Introduction
With improvements in ultrasound technology, particularly in the development of a newer generation of machines that work with high- and variable-frequency probes, ultrasonography has become increasingly useful for imaging superficial structures. Ultrasound has the capability of distinguishing skin layers, and therefore, can be used as a tool to evaluate cutaneous pathologies. In recent years, the applications of ultrasonography in dermatology have been growing [1,2]. The vulva, which consists of the mons pubis, labia majora, labia minora, clitoris, and the vestibule containing the urethral meatus and the vaginal opening, can be affected by a wide variety of dermatological conditions, some of which are unique to this area. The application of high- and variable-frequency ultrasound increases the degree to which common vulvar lesions can be identified and characterized with regard to their location, size, vascularity, and content. To our knowledge, very few articles in the literature have described the clinical applications of ultrasound in evaluating vulvar lesions, except in relation to the assessment of the supporting structures, incontinence, and pelvic organ prolapse. This pictorial essay serves as an introduction to the relevant sonographic techniques and the normal anatomy of the vulvar skin, and provides an illustration of certain vulvar entities that the author has recently encountered and evaluated sonographically. This overview will help promote physicians’ interest in using ultrasound on the vulva, with the ultimate aim of evaluating whether this imaging modality can be clinically applicable for the evaluation of common vulvar conditions.
Scanning Techniques
Ideally, as in other dermatologic applications, high- and variable-frequency transducers working with upper frequencies of 15 MHz or higher are recommended [1]. A lower-frequency transducer can be used, but the definition of skin layers may be suboptimal. The scanning techniques for the vulva are similar to those that have been described for skin lesions on other parts of the body [1]. However, the vulva is in a peculiar location and acoustic gel can slide off quickly despite multiple applications. Scanning needs to be quick with occasional gel replacement over the involved area. No or only minimal pressure should be applied on the skin to avoid distortion of the vulvar structures. The greyscale examination of a lesion should be carried out in at least two perpendicular planes, followed by color Doppler imaging if necessary. If the target lesion is identified, an evaluation of the echogenicity patterns, measurement of its size, identification and measurements of the blood flow (distribution, type, and maximum peak systolic velocity of the arterial vessels), and localization, particularly in relation to the skin layers, should all be reported.
All images shown in this article were obtained using the Samsung Medison Accuvix XG System (Samsung Medison Co., Ltd., Seoul, Korea) with a variable linear transducer with an upper frequency of 13 MHZ.
Sonographic Anatomy
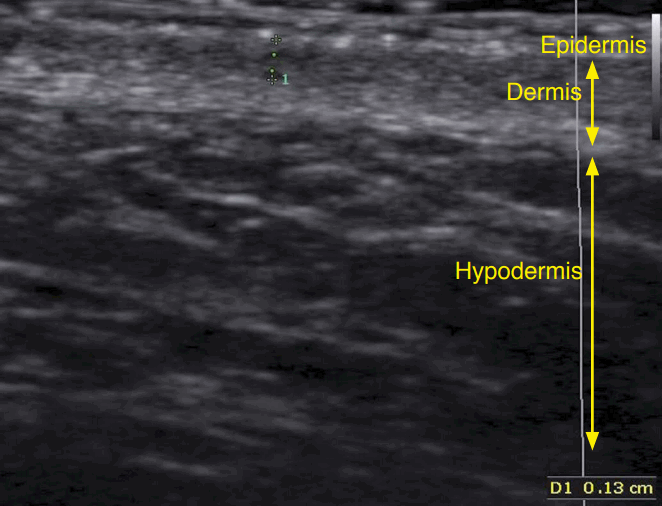
The skin is composed of three layers: the epidermis, dermis, and hypodermis (also known as subcutaneous tissue). On 2-dimensional greyscale sonography, the echogenicity of each layer depends on its main component: keratin in the epidermis, collagen in the dermis, and fat lobules in the subcutaneous tissue [1]. The epidermis usually appears as an echogenic line (Fig. 1) [1]. However, because the vulvar skin has various degrees of keratinization, from keratinized epithelium on the labia majora to non-keratinized epithelium on the labia minora, the echogenicity of the epidermis on the vulva can vary. In areas with a thicker corneous layer, such as the medial aspect of the labia minora, the epidermis may appear as a bilaminar parallel hyperechoic structure (Fig. 1).
The dermis appears as a hyperechoic band, less bright than the epidermis (Fig. 1). As the collagen content in the vulva can vary, particularly depending on the patient’s age, the echogenicity and thickness of the dermis can also be variable [3]. The identification of this layer is also difficult, as the vulvar structures are compacted and the overlying skin is generally wrinkled. Beneath the dermis, fatty lobules provide the main source of echogenicity of the hypodermis, which is mostly hypoechoic and contains hyperechoic strands of fibrous septa (Fig. 1).
Three-dimensional volume reconstruction and color and/or power Doppler ultrasound can be performed selectively to improve the image or highlight the vascularity.
Vulvar Lesions
Bartholin Cyst and Abscess
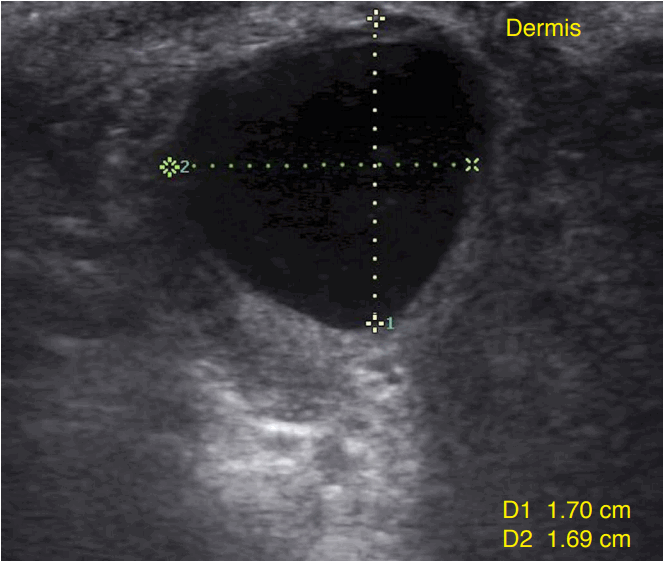
Bartholin cyst is the most common cystic lesion of the vulva, and arises from cystic dilatation of an obstructed Bartholin duct. This cyst is usually seen as a unilateral, fluctuating structure at the posterior third of the labia majora and contains clear mucous fluid. Sonographically, this cyst is located in the hypodermis with intact epidermis and dermis. It appears mostly anechoic to hypoechoic due to predominant fluid content, with a well-defined cyst wall. Echo enhancement is frequently seen posterior to the cyst due to increase through transmission of the cyst content (Fig. 2) [4].
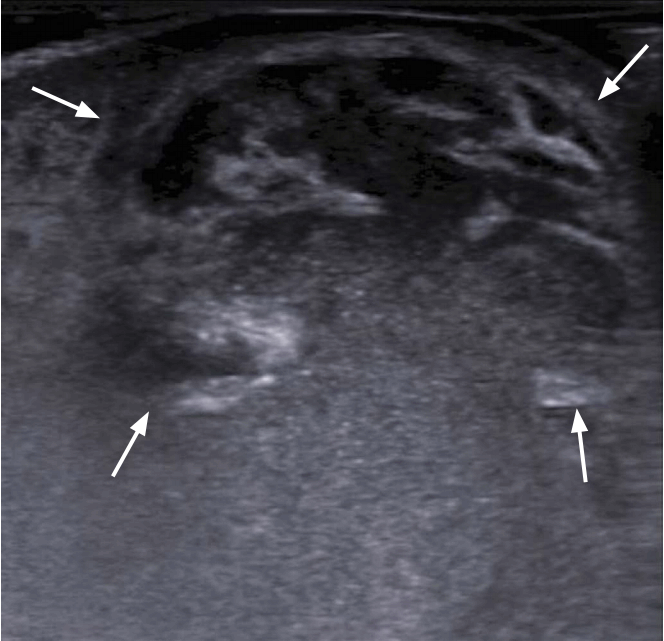
When infected, the overlying skin appears red and becomes tender on palpation. The cyst wall contains pus instead of clear fluid, and the sonographic appearance is a collection of echogenic fluid, occasionally containing septa and sediment. The cyst wall may become echogenic with less well-defined borders due to the inflammatory response of the adjacent tissue (Fig. 3) [5].
Epidermal Cyst
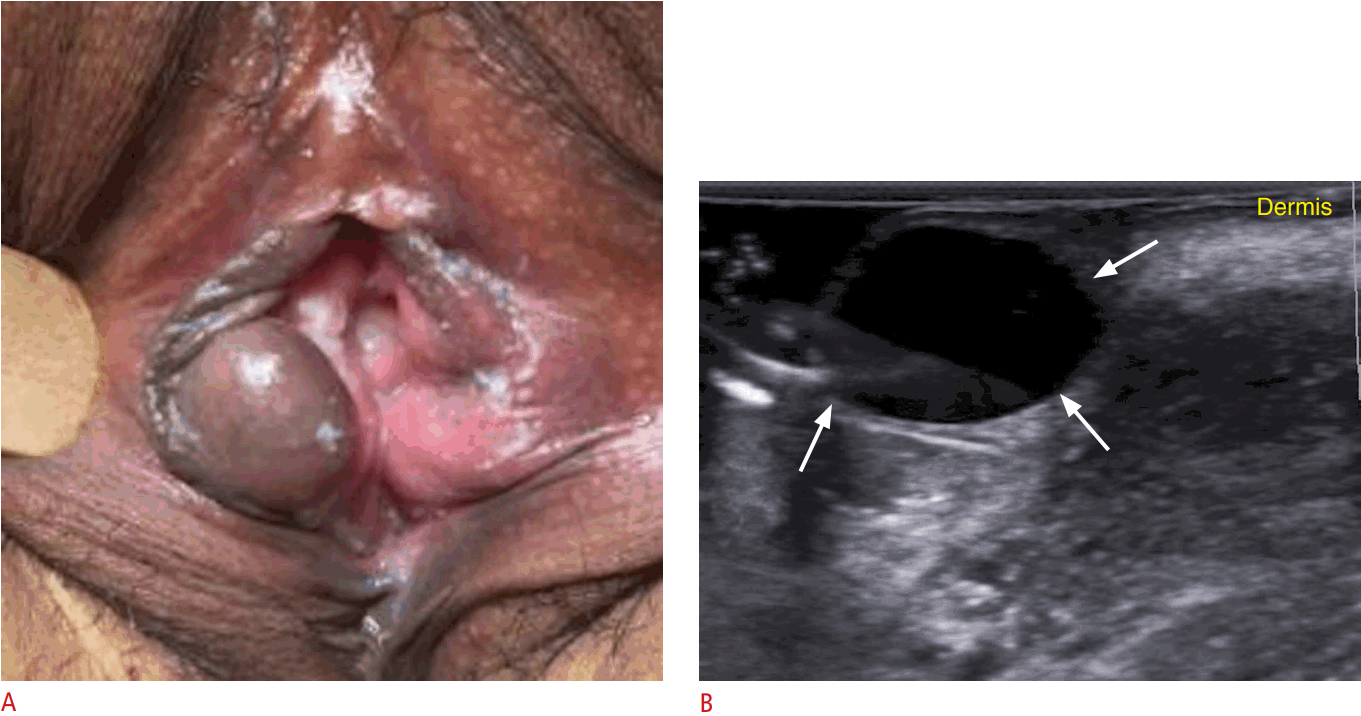
An epidermal cyst is derived from the entrapment of epidermal components in the dermis and hypodermis (Fig. 4A). On ultrasonography, these cysts appear as well-defined, oval or round, anechoic or hypoechoic structures located in the dermis and hypodermis, frequently with a posterior acoustic enhancement artifact (Fig. 4B).
Hemangioma
Resulting from the abnormal proliferation of blood vessels, hemangiomas are commonly found in the skin and subcutaneous tissue. However, their occurrence in the female genital tract is rare [7]. Clinically, hemangiomas appear as multiple purple-blue swellings (Fig. 6A). Color Doppler ultrasound shows tortuous vessels with multidirectional, turbulent blood flow (Fig. 6B), which can also help to delineate the extent of the lesion.
Angiomyofibroblastoma
Angiomyofibroblastoma is a benign mesenchymal soft tissue tumor that occurs predominantly in the vulvar region of middleaged women. However, it can also occur in the vagina, cervix, and retroperitoneum [8]. It is a well-circumscribed, elastic, soft subcutaneous tumor and is usually less than 5 cm in diameter. Sonographically, it is described as a well-demarcated soft tissue mass with non-homogeneous mixed echogenicity, comprising an echogenic hypocellular myxoid stroma interspersed with irregular hypoechoic areas of hypercellularity (Fig. 7) [9]. Occasionally, multiple variable-sized cystic lesions within the mass can be seen, corresponding to dilated glands in the vulva. Color Doppler ultrasonography shows no vascularity within the mass [9].
Soft Tissue Infection
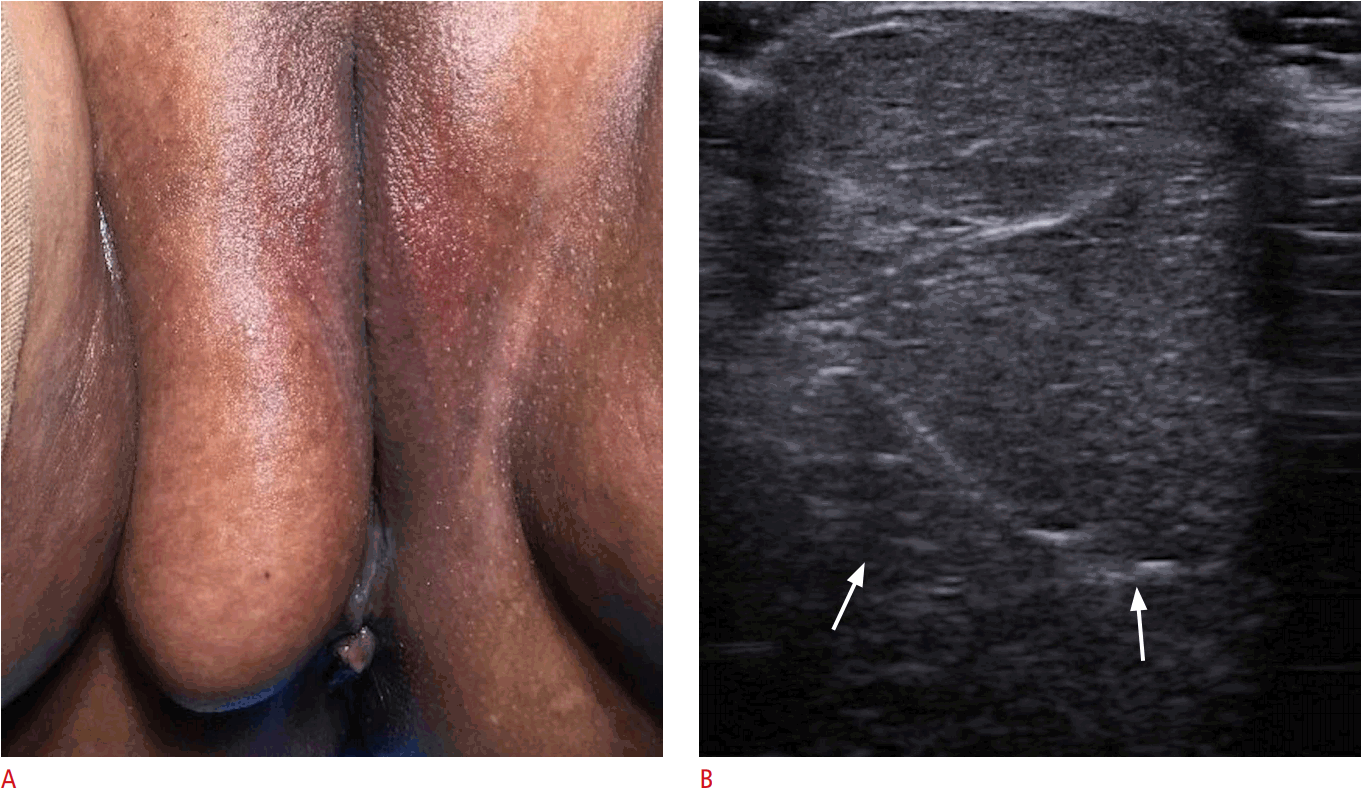
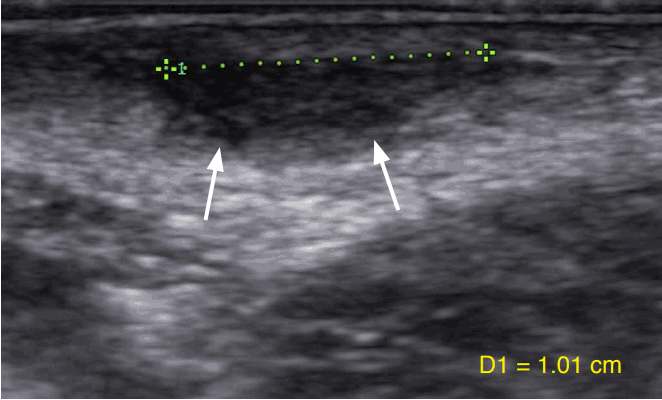
The distinction between vulvar abscess and cellulitis is important, because the treatment of these conditions is different. This condition is commonly seen in the emergency department where point-ofcare ultrasound may help in making the correct diagnosis [10]. Fig. 8 is a sonogram from a 31-year-old woman who presented with an approximately 1-cm tender lesion over the right labia majora. Ultrasound favored the diagnosis of cellulitis rather than an abscess, and the lesion was therefore successfully treated with antibiotic therapy, without the need for drainage.
Conclusion
Many different dermatological and gynecological entities can occur on the vulva. The vulvar lesions that are described in this article only represent those encountered by the author, and this review is clearly not exhaustive. Ultrasonography can play a helpful role in the evaluation of benign vulvar lesions, particularly when unfamiliar lesions are encountered. Ultrasonography can assist in determining the location, depth of involvement (particularly in relation to the skin layers), exact size, contents, and vascularity of a lesion. It is also useful for monitoring such lesions when they are managed nonsurgically. Therefore, this review provides background information on the application of ultrasonography for the evaluation of vulvar lesions, with the inclusion of basic guidelines on the relevant techniques and normal ultrasonographic anatomy. This review promotes physicians’ awareness of the ultrasonographic appearance of various vulvar conditions, with the goal of increasing physicians’ interest in and utilization of ultrasonography for the evaluation of vulvar conditions.



 Print
Print facebook
facebook twitter
twitter Linkedin
Linkedin google+
google+


 Download Citation
Download Citation PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC




