Introduction
The American College of Radiology (ACR) fifth edition of the Breast Imaging-Reporting and Data System [BI-RADS] Atlas [1] provides essential updating and expansion of the guidebook central to breast imaging. The BI-RADS lexicon frames and details the language that we speak in the field of breast radiology. The first edition of BI-RADS, published in 1992, covered only mammography, the sole breast-specific imaging modality at that time. The 2003 BI-RADS Atlas was the fourth edition for mammography and the first edition for breast ultrasonography (US) and magnetic resonance imaging (MRI). This fifth edition is the second edition for US and MRI.
The goals of BI-RADS are to (1) standardize imaging reporting, (2) reduce confusion in imaging interpretations by providing a common language among radiologists and among imaging practices, (3) enable reliable communication to referring clinicians regarding the significance of findings and management recommendations, and (4) facilitate outcomes monitoring.
Overarching concepts apply to the entire BI-RADS fifth edition. Real cases replaced the diagrams in the early editions. Deliberate efforts to “harmonize” the lexicon across modalities (mammography, US, and MRI) changed terms and definitions; these are highlighted. There is now an intentional uncoupling of the assessment and management recommendation categories for various clinical situations; examples of this are also provided. Specific to-do and not-to-do recommendations are provided to facilitate outcomes monitoring across modalities. New “frequently asked questions” (FAQs) and guidance chapters are replete with practical help, and there are several summary tables, convenient for the workstation.
This article presents the updated lexicon using original case examples to illustrate and summarize selected grouped US concepts along with highlighting the key changes and overarching concepts.
US Reporting
Components of a typical report are listed in the Atlas. Indication for the exam (e.g., diagnostic, palpable complaint, screening recall, short-term follow up, or screening), dates of comparison/correlation exams, pertinent physical exam details, and the scope and technique of the exam (e.g., hand-held, automated US, unilateral/bilateral, complete vs. targeted/limited, technologist/radiologist/both, or special techniques) are expected. New is the recommendation to include a succinct description of the breast composition. Next is a clear description of significant findings, with images to document. For example, at minimum, a negative complete screening US should show all four quadrants and retroareolar regions. Each practice may choose to include axillary views. When mammography and US are jointly performed, composite reports that report in chronological order with one overall BI-RADS assessment are recommended. The most worrisome feature from either or both exams should lead to the final BI-RADS and management recommendation.
US Lexicon Overview
The following will be presented next, in order as per the Atlas: tissue composition, categories of findings (masses, calcifications, associated features, and special cases), and lexicon classification.
US: Tissue Composition
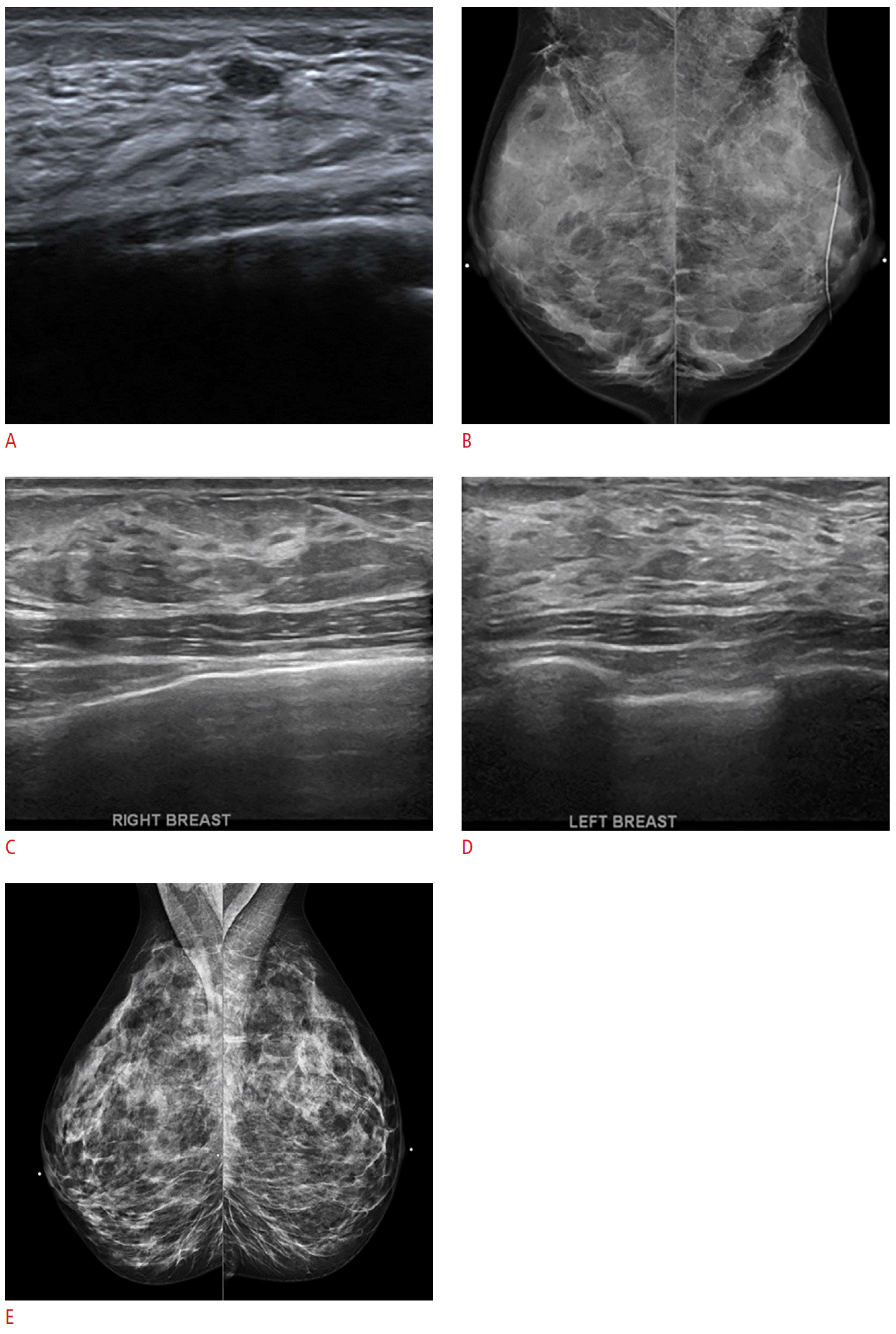
Now recommended is a mention of the dominant tissue composition on the screening US (Fig. 1). This should correlate with mammography, if performed. “Homogeneous background echotexture-fat” parallels a predominantly fatty mammogram. “Homogenous background echotexture-fibroglandular” is a corollary for an extremely dense mammography. “Heterogeneous background echotexture” reflects density categories C and D, possibly leaning towards a denser tissue pattern.
In addition to screening US reports, diagnostic cases may occasionally call for a mention of the breast echotexture as a caveat. For example, when seeking a US correlate for a mammographic asymmetry, a hypoechoic or heterogeneous area with subtle shadowing may be visible. This may be suspicious and indeed be the US correlate for the mammographic concern, but the radiologist should beware and be skeptical first. Scanning and assessing broadly is appropriate. If in the rest of the breast(s), there are many areas having a similar ambiguous echotexture with shadowing, then this finding is less specific and reliable, which might undermine diagnostic confidence. Of course, all the breast imaging tools of triangularization and intermodality correlation should be used. An US-guided biopsy is reasonable to test one's suspicion after exercising due diligence.
US: Findings, Masses
In a deliberate effort to harmonize with mammography, the mass shape descriptors are not oval (i.e., elliptical, egg shaped, have up to 2-3 gentle lobulations), round (i.e., spherical, ball shaped, globular), and irregular (neither round nor oval) (Fig. 2). This schema is simplified for ease of use, but there are still lesions that do not fall neatly into one of these strict definitions. For example, benign-appearing masses with more than three lobulations are common (Fig. 3). The radiologist should use judgment and communicate the details of the case through the prose description.
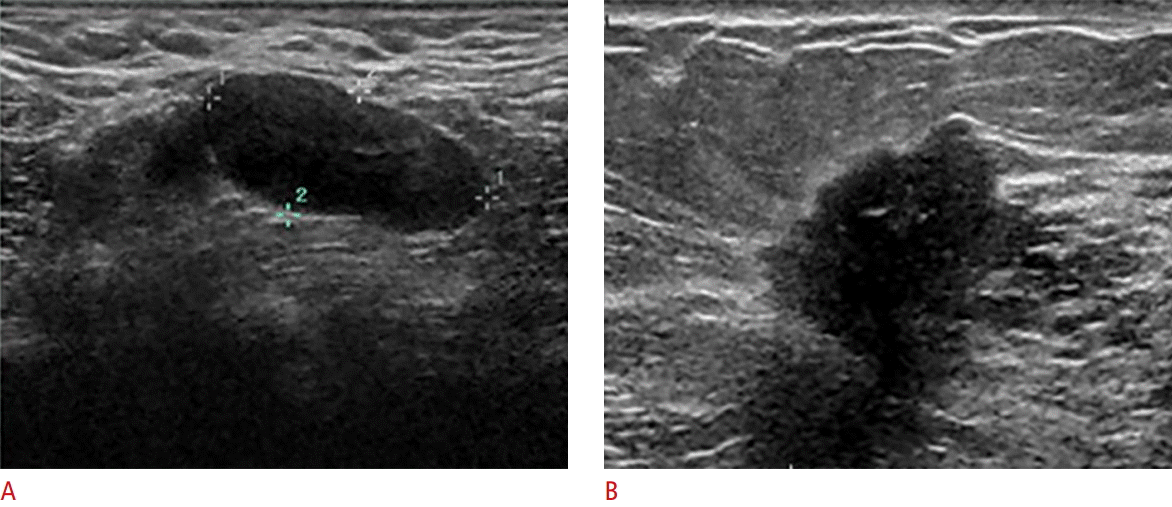
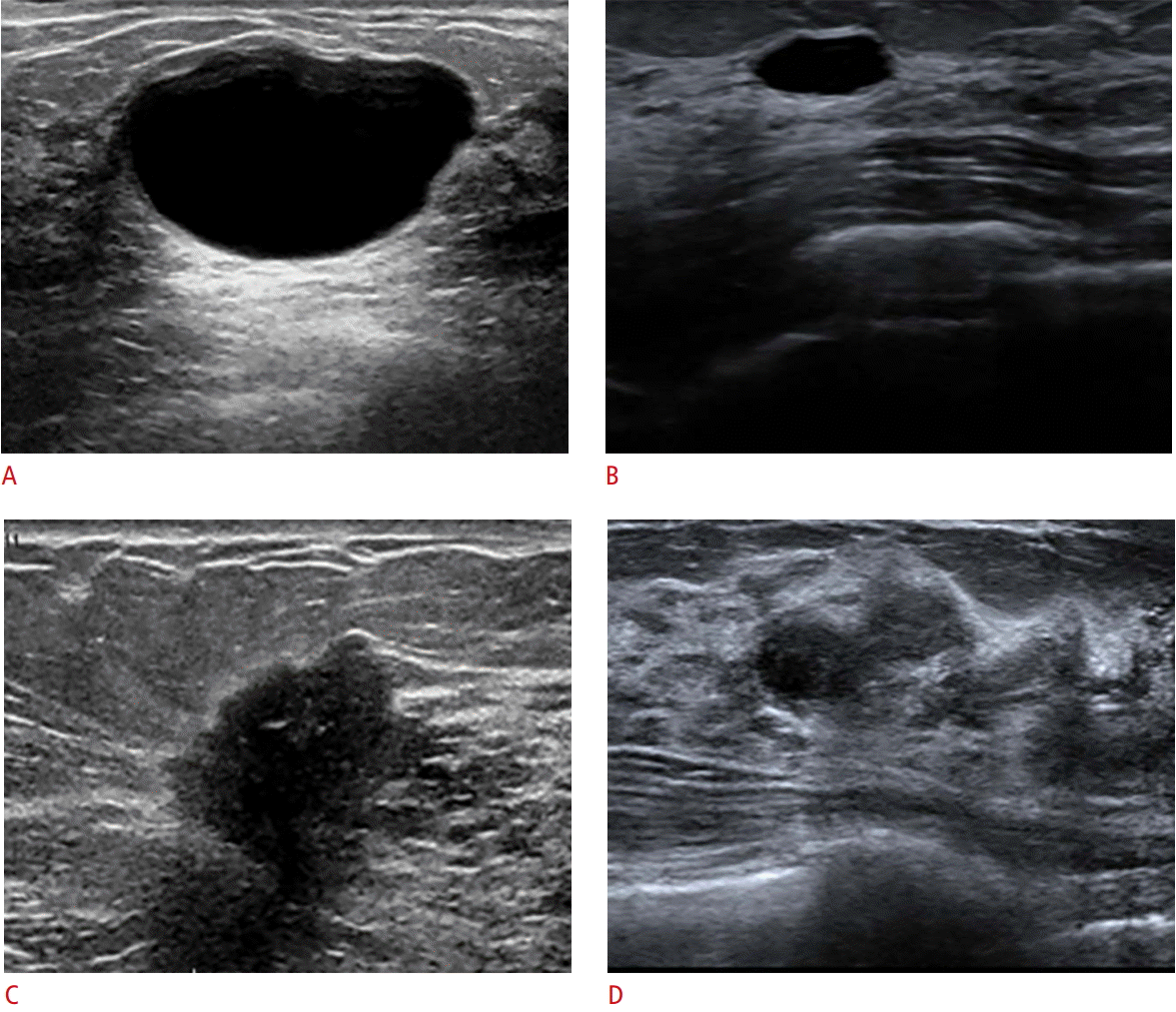
The descriptors for the mass margin first bifurcate into circumscribed or not circumscribed (Fig. 4). A circumscribed margin suggests but is nonspecific for benignity. The subcategories of a not circumscribed margin are indistinct, angular (unique to US), microlobulated, and spiculated; these suggest “not benign” but do not guarantee malignancy. A full-margin evaluation is important, with a real-time assessment recommended particularly for lesions that are indeterminate or cases in which management is not straightforward. Use these descriptors in combination to fully characterize the margin. Proper usage should lead rationally towards a differential diagnosis and support the overall BI-RADS assessment and management recommendations.
The descriptor orientation, echo pattern, and posterior acoustic features are US specific. These are all secondary to the shape and margin in estimating the likelihood for malignancy. Orientation refers to the lesion’s long axis relative to the skin (Fig. 5). Choices are parallel or not parallel, with parallel suggesting a benign etiology. These terms replace the phrases “wider-than-tall” and “taller-than-wide” that are still commonly spoken. By definition, a round mass is neither parallel nor not parallel.
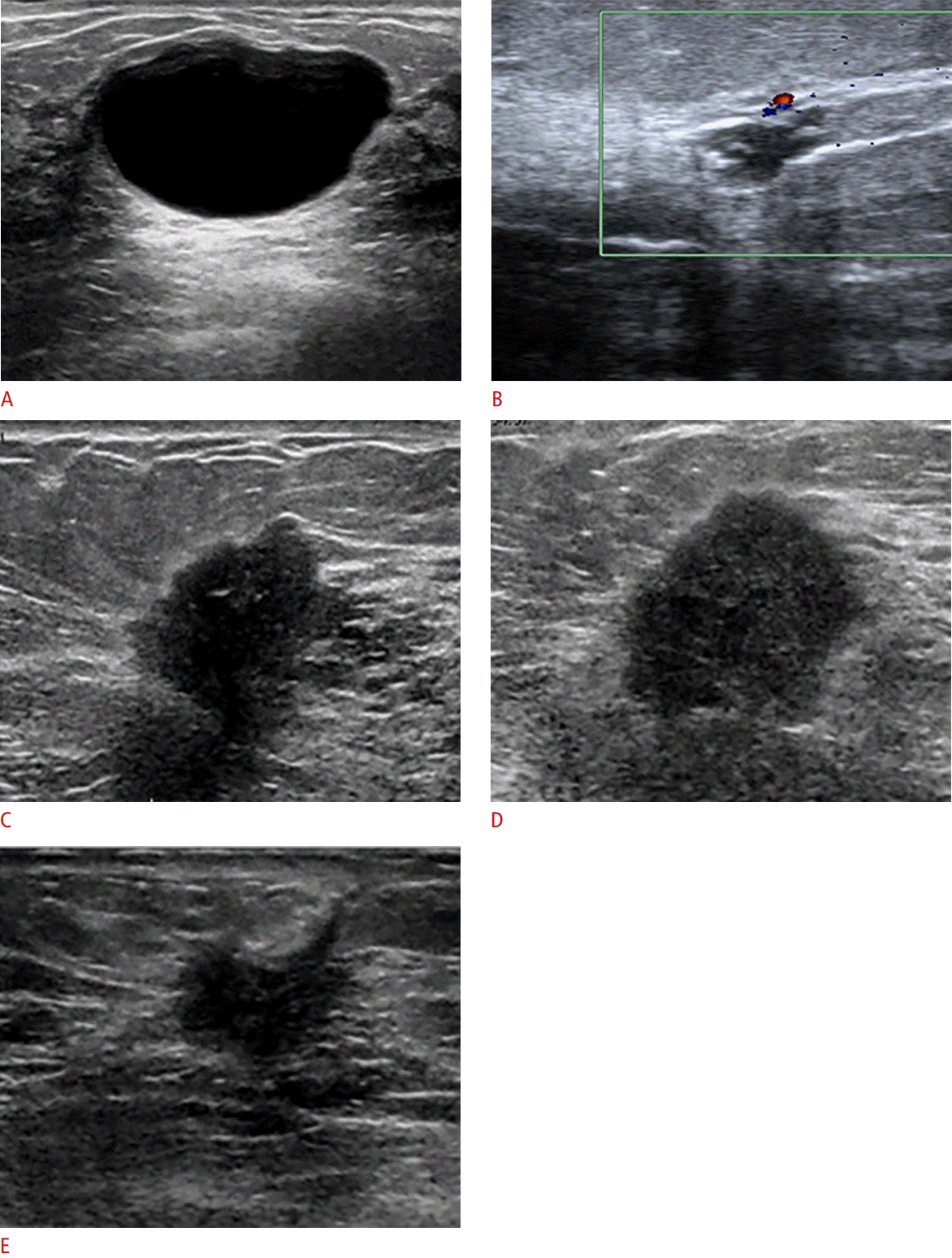
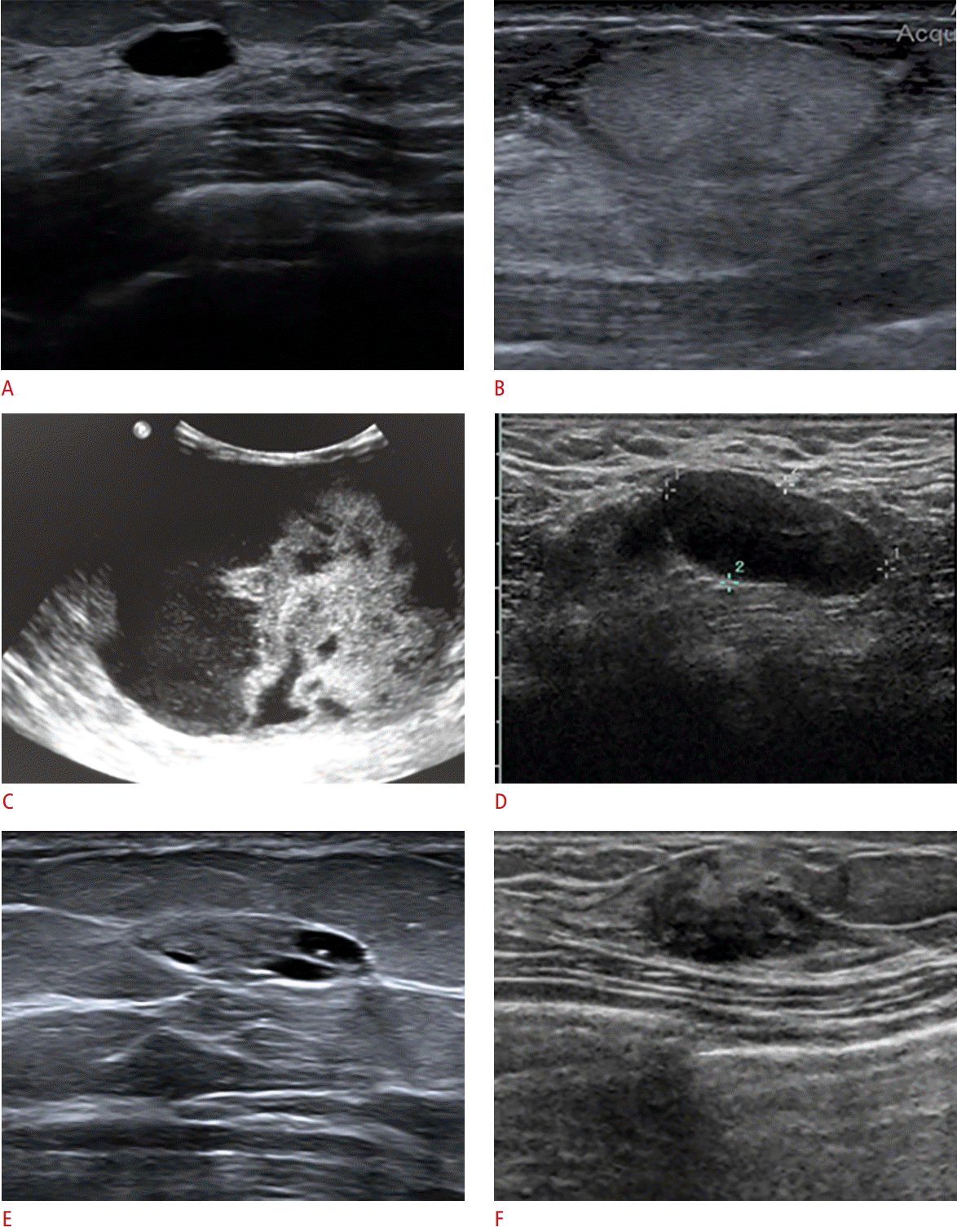
A mass echo pattern relies on fat as the reference echotexture. Choices are anechoic, hyperechoic, complex cystic and solid, hypoechoic, isoechoic, and heterogeneous (Fig. 6). In general, the lesions that we seek are hypoechoic, heterogeneous, or complex cystic and solid.
For posterior acoustic features, choices are no posterior features, enhancement, shadowing, and combined echo pattern. Although posterior acoustic enhancement helps define a classic simple cyst, this feature is not specific for benignity as it can also be seen in lesions such as a metastatic lymph node or metastasis to the breast. In contrast, shadowing is classically associated with a highly suspicious mass, but this suspicious feature is nonspecific and can be seen with benign fat necrosis and stromal fibrosis (Fig. 7).
US: Findings, Calcifications
The BI-RADS Atlas lists choices as follows: calcifications in a mass, calcifications outside of a mass, or intraductal calcifications. It is not clear whether calcifications outside of a mass can mean calcifications without a mass. Although US is not typically used for screening for calcifications or seeking mammographic calcifications, there are occasions when US is used for correlating with mammographic calcifications. Examples would be calcifications associated with a suspicious mass, in an intraductal location, or difficult to reach stereotactically but biopsiable ultrasonographically if found. Mammography should be used to confirm before reporting calcifications as being present. Some US speckles may not be calcifications at all. If a core biopsy is indicated, specimen radiography should be recommended to confirm calcification sampling. Multiple and different diagnoses can coexist in the same patient, as illustrated in Fig. 8. Sometimes, the calcifications are associated with a mass that is of lower suspicion, and US may confirm or help downgrade mammographic suspicion.
US: Findings, Associated Features
Please see the BI-RADS atlas for full detailed list. These are architectural distortion, duct changes, skin changes, edema, vascularity, and elasticity assessment. Elasticity is mentioned not as endorsement but rather as acknowledgement that elastography exists and of possible future formal guidance on usage and reporting. The associated features are architectural distortion, duct changes, skin changes, edema, vascularity, and elasticity assessment. Elasticity is mentioned not as an endorsement but as an acknowledgment that elastography exists and of possible future formal guidance on usage and reporting.
US: Findings, Special Cases
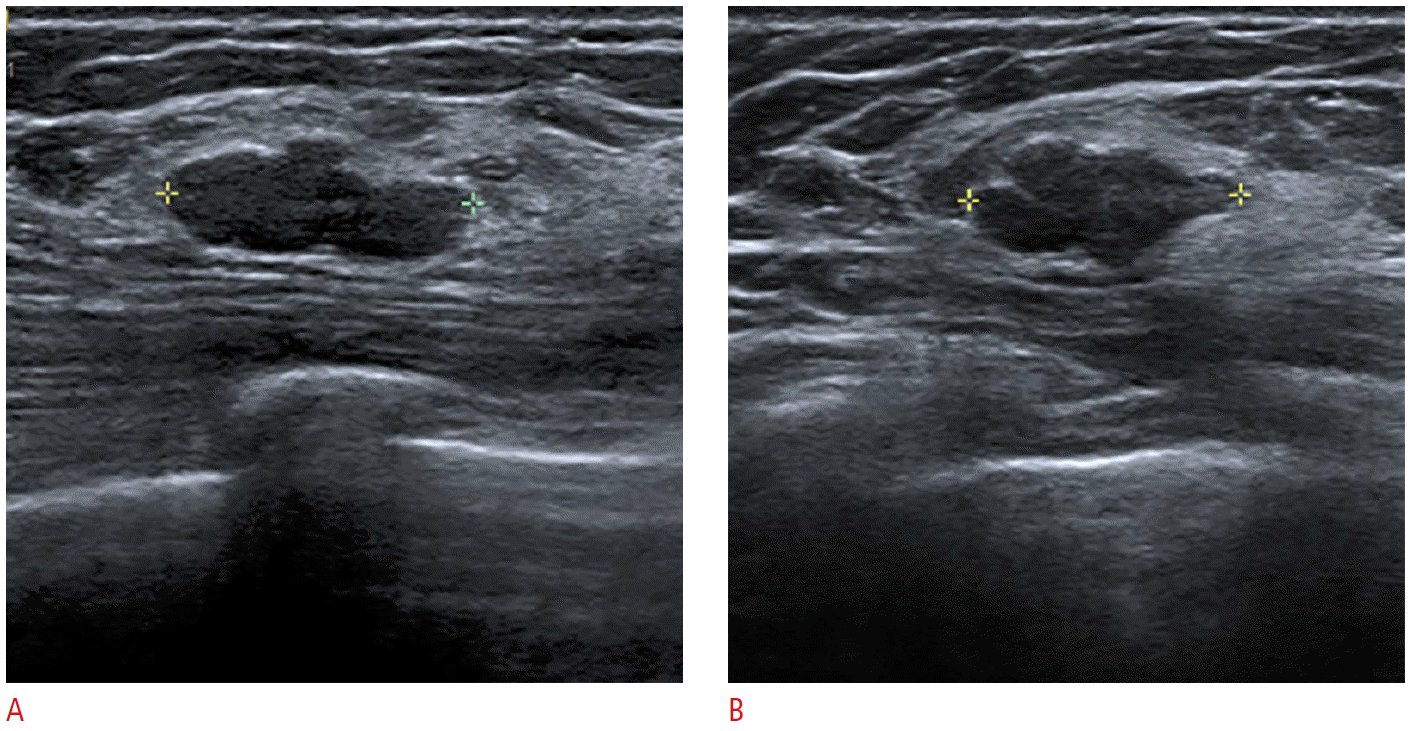
Please refer to BI-RADS atlas for full detailed list and descriptions. Special cases are simple cyst, clustered microcysts, mass in or on skin, foreign body including implants, lymph node-intramammary, lymph node-axillary, vascular abnormalities, postsurgical fluid collection, and fat necrosis. Listed are simple cyst, clustered microcysts, mass in or on the skin, foreign body including implants, lymph node-intramammary, lymph node-axillary, vascular abnormalities, postsurgical fluid collection, and fat necrosis.
US: Assessment and Management
Table 5 in the Ultrasonography section of the atlas maps the BI-RADS assessment categories to their likelihoods of malignancy; please refer to that table for more details regarding these and other small changes in language and percentages. Important adjustments now close the percentage gaps in the prior lexicon. The likelihood of cancer for category 3 is clearly stated as >0% to ≤2%. Even now it is common to hear a reference to BI-RADS 3 to mean a <2% chance of cancer. Category 4 is now a >2% and <95% chance of cancer, with the subcategories now as follows: 4A, >2% to ≤10% likelihood; 4B, >10% to ≤50% likelihood; and 4C, >50% to <95% likelihood. The change in category 4 subdivisions should be noted; “intermediate” has been removed. Category 5 means a ≥95% chance.
Four additional points regarding exam reports are worth mentioning. First, a composite reporting of mammography and US is suggested when both were performed in the same encounter, for instance, for a diagnostic recall from screening or in an evaluation of palpable complaints. The most concerning or worrisome feature from either or both modalities should determine the final BI-RADS and management recommendation. In general, BI-RADS 0 cases should be rare to none.
Second is how screening US should be reported. If according to the technologist’s static images, there are no findings that the radiologist desires to re-evaluate, then BI-RADS 1 or 2 would be appropriate depending on the findings. However, if the radiologist wishes to scan any lesion with a real-time assessment, even if it is of very low suspicion (e.g., a cyst with debris), then BI-RADS 0 is suggested as the appropriate reading. In such a case, a separate exam and accession for “diagnostic ultrasonography” would proceed. These suggested guidelines aim to (1) “harmonize” with the protocol of a screening mammography and (2) accommodate cases when/where the radiologist is not present. The author imagines a variable uptake of this reporting suggestion that will depend on the practice preferences and staffing.
An additional point relates to when a patient should undergo the next screening test. Until there are standard guidelines, which may not ever happen with US, the reporting radiologist should be clear about her/his own recommendations regarding the mammography and US. “Routine screening” is presumptive language; clear and responsible recommendations are the most helpful to patients and referring clinicians.
The fourth point is the now-official uncoupling of the assessment and management to build in a flexible language for the few occasions that call for it. For example, a 35-year-old woman with an enlarging mass presents for baseline imaging. Dense breast tissue but otherwise nonfocal mammography might lead to bilateral breast US showing multiple cysts, some with debris and one clearly accounting for the palpable site. Notice that this would be BI-RADS 2 overall for benign cysts. However, a therapeutic cyst aspiration would be appropriate to offer as an additional line in the impression, for example, “Therapeutic cyst aspiration is offered, if desired.” along with a sentence to the effect of “Screening mammography recommended at the next clinically appropriate interval, with ultrasonography as indicated.”
Another example could be if this same palpable mass were solid and probably benign. If the patient is undergoing in vitro fertilization, then a biopsy would be reasonable. Thus, the radiologist could render a BI-RADS 3 reading and still offer a US-guided biopsy for the diagnosis, if this would help in clinical management. This newly instituted flexibility in language officially sanctions what we already do in our reports, as we fulfill the role of a physician radiologist who appreciates the “big picture” clinical context in which our work matters.
Summary and Conclusion of BI-RADS for US
The BI-RADS fifth edition includes the second edition for breast US. This long-awaited and eagerly anticipated update comprises changes and additions in the US lexicon with real cases similar to the author’s own cases used here for the purpose of illustration. Modifications achieve several overarching goals, namely harmonizing lexicons across modalities (mammography, US, and MRI), anticipating the growing trends of supplemental screening and specialized technologies such as automated breast US and elastography, and helping to guide us towards an effective and efficient interpretation and reporting. Sections on reporting and FAQs are useful for addressing practical questions that may arise in our daily work as breast imagers. The authors of the ACR BI-RADS lexicon do welcome feedback from us, all of us. The lexicon is a living entity and was designed to flex with the times and with our collective needs. Therefore, radiologists should use it well and be empowered to provide the feedback that can help further refine it.



 Print
Print facebook
facebook twitter
twitter Linkedin
Linkedin google+
google+


 Download Citation
Download Citation PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC




