Introduction
Percutaneous cystostomy is an alternative procedure to be considered when urinary bladder catheterization is needed, but urethral catheterization is contraindicated or unsuccessful. Bedside ultrasound-guided percutaneous cystostomy for infants in the neonatal intensive care unit is not commonly performed and is not well documented in the literature [1-3]. We report a case of ultrasound-guided percutaneous cystostomy performed as a bedside procedure for an infant in the neonatal intensive care unit.
Case Report
An infant born at 39 weeks of gestation, weighing 2,785 g and 47 cm in length, underwent an arterial switch operation for transposition of the great arteries with an intact ventricular septum, closure of a patent foramen ovale, and division of a patent ductus arteriosus on the fifth day of life. A FoleyŌĆÖs catheter was inserted on the day of the operation. Hematuria was noted soon after the insertion of the FoleyŌĆÖs catheter, and the catheter was removed. In light of the suspected urethral injury, percutaneous cystostomy was considered to enable urinary drainage. Blood test results were normal, including a complete blood count, tests of liver and renal function, and the clotting profile.
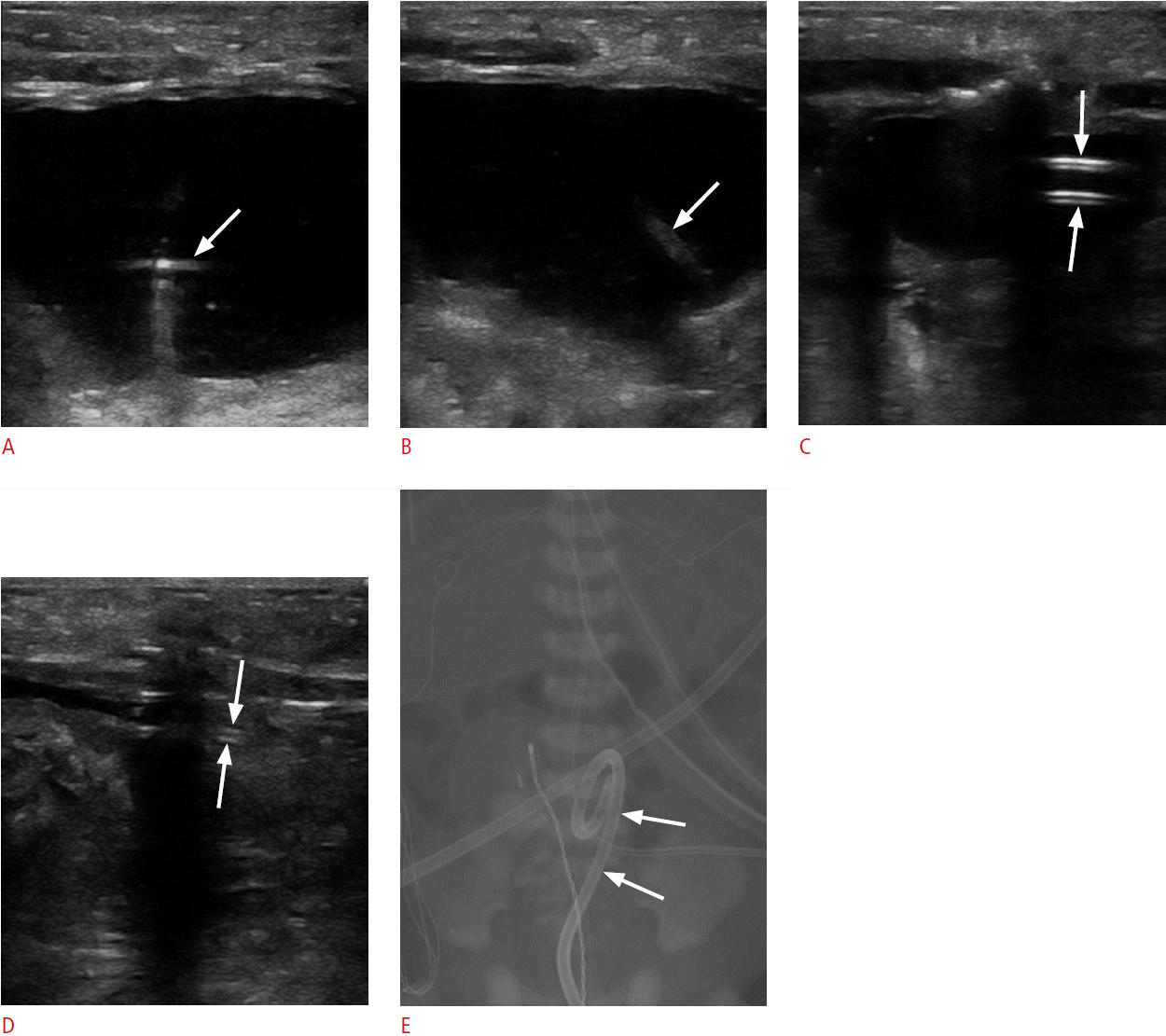
As the infant was unfit for transfer to the interventional radiology suite, the procedure was performed at the bedside with the infant in the incubator in the neonatal intensive care unit. Preliminary bedside ultrasonographic examination showed a distended urinary bladder. After planning the most direct route for percutaneous access to the bladder, the infant was prepared and draped in a sterile manner. Before the procedure, premedication with 3 ╬╝g of fentanyl was provided and local anesthesia with lidocaine was administered during the procedure. The urinary bladder was punctured over the suprapubic region using a 21-gauge Chiba needle (Cook, Bloomington, IN, USA) under ultrasound guidance, and a 0.018-inch guide wire was inserted, followed by exchange with a 6-Fr Neff catheter (Cook) (Fig. 1A). A 0.035-inch hydrophilic guide wire (Radifocus Guide Wire M, Terumo, Tokyo, Japan) was then inserted (Fig. 1B). The 6-Fr Neff catheter was exchanged with an 8.5-Fr drainage catheter (Cook) (Fig. 1C). Clear urine was aspirated after removal of the guide wire and the urinary bladder collapsed after the aspiration of the urine (Fig. 1D). The percutaneous suprapubic catheter was taped securely in place on the abdomen. Portable postprocedure abdominal radiography confirmed the position of the cystostomy catheter (Fig. 1E). The procedure was successful and no complications were noted.
Discussion
Percutaneous cystostomy offers an alternative way to drain the urinary bladder when urethral catheterization is contraindicated or unsuccessful [4,5]. Indications for cystostomy in pediatric patients include temporary urinary diversion during surgery for hypospadias, cloacal anomalies, urethral trauma, or stricture [6,7]. Other indications include the need for short-term decompression in patients with posterior urethral valves who are unfit for primary valve ablation [8,9]. The use of percutaneous suprapubic cystostomy as an access route for lithotripsy of bladder calculi in pediatric patients has also been reported [10]. In our case, since urethral trauma was clinically suspected, functional bypass of the urethra by cystostomy was indicated.
The general contraindications for percutaneous cystostomy in pediatric patients are similar to those in adults. This procedure is contraindicated when the urinary bladder is not distended and cannot be localized with ultrasonography [6]. Percutaneous cystostomy performed in infants is often considered to be technically demanding, and there are understandable worries about a potentially increased complication rate if it is performed as a bedside procedure [1-3]. Another possible reason that cases are preferentially not performed at the bedside is the convenience of having a large amount of readily available specialized equipment in the operation room or interventional radiology suite. Most pediatric cases that have been reported were performed in a surgical setting [3,7,8,10,11].
However, neonates in the neonatal intensive care unit are often critically ill patients who require continuous life support and monitoring. As in our case, they may not be stable enough to be transferred to the interventional radiology suite or operation room for cystostomy. One solution for this dilemma is to perform the procedure at the bedside. With improved patient monitoring and life support, it is possible to use the neonatal intensive care unit as a miniature interventional radiology suite.
The techniques used in percutaneous cystostomy for infants are modifications of those used in adults. The main differences are the use of smaller catheters and the necessity of employing more refined techniques, due to the smaller body size and a more confined operating field. Previous reports have indicated that it is preferable to use smaller catheters (8-10 Fr) in pediatric patients [3,6]. Cases of percutaneous cystostomy or suprapubic aspiration performed in pediatric patients without image guidance have been reported [12]. However, we recommend the use of ultrasound examination before bedside percutaneous cystostomy, as it can help confirm the degree of distension and the position of the urinary bladder. Ultrasonography also assists in evaluating the surrounding intervening bowel loops and vasculature and provides important information for planning the most direct route for percutaneous access to the bladder.
The general complications of percutaneous cystostomy in pediatric patients are similar to those seen in the adult population [3]. Complications include minor bleeding, bowel injury, voiding of the tip of catheter into the proximal urethra, infection and stone formation, thickening of the bladder wall secondary to chronic irritation, and bladder spasms [6]. Anuric acute renal failure due to obstruction of the vesicoureteral junction by a suprapubic catheter in an infant has also been reported [4].
In conclusion, this case demonstrates that ultrasound-guided percutaneous cystostomy performed in a bedside setting can be safe and minimally invasive in indicated patients, including neonates. Further studies would be helpful to refine the technique and to assess the efficacy and safety of this bedside procedure in infants.



 Print
Print facebook
facebook twitter
twitter Linkedin
Linkedin google+
google+
 Download Citation
Download Citation PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC




