AbstractUltrasound (US) elastography is a valuable imaging technique for tissue characterization. Two main types of elastography, strain and shear-wave, are commonly used to image breast tissue. The use of elastography is expected to increase, particularly with the increased use of US for breast screening. Recently, the US elastographic features of breast masses have been incorporated into the 2nd edition of the Breast Imaging Reporting and Data System (BI-RADS) US lexicon as associated findings. This review suggests practical guidelines for breast US elastography in consensus with the Korean Breast Elastography Study Group, which was formed in August 2013 to perform a multicenter prospective study on the use of elastography for US breast screening. This article is focused on the role of elastography in combination with B-mode US for the evaluation of breast masses. Practical tips for adequate data acquisition and the interpretation of elastography results are also presented.
Ultrasound (US) elastography is an imaging technique that can visualize tissue elasticity (stiffness) in vivo. The first practical equipment was released in 2003, and many manufacturers offer various kinds of commercial systems that are based on the following two US elastography techniques: strain and shear-wave elastography (SWE). The most common type of strain elastography (SE) displays relative tissue displacement under compression, whereas SWE displays an image of the shear-wave speedusing acoustic radiation force excitation.
US elastography is used to perform breast mass evaluation and characterization, and many studies have reported that it can increase the specificity of conventional B-mode US in differentiating benign from malignant breast masses [1-4]. Recently, the US elastographic features of breast masses have been incorporated into the 2nd edition of the Breast Imaging Reporting and Data System (BI-RADS) US lexicon as associated findings [5]; hence, the use of elastography is expected to increase. In addition, the correlations between the elasticity and histological features of breast cancers are also being studied [6-8]. This article is focused on the role of elastography combined with B-mode US for evaluating breast masses. Practical guidelines for performing US elastography on breast tissue, including tips for adequate data acquisition and the interpretation of elastography results, are presented here based on the consensus of the Korean Breast Elastography Study Group.
When the breast tissue is pressed by the transducer, a hard lesion undergoes less strain than does the surrounding soft background. The relative strain in the tissue is displayed in a black-and-white (bright, soft; dark, hard) or color-coded (red, soft; blue, hard) image. In SE, the lesion size or area on the elastogram is compared to the corresponding lesion on the B-mode US image, as malignant lesions appear larger on elastograms than on B-mode US images. Itoh et al. [1] proposed the 5-point scale elasticity score indicating an increasing probability of malignancy (Fig. 1A) that is most commonly used for SE. A cut-off point between the elasticity scores of 3 and 4 was initially suggested to differentiate benign from malignant breast lesions. However, a cut-off point between the elasticity scores of 1 and 2 or 2 and 3 was used in several studies and achieved better diagnostic performance with less interobserver variability [2,4]. Recently, we classified elasticity scores into three categories: a score of 1 (even strain across the entire lesion) as negative, scores of 2 and 3 (uneven strain in the lesion) as equivocal, and scores of 4 and 5 (no strain across the entire lesion) as positive results [3,9]. A specific bull’s eye artifact on black-and-white images or an aliasing artifact that appears as a blue-green-red (BGR) pattern on colorcoded images (Fig. 1B) can be observed in simple cysts [9-11].
Using SWE, transversely oriented shear waves are generated by acoustic radiation force, and these waves propagate faster in hard tissue than soft tissue. A color-coded image displaying the shear wave velocity (m/sec) or elasticity (kilopascals, kPa) for each pixel in the region of interest (ROI) is acquired. Generally, a color scale ranging from 0 (dark blue, soft) to +180 kPa (red, hard) is used for breast lesions. A variety of qualitative and quantitative parameters of SWE have been studied so far [12-20], and the most useful SWE feature is the color assessment of the maximum elasticity, which is correlated with the maximum elasticity value (kPa) (Fig. 2A). The positive predictive value for malignancy increases with increasing elasticity, from 0.4% for dark blue to 81.8% for red colors [16]. The maximum elasticity colors on SWE can be classified into three categories: dark blue and light blue colors (representing soft elasticity) as negative, green and orange colors (intermediate elasticity) as equivocal, and red colors (hard elasticity) as positive [16,21]. Signal-void areas that are not color-coded even in the penetration mode can appear in simple cysts (Fig. 2B) or in very hard masses with dense collagen deposition, as shear waves cannot propagate through them [22].
Elastographic results can be applied to evaluate breast masses in combination with B-mode US findings in the four ways discussed below.
BI-RADS category 4a (low suspicion of malignancy) masses with soft elasticity can be downgraded to category 3 (probably benign), reducing unnecessary biopsies without a significant loss of sensitivity [2,4,16,23]. When downgrading category 4a masses to category 3, two different strategies (aggressive and conservative strategies) can be applied according to the management policy preferences of the radiologist. An aggressive strategy can be used to achieve the highest specificity, whereas a conservative strategy is intended to prevent a false negative. A score of 1 or 2 on SE and a maximum elasticity color of ≤ light blue or a maximum elasticity of ≤ 80 kPa on SWE was used for the aggressive strategy, and a score of 1 on SE and a maximum elasticity color of dark blue or a maximum elasticity of ≤30 kPa on SWE was used for the conservative strategy [16]. Several studies are currently underway under the hypothesis that specific criteria might be needed for each clinical setting, such as screening US or combined examination with Doppler US [24]. A multicenter prospective study is currently underway by the Korean Breast Elastography Study Group on whether US elastography can increase the positive predictive value of screening breast US using either SE or SWE.
BI-RADS category 3 is defined as a breast mass with an oval, circumscribed shape and a margin that presents the typical appearance of fibroadenoma and that has a malignancy rate of less than 2%. On screening US, approximately 20% of women presented BI-RADS category 3 lesions, leading to unnecessary shortterm follow-up in most cases [25]. BI-RADS category 3 masses with very soft elasticity (score 1 on SE or a maximum elasticity color of dark blue or a maximum elasticity of ≤20 kPa on SWE) can safely be downgraded to category 2 (benign), thereby reducing unnecessary short-term follow-up [26,27]. A multicenter prospective study is currently underway by the Korean Breast Elastography Study Group on whether US elastography can increase the positive predictive value of screening breast US using either SE or SWE.
Well-circumscribed cancers can be misclassified as BI-RADS category 3 (probably benign lesions) on B-mode US, leading to a delay in diagnosis. Because these cancers are usually high-grade, it has been proposed that hard elasticity (a score of 4 or 5 on SE and a maximum elasticity color of red or a maximum elasticity of ≥160 kPa on SWE) could be used to detect cancers among BI-RADS category 3 masses [6-8]. However, upgrading category 3 masses might be controversial, especially in a screening setting, because the malignancy rate of category 3 masses is known to be very low [25], and malignancies detected by screening US are known to be small in size, indicating relatively low elasticity [28-30]. We hope that the multicenter prospective study by the Korean Breast Elastography Study Group can offer further evidence on this point.
For malignant breast masses with low suspicious findings on B-mode US (BI-RADS category 4a), hard elasticity can increase the suspicion of malignancy (BI-RADS category 4b or higher), although the management remains unaffected. In addition, fat lobules or benign cysts, which can mimic solid breast masses, can be identified by their markedly soft elasticity, similar to that of the adjacent subcutaneous fat or BGR pattern on elastography, respectively.
The guidelines for combining B-mode US and elastographic results suggested by the Korean Breast Elastography Study Group are summarized in Fig. 3. Positive or negative elastographic results acquired on either SE or SWE can influence the BI-RADS category of a breast mass. For breast masses that present equivocal elastographic results, B-mode US findings should be considered preferentially.
Although elastography is useful during the evaluation of breast masses, a substantial amount of interobserver variability occurs during data acquisition and interpretation [31,32]. The reliability of the imaging technique depends on the training and experience of the operator. Practical tips for adequate data acquisition and interpretation of US elastography results are summarized in Tables 1 and 2.
For adequate data acquisition, the probe should be placed vertically on the skin to correctly compress the tissue using light pressure. SWE is known to be highly reproducible and less dependent on the operator [33-35]; however, technical errors, such as probe compression or movement, can also lead to inaccurate results. Generous amounts of contact jelly should be used and the range of ROI should be adjusted to exclude the skin and chest wall layers to reduce artifacts.
Even when elastography is performed using an appropriate technique, the image quality can be affected by intrinsic factors, such as the lesion size, lesion depth, or breast thickness. On SE, a smaller lesion size, shallower lesion depth, and reduced breast thickness at the site of the lesion were significantly associated with a higher image quality [14]. On SWE, a larger lesion size and increased breast thickness were correlated with a higher falsepositive rate, and a smaller size and deeper lesion were correlated with a higher false-negative rate [36]. Good quality elastographic images can be defined by a high signal-to-noise ratio in the ROI (Fig. 4). High quality images exhibited better diagnostic performance in differentiating benign from malignant breast masses, whereas poor quality images offered less diagnostic information [14,21,37]. Therefore, it is important to consider the image quality during decision making when deciding whether to apply the elastographic result to management.
US elastography provides valuable information regarding tissue elasticity during the assessment of breast masses and can increase the specificity of conventional B-mode US in differentiating benign from malignant breast masses. However, training and education are important for adequate data acquisition and interpretation of elastography results, as well as for deciding whether to apply the elastographic results to management. Our guidelines would be helpful for applying breast US elastography in daily practice.
References1. Itoh A, Ueno E, Tohno E, Kamma H, Takahashi H, Shiina T, et al. Breast disease: clinical application of US elastography for diagnosis. Radiology 2006;239:341–350.
2. Cho N, Moon WK, Park JS, Cha JH, Jang M, Seong MH. Nonpalpable breast masses: evaluation by US elastography. Korean J Radiol 2008;9:111–118.
3. Cho N, Jang M, Lyou CY, Park JS, Choi HY, Moon WK. Distinguishing benign from malignant masses at breast US: combined US elastography and color doppler US--influence on radiologist accuracy. Radiology 2012;262:80–90.
4. Yi A, Cho N, Chang JM, Koo HR, La Yun B, Moon WK. Sonoelastography for 1,786 non-palpable breast masses: diagnostic value in the decision to biopsy. Eur Radiol 2012;22:1033–1040.
5. Harvey J. Breast US: What's new in BI-RADS 2012? In: The 44th Annual Congress of Korean Society of Ultrasound in Medicine. In: The 44th Annual Congress of Korean Society of Ultrasound in Medicine; 2013 May 25; Seoul, Korea. Korean Society of Ultrasound in Medicine. 2013. p.138.
6. Evans A, Whelehan P, Thomson K, McLean D, Brauer K, Purdie C, et al. Invasive breast cancer: relationship between shear-wave elastographic findings and histologic prognostic factors. Radiology 2012;263:673–677.
7. Chang JM, Park IA, Lee SH, Kim WH, Bae MS, Koo HR, et al. Stiffness of tumours measured by shear-wave elastography correlated with subtypes of breast cancer. Eur Radiol 2013;23:2450–2458.
8. Youk JH, Gweon HM, Son EJ, Kim JA, Jeong J. Shear-wave elastography of invasive breast cancer: correlation between quantitative mean elasticity value and immunohistochemical profile. Breast Cancer Res Treat 2013;138:119–126.
9. Kim MY, Cho N, Yi A, Koo HR, Yun BL, Moon WK. Sonoelastography in distinguishing benign from malignant complex breast mass and making the decision to biopsy. Korean J Radiol 2013;14:559–567.
10. Cho N, Moon WK, Chang JM, Kim SJ, Lyou CY, Choi HY. Aliasing artifact depicted on ultrasound (US)-elastography for breast cystic lesions mimicking solid masses. Acta Radiol 2011;52:3–7.
12. Athanasiou A, Tardivon A, Tanter M, Sigal-Zafrani B, Bercoff J, Deffieux T, et al. Breast lesions: quantitative elastography with supersonic shear imaging--preliminary results. Radiology 2010;256:297–303.
13. Evans A, Whelehan P, Thomson K, McLean D, Brauer K, Purdie C, et al. Quantitative shear wave ultrasound elastography: initial experience in solid breast masses. Breast Cancer Res 2010;12:R104.
14. Chang JM, Moon WK, Cho N, Kim SJ. Breast mass evaluation: factors influencing the quality of US elastography. Radiology 2011;259:59–64.
15. Tozaki M, Fukuma E. Pattern classification of ShearWave™ Elastography images for differential diagnosis between benign and malignant solid breast masses. Acta Radiol 2011;52:1069–1075.
16. Berg WA, Cosgrove DO, Dore CJ, Schafer FK, Svensson WE, Hooley RJ, et al. Shear-wave elastography improves the specificity of breast US: the BE1 multinational study of 939 masses. Radiology 2012;262:435–449.
17. Gweon HM, Youk JH, Son EJ, Kim JA. Visually assessed colour overlay features in shear-wave elastography for breast masses: quantification and diagnostic performance. Eur Radiol 2013;23:658–663.
18. Lee EJ, Jung HK, Ko KH, Lee JT, Yoon JH. Diagnostic performances of shear wave elastography: which parameter to use in differential diagnosis of solid breast masses? Eur Radiol 2013;23:1803–1811.
19. Yoon JH, Ko KH, Jung HK, Lee JT. Qualitative pattern classification of shear wave elastography for breast masses: how it correlates to quantitative measurements. Eur J Radiol 2013;82:2199–2204.
20. Kim H, Youk JH, Gweon HM, Kim JA, Son EJ. Diagnostic performance of qualitative shear-wave elastography according to different color map opacities for breast masses. Eur J Radiol 2013;82:e326–e331.
21. Lee SH, Cho N, Chang JM, Koo HR, Kim JY, Kim WH, et al. Twoview versus single-view shear-wave elastography: comparison of observer performance in differentiating benign from malignant breast masses. Radiology 2013 Sep 12 [Epub]. http://dx.doi.org/10.1148/radiology.13130561.
22. Lee SH, Moon WK, Cho N, Chang JM, Moon HG, Han W, et al. Shear-wave elastographic features of breast cancers: comparison with mechanical elasticity and histopathologic characteristics. Invest Radiol 2013 Oct 28 [Epub]. http://dx.doi.org/10.1097/RLI.0000000000000006.
23. Youk JH, Gweon HM, Son EJ, Han KH, Kim JA. Diagnostic value of commercially available shear-wave elastography for breast cancers: integration into BI-RADS classification with subcategories of category 4. Eur Radiol 2013;23:2695–2704.
24. Lee SH, Chang JM, Cho N, Koo HR, Bae MS, Kim WH, et al. Added value of shear-wave elastography in evaluation of breast masses detected on screening ultrasound. In: Radiological Society of North America 99th Scientific Assembly and Annual Meeting; 2013 Dec 1-6; Chicago, IL.
25. Barr RG, Zhang Z, Cormack JB, Mendelson EB, Berg WA. Probably benign lesions at screening breast us in a population with elevated risk: prevalence and rate of malignancy in the ACRIN 6666 trial. Radiology 2013;269:701–712.
26. Schafer FK, Hooley RJ, Ohlinger R, Hahne U, Madjar H, Svensson WE, et al. ShearWave™ Elastography BE1 multinational breast study: additional SWE™ features support potential to downgrade BI-RADS®-3 lesions. Ultraschall Med 2013;34:254–259.
27. Lim J, Cho N, Yi A, Chang JM, Moon WK. Can US-elastography help reduce the number of short-term follow-ups for BI-RADS category 3 lesions detected on supplemental screening breast US? In: Radiological Society of North America 98th Scientific Assembly and Annual Meeting; 2012 Nov 25-30; Chicago, IL.
28. Berg WA, Blume JD, Cormack JB, Mendelson EB, Lehrer D, Bohm-Velez M, et al. Combined screening with ultrasound and mammography vs mammography alone in women at elevated risk of breast cancer. JAMA 2008;299:2151–2163.
29. Bae MS, Han W, Koo HR, Cho N, Chang JM, Yi A, et al. Characteristics of breast cancers detected by ultrasound screening in women with negative mammograms. Cancer Sci 2011;102:1862–1867.
30. Chang JM, Moon WK, Cho N, Yi A, Koo HR, Han W, et al. Clinical application of shear wave elastography (SWE) in the diagnosis of benign and malignant breast diseases. Breast Cancer Res Treat 2011;129:89–97.
31. Regner DM, Hesley GK, Hangiandreou NJ, Morton MJ, Nordland MR, Meixner DD, et al. Breast lesions: evaluation with US strain imaging--clinical experience of multiple observers. Radiology 2006;238:425–437.
32. Burnside ES, Hall TJ, Sommer AM, Hesley GK, Sisney GA, Svensson WE, et al. Differentiating benign from malignant solid breast masses with US strain imaging. Radiology 2007;245:401–410.
33. Cosgrove DO, Berg WA, Dore CJ, Skyba DM, Henry JP, Gay J, et al. Shear wave elastography for breast masses is highly reproducible. Eur Radiol 2012;22:1023–1032.
34. Gweon HM, Youk JH, Son EJ, Kim JA. Clinical application of qualitative assessment for breast masses in shear-wave elastography. Eur J Radiol 2013;82:e680–e685.
35. Mun HS, Choi SH, Kook SH, Choi Y, Jeong WK, Kim Y. Validation of intra- and interobserver reproducibility of shearwave elastography: phantom study. Ultrasonics 2013;53:1039–1043.
Strain elastographic images of breast masses.A. Five-point scale elasticity scores (Tsukuba score) with increasing probability of malignancy. A score of 1 indicates even strain throughout the entire hypoechoic lesion; a score of 2 indicates strain in most of the hypoechoic lesion with some areas of no strain; a score of 3 indicates strain at the periphery of the hypoechoic lesion with sparing of the center of the lesion; a score of 4 indicates no strain throughout the entire hypoechoic lesion; and a score of 5 indicates no strain throughout the entire hypoechoic lesion or in the surrounding area. B. An aliasing artifact that appears as a blue-green-red (BGR) pattern can be seen in a simple cyst. Note that a color code of red indicates soft, and blue is hard.
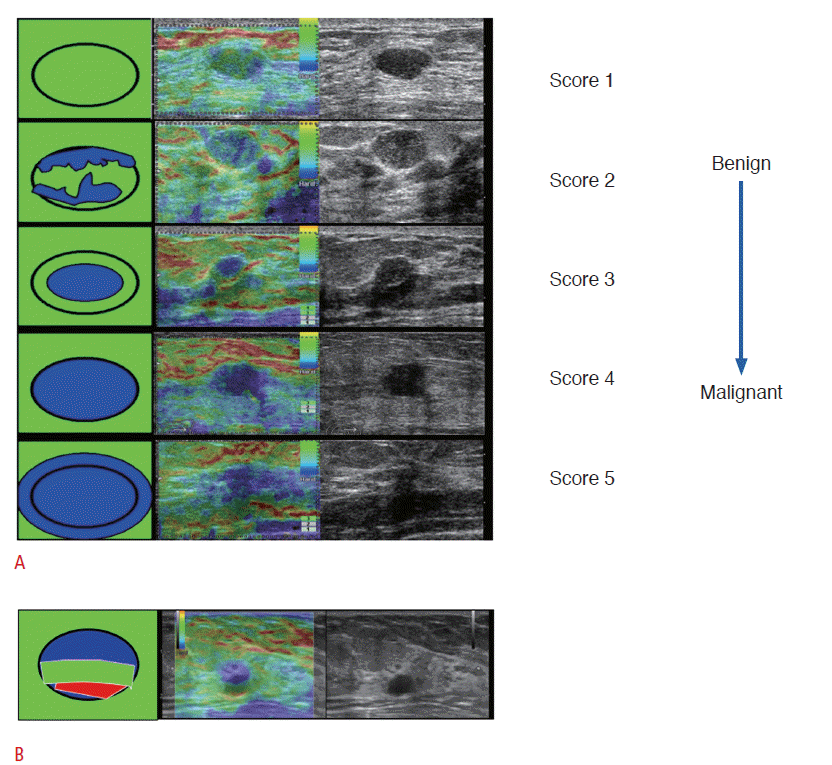 Fig. 1.Shear-wave elastographic images of breast masses.A. The ranges of maximum elasticity value according to the maximum elasticity color of breast masses are shown using a default color scale that ranges from 0 to +180 kPa. The maximum elasticity colors on shear-wave elastography (SWE) can be classified into three categories: dark blue and light blue indicating soft elasticity, green and orange indicating intermediate elasticity, and red indicating hard elasticity. B. A signal-void area (arrow) appears in a simple cyst.
 Fig. 2.A flowchart showing the combination of B-mode and elastographic results for the evaluation of breast masses.Positive or negative elastographic results acquired on either strain elastography (SE) or shearwave elastography (SWE) can change the Breast Imaging Reporting and Data System (BI-RADS) category of breast masses. For the breast masses that present equivocal elastographic results, the B-mode ultrasound findings should be considered preferentially. E(+), positive result on SE or SWE; E(-), negative result on SE or SWE.
 Fig. 3.Representative good and poor quality elastographic images.A. Good quality images on SE can be defined by a high signal-to-noise ratio in the region of interest. B. Poor quality images were acquired due to probe slipping (left) and a deeply located lesion or thick breast (right) on strain elastography. C. Good quality images with the typical appearance of a benign (left) and malignant mass (right) on shear-wave elastography (SWE). D. A benign mass can exhibit increased stiffness when the SWE image was acquired using compression (left). Artifacts can appear on SWE images (right) in the skin and chest wall (arrows).
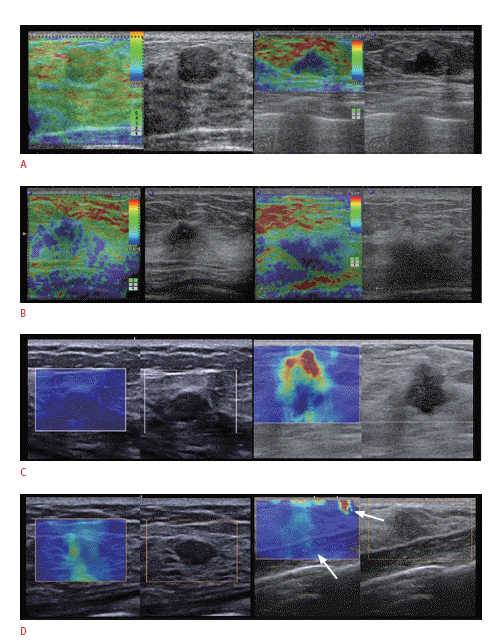 Fig. 4.Table 1Practical tips for data acquisition during breast ultrasound elastography Table 2Practical tips for the interpretation of breast ultrasound elastography |



 Print
Print facebook
facebook twitter
twitter Linkedin
Linkedin google+
google+
 Download Citation
Download Citation PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC




