Introduction
The spleen is frequently involved in both blunt and penetrating trauma, accounting for 45% of all visceral injuries [1,2]. Falls onto bicycle handlebars represent a common cause for splenic trauma, particularly in the paediatric population [3]. Imaging with both ultrasonography (US) and computed tomography (CT) plays an important role in both the initial evaluation and the follow-up of such patients [4,5]. CT is the well-established ŌĆ£gold standardŌĆØ for the initial assessment of splenic injuries and an excellent modality to document the healing process [5]. However, as follow-up with CT is not routinely recommended, US may play a potential role in monitoring the healing process of the spleen [6]. Taking into consideration its wide availability, low cost, and lack of radiation, US is a valuable modality to follow-up splenic trauma. Here, we report a case of a splenic injury in a patient with underlying splenomegaly and discuss the serial changes on US throughout the healing process.
Case Report
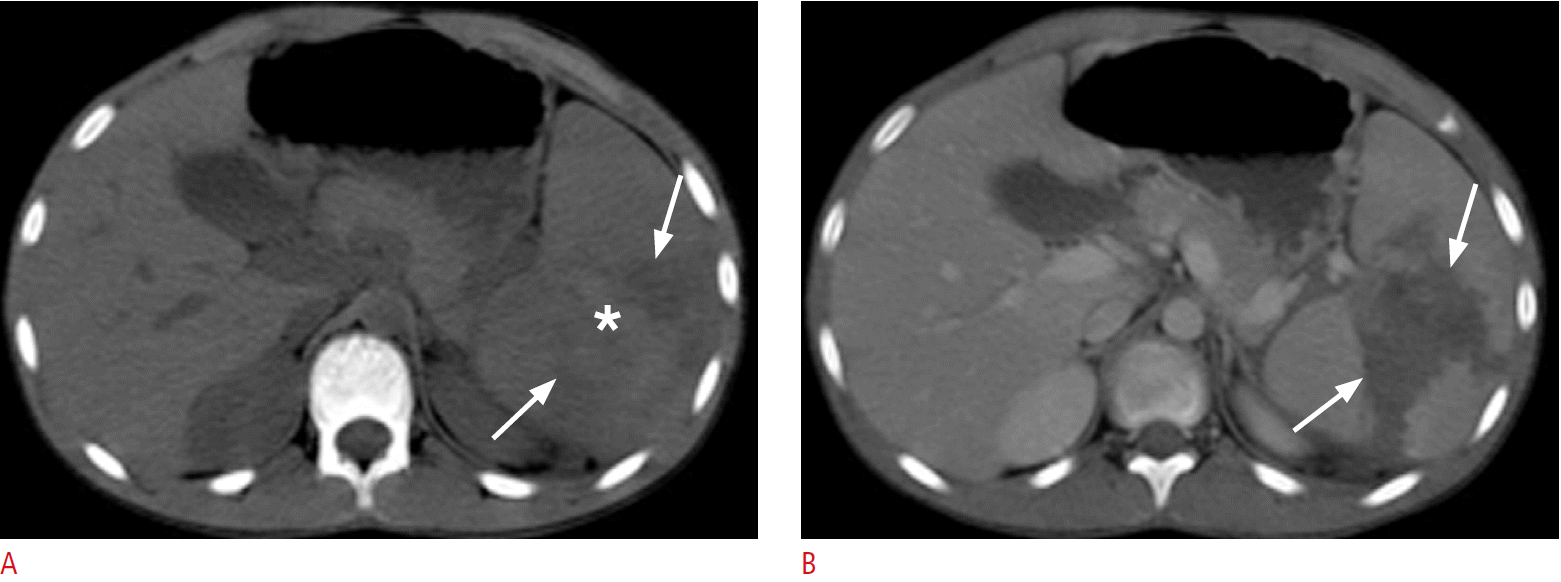
A 14-year-old boy presented to the Emergency Department of our hospital complaining of left upper quadrant pain after an accident during which he fell onto his bicycleŌĆÖs handlebars. The boyŌĆÖs past medical history included splenomegaly due to thalassemia. As the boy was hemodynamically stable, he was initially referred for CT of the upper abdomen. This examination was performed using a 4-slice CT scanner (Asteion, Toshiba Medical Systems, Otawara, Japan) and revealed the presence of a large intraparenchymal hematoma which was centrally located in the enlarged spleen with mixed attenuation density, suggesting different ages of hemorrhage along with a small perisplenic fluid collection on the unenhanced CT. In the enhanced CT, the normal splenic parenchyma was homogeneously enhanced (59 Hounsfield units [HU] before and 114 HU after the contrast administration), whereas the hematoma did not show any enhancement (Fig. 1). The splenic injury was classified as type III according to the American Association for the Surgery of Trauma (AAST) classification [2]. Conservative treatment was decided with US follow-up.
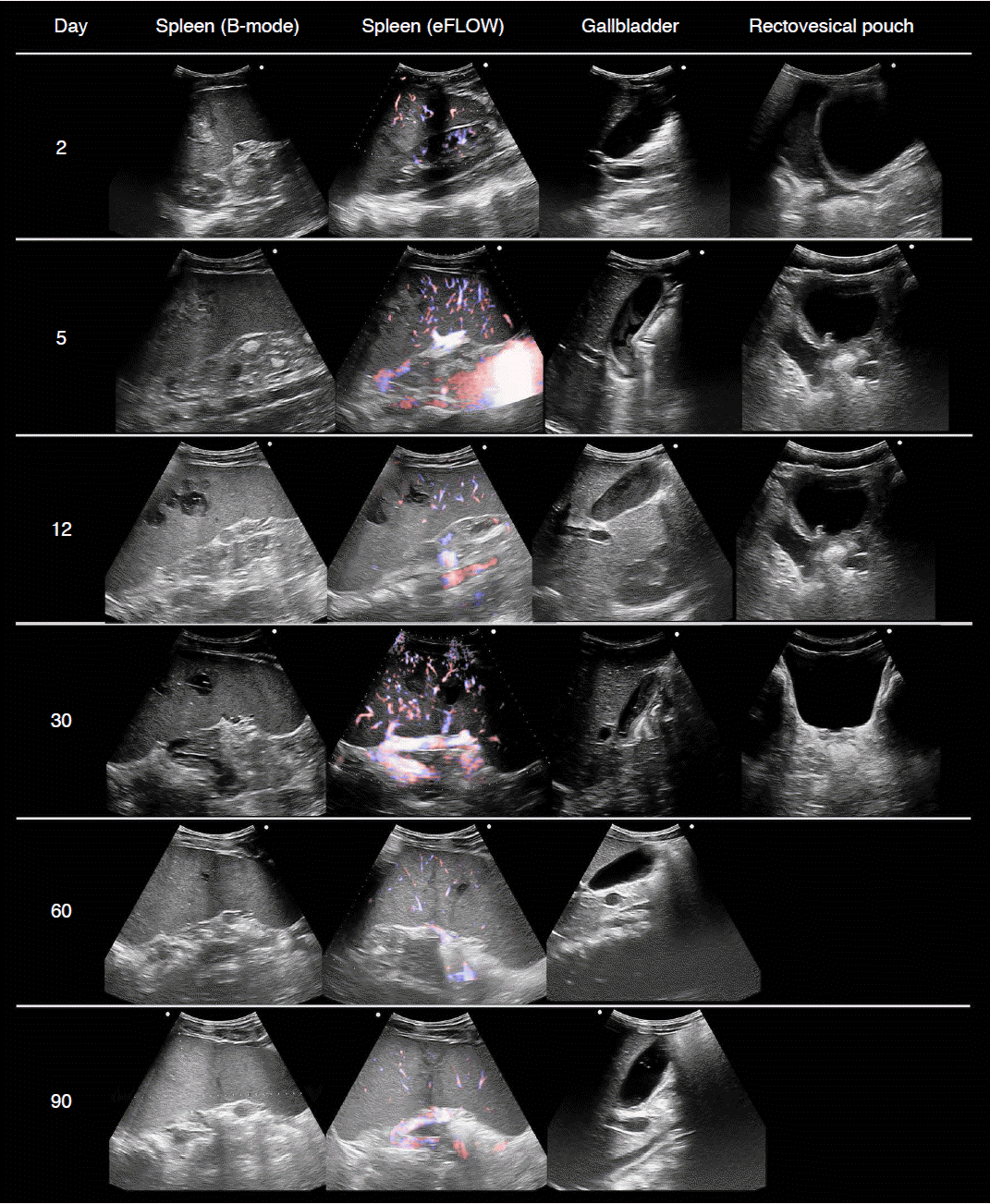
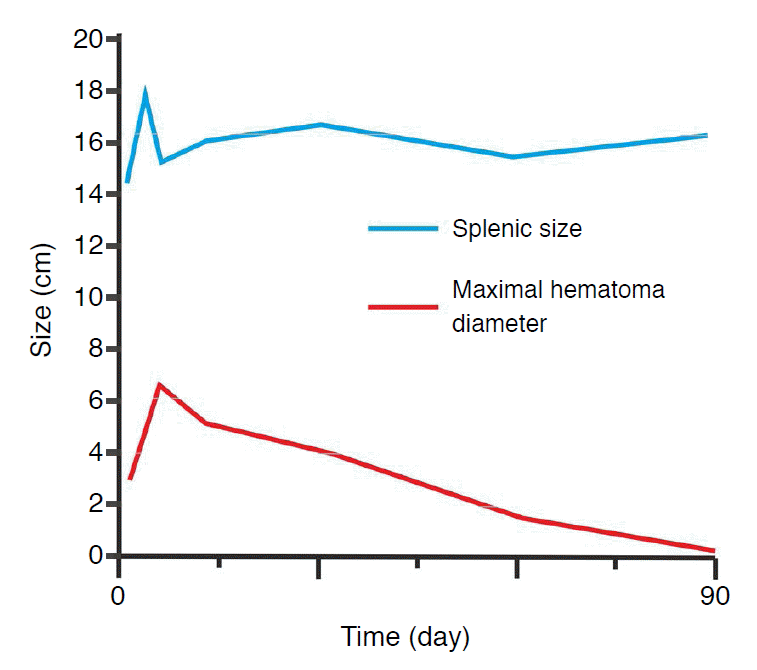
All the US examinations were performed by the same experienced radiologist with a Prosound Alpha 7 device (Aloka GmbH, Meerbusch, Germany) and a 2-6-MHz convex abdominal multifrequency probe. The directional eFLOW technique was used to demonstrate blood flow with enhanced spatial resolution and greater detail. The spleen size was constantly measured on the organŌĆÖs longitudinal axis. On the initial CT scan, the spleen was 14.3 cm in size, and the hematoma was 3 cm├Ś2.8 cm in size. On the second day, US demonstrated an enlarged spleen with a longitudinal diameter of 17.7 cm and a rounded accessory spleen with a diameter of 1.4 cm situated near the splenic hilum. There was an intraparenchymal heterogeneous hyperechoic area which represented the hematoma, measuring 5 cm├Ś3.5 cm. No blood flow signals were identified within the hematoma with the directional eFLOW technique, suggesting an interruption of the vascular flow. The gallbladder was free of echogenic material. There was also fluid collection in the rectovesical pouch. On the fifth day, the estimated size of the spleen and of the hematoma was 15.2 cm and 6.1 cm, respectively. The hematoma was characterized by a patchy hyperechoic echostructure, compared with the adjacent splenic parenchyma. The directional eFLOW technique revealed no blood flow signals within the hematoma. The gallbladder was imaged and found to contain echogenic sludge. The rectovesical fluid collection was significantly decreased. On the 12th day, the hematoma became hypoechoic and the gallbladder was full of bile sludge. No fluid collection was detected except for a small collection near the cecum. On the 30th day, the hematoma was further reduced (3.8 cm├Ś3.9 cm) and was anechoic, while the rectovesical fluid collection resolved completely. Two months after the accident, the hematoma measured 1.3 cm and there was evidence of gallbladder microlithiasis as the previously detected gallbladder content disappeared. The final follow-up US, 3 months after the accident, showed no evidence of the hematoma, while the gallbladder contained nothing but few fine echogenic foci. All the aforementioned ultrasonographic changes can be seen in Fig. 2. The evolution of US-estimated dimensions of the spleen and the hematoma can be seen in Fig. 3.
Discussion
The spleen is the second most frequently traumatized abdominal organ in the cases of blunt trauma, following the liver [2,7]. Because of its protected position in the left hypochondrium, the spleen is less affected by penetrating trauma than the liver and the other abdominal organs. However, patients with splenomegaly due to anemia like the one discussed above are more vulnerable to splenic trauma. Causes of splenic trauma include motor vehicle and motorcycle collisions, assaults, falls, and many sports activities like cycling [2]. Falls onto bicycle handlebars usually affect male children and are considered to represent a serious mechanism of trauma as they may result in injuries of parenchymal organs like the spleen in 20%-37% of the cases and gastrointestinal perforation in 21% of the cases [3]. Splenic trauma is usually characterized as lacerations or hematomas and classified according to the AAST classification, on the basis of CT findings [2]. However, this grading system is poorly correlated with the patientŌĆÖs outcome and the decision of surgery [7]. Once clinical examination and assessment of hemodynamic stability are performed, the patient can be referred for imaging studies.
Typical US findings of splenic trauma include traumatic fissures (hyperechoic or hypoechoic), subcapsular or intraparenchymal hematomas, and free fluid collections. Intraparenchymal hemorrhage may be either hyperechoic or complex in echogenicity. A hematoma may be hyperechoic when acute or of various echogenicities when organised. Pseudoaneurysms can be easily detected with the colour Doppler technique, which in normal spleen reveals diffuse uninterrupted vascular flow. However, US of the spleen may miss some cases of acute rupture [1]. A grading system of splenic trauma was designed on the basis of colour Doppler findings [4]. CT is 96% sensitive and specific in the visualization of a direct splenic injury and thus, represents the modality of choice for hemodynamically stable patients and patients with restored stability after resuscitation [2]. Regarding CT findings of splenic trauma, the term laceration refers to an irregular hypodense area with indistinct margins, which is not enhanced after contrast medium administration. Subcapsular hematoma is identified as a regular hypodense collection which is crescentic in shape and follows the splenic margin. The underlying parenchyma may be deformed or indented. Intraparenchymal hematomas appear broader; irregularly shaped; and hypodense, isodense, or even hyperdense and cause enlargement of the spleen and mass effect. The surrounded splenic parenchyma enhances after contrast administration. Hematomas may take more than a month to resolve [2,5,8]. During the first 48 hours after splenic trauma, hematomas may be hyperdense or isodense to the splenic parenchyma. During the next month, hematomas become gradually hypodense and smaller in size, while their margins may become sharper. This evolution of imaging findings is attributed to the lysis of the blood clot and the resorption of the protein contents and may last for several months. When a hematoma fails to completely resolve, a chronic splenic pseudocyst may develop, containing serous fluid [5]. In the case report presented, we documented the healing process of the spleen with US and yielded findings similar to those reported with CT. Namely, an initially hyperechoic splenic hematoma gradually became hypoechoic and anechoic and finally resolved completely.
Hemoperitoneum is another important CT finding of splenic trauma. Blood can be found in the perisplenic space, in the right upper quadrant, or in the left paracolic gutter and the pelvis. While the volume of hemoperitoneum is considered to predict the need for surgical treatment, recent publications have documented successful conservative treatment in patients with large blood collections [8]. The resolution of the fluid collection after splenic trauma takes 2-4 weeks [5]. In our case, the fluid collection disappeared after 2 weeks.
Follow-up imaging is valuable to document the healing process of the spleen, which may last up to 3 months. As this information does not alter management when healing is uneventful, the use of CT for follow-up purposes is not recommended [8]. Lyass et al. [6] concluded that follow-up radiological studies can be safely omitted in patients with splenic trauma grades I to III and hemodynamic stability. As discussed in the present case report, US with either B-mode or blood flow imaging techniques like colour Doppler, power Doppler, or directional eFLOW provides a useful alternative to CT when it comes to the follow-up of splenic trauma.
Regarding the formation of gallbladder sludge in our patient, we believe that it may have been caused by the hemolytic hyperbilirubinemia which occurred during the nonsurgical management of the splenic hematoma [9].
In conclusion, blunt abdominal trauma resulting in a spleen injury is a frequent clinical scenario with a variety of imaging findings on both US and CT. Despite the superiority of CT over US in terms of diagnostic accuracy in the initial evaluation of the traumatized spleen, US represents a valuable tool in the follow-up of conservatively treated patients, particularly in the paediatric population. In this case report, we presented the US findings of a splenic hematoma and the other associated findings throughout the healing process.



 Print
Print facebook
facebook twitter
twitter Linkedin
Linkedin google+
google+
 Download Citation
Download Citation PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC




