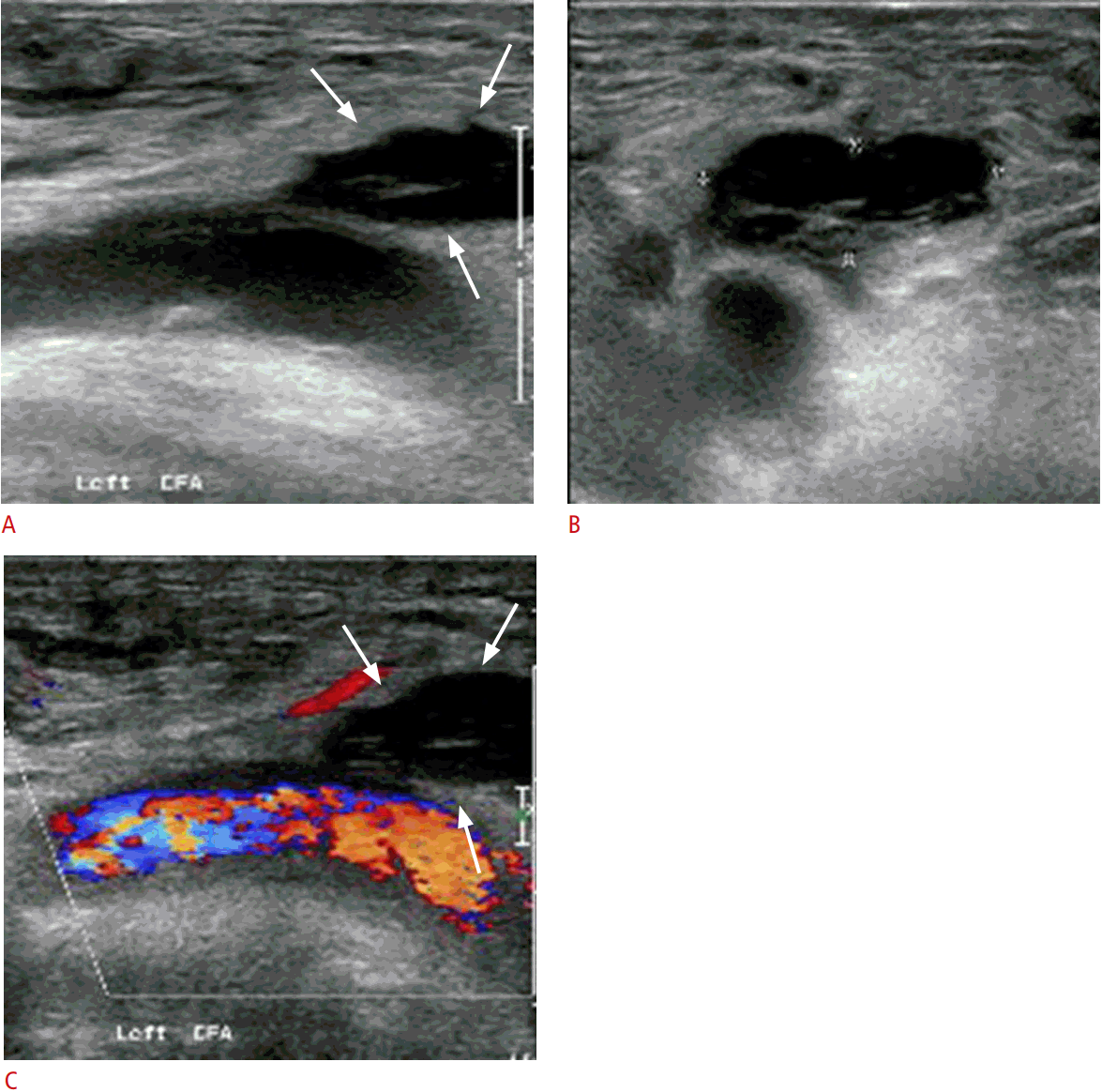
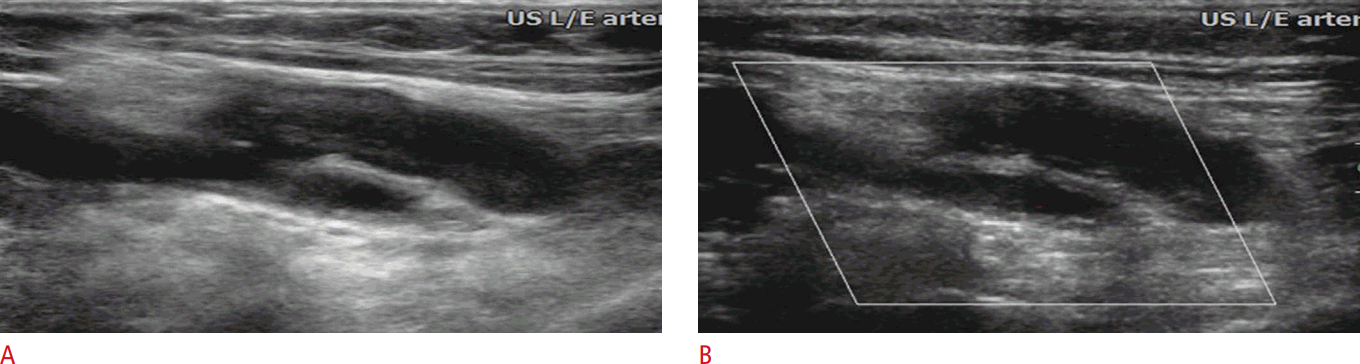
Dissections occur when a wire or catheter enters the subintimal space and creates a false lumen. Its incidence was approximately 0.1%-0.4% in patients who underwent cardiac catheterization [12]. Gray-scale ultrasound can reveal an echogenic dissection flap representing the dissected intimal layer of the arterial wall that may be found centrally within the lumen (Fig. 10). Color Doppler can show the parallel blood-flow channel that separates the true and false lumen. If the false lumen is filled by a thrombus, it is not distinguishable from an intramural hematoma or plaque. The majority of non-flow-limiting dissections can be clinically observed and will spontaneously resolve. If there is a flow-limiting dissection or associated limb ischemia, surgical repair can be performed, such as patch angioplasty or endarterectomy [12].
Arterial Thrombus/Occlusion
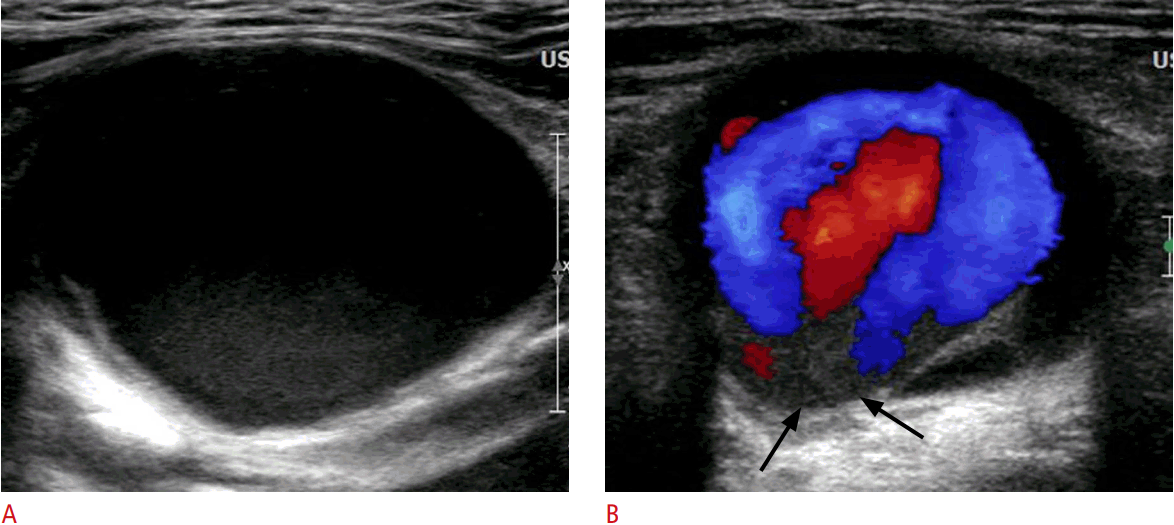
Up to 3% of patients who undergo transfemoral arterial interventions will experience angioplasty-site thrombosis. Ultrasound images of such thrombi show various degrees of echogenicity and internal complexity, along with an absence of color flow (Fig. 11). In a chronic thrombus, the diameter is small and there is a heterogeneous echogenic wall. Except when contraindicated by active hemorrhage, recent major surgery, or stroke within the past 6 months, thrombolytic treatment includes the use of streptokinase, urokinase, or low-molecular-weight heparinization [13].
Retroperitoneal Hemorrhage
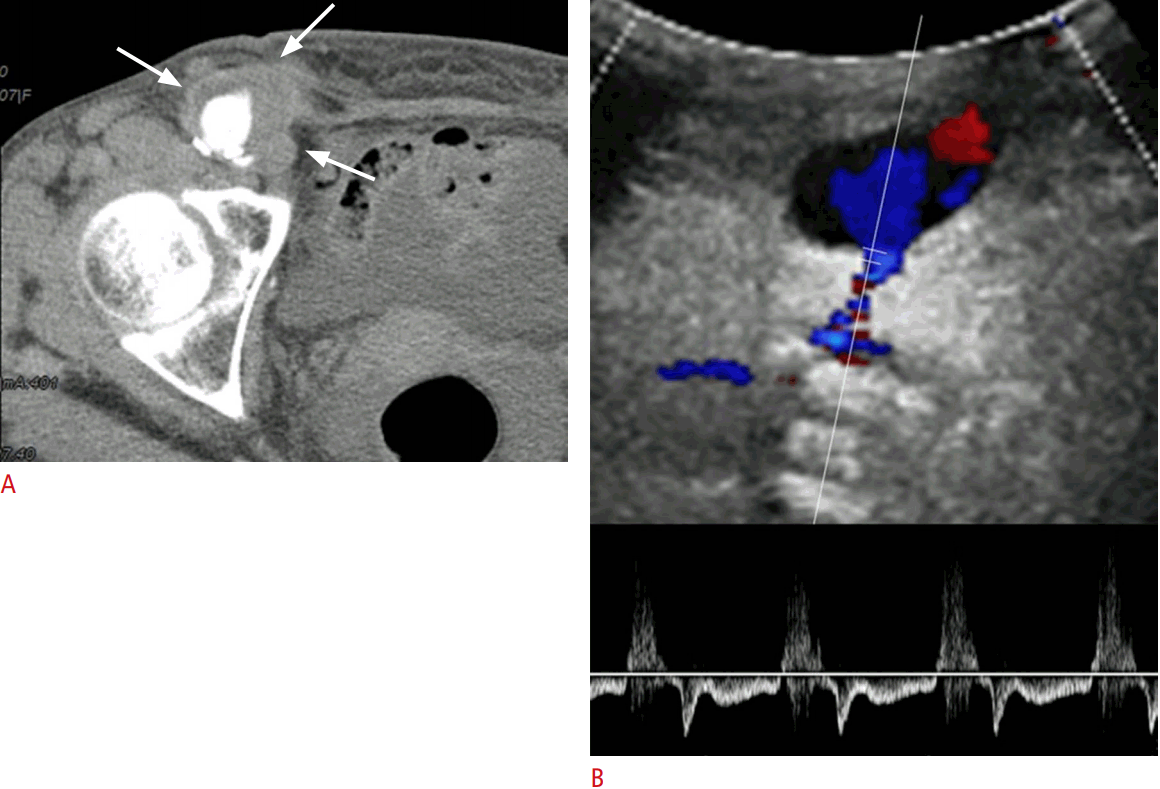
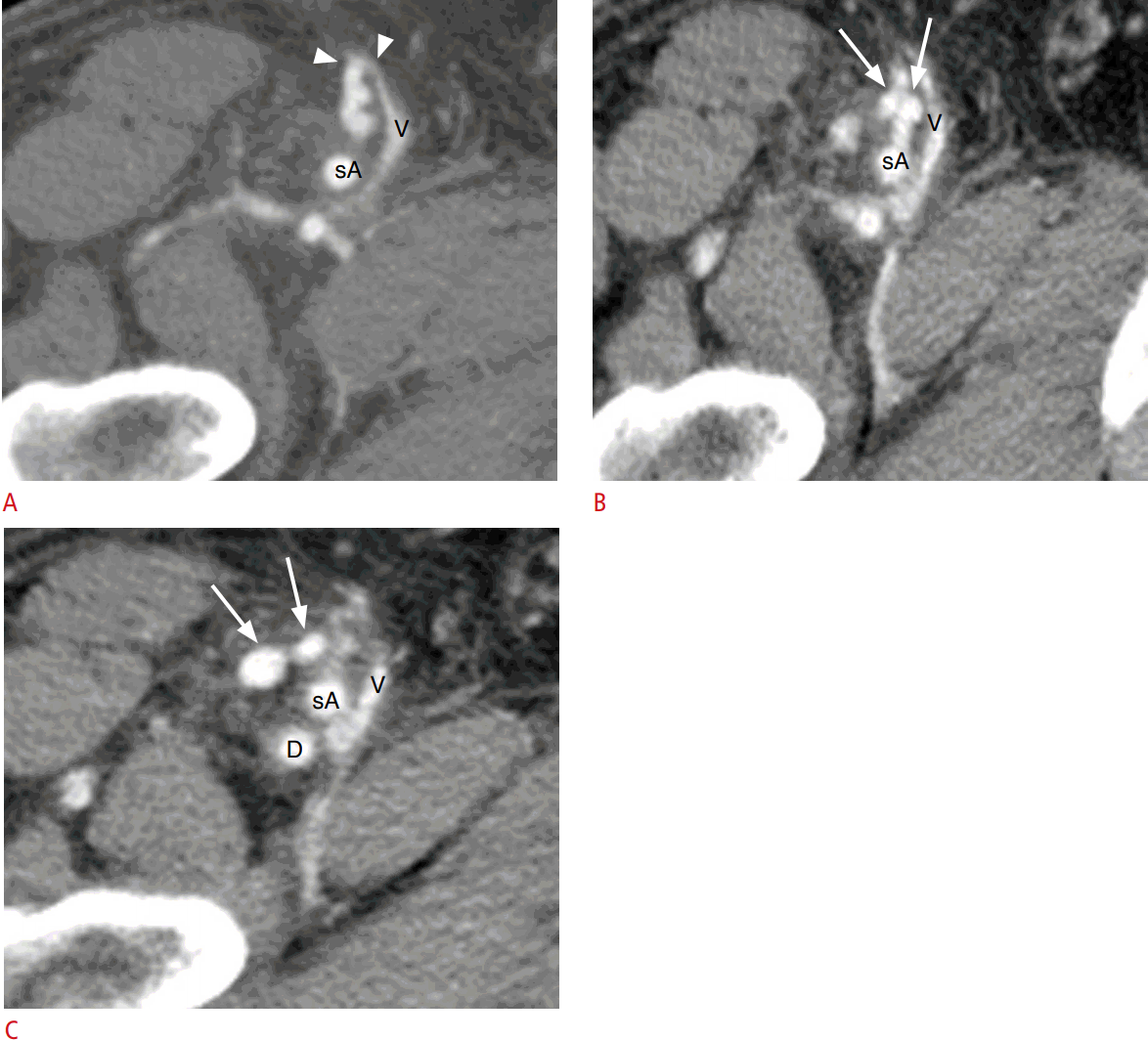
Retroperitoneal hemorrhage is very rare, with an incidence of 0.15%-0.5% in patients who undergo cardiac catheterization; however, its mortality rate (6.6%) is high [14]. The risk factors relevant to retroperitoneal hemorrhage are anticoagulation, hypertension, a higher femoral arterial puncture site, and use of larger sheath sizes. It should be suspected when there is serial decrease in hemoglobin and clinical symptoms such as dizziness, orthostatic hypotension, and ipsilateral flank pain [14]. For the detection of retroperitoneal hemorrhage, computed tomography (CT) is more sensitive than ultrasound because the retroperitoneal space may limit the field of the echo window (Fig. 12). CT can successfully reveal the location of the bleeding, the extent of the hematoma, and other associated traumatic conditions. Although the majority of cases respond to conservative management, endovascular coil, Gelfoam embolization, or surgical repair may be required to control active bleeding [15].
Conclusion
All patients undergoing femoral arterial puncture should be promptly evaluated for potential complications because significant hemodynamic deterioration from bleeding or an AVF can lead to deleterious outcomes. Duplex ultrasound is useful for the initial evaluation of femoral puncture-related vascular lesions, because it can provide anatomic and hemodynamic information at the same time. Using color Doppler ultrasound, complications such as hematoma, pseudoaneurysm, and AVF can be distinguished. In addition, ultrasonography plays an important role in the guidance of thrombin injections, resulting in high efficacy of the procedure and reduced complications. Therefore, radiologists should be aware of the characteristic ultrasonographic findings of complications related to transfemoral arterial procedures in order to provide the proper treatment.



 Print
Print facebook
facebook twitter
twitter Linkedin
Linkedin google+
google+




 Download Citation
Download Citation PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC




