Introduction
Ultrasonography is an essential imaging modality in diagnosing testicular and scrotal pathology, as it provides fine anatomical details of the testicle and surrounding structures and evaluates vascular perfusion in real time. Clinical examination often yields nonspecific signs and symptoms such as scrotal pain, swelling or a palpable scrotal mass. Ultrasonography is able to identify and characterize intratesticular or extratesticular lesions and is often able to distinguish between benign or malignant lesions as well as identify conditions that require emergent surgical intervention. In addition, ultrasonography is a safe, relatively inexpensive, and readily available imaging modality that does not require ionizing radiation. This pictorial review provides an overview of the ultrasonographic anatomy of the scrotum followed by diagnosis of a variety of intra- and extratesticular lesions based on different clinical manifestations.
Normal Scrotal Anatomy on Ultrasonography
Both testicles lie within the scrotum, a fibromuscular sac divided into the right and left hemiscrotum by a midline septum (raphe). The normal male testicle is an ovoid structure measuring approximately 5×3×2 cm (length×height×breadth) with a homogeneous, intermediate echogenicity (Fig. 1). The epididymis is a comma-shaped, elongated structure located at the posterior border of the testicle and is divided into the head, tail, and body. The epididymal head overhangs the superior pole of the testicle and is isoechoic or slightly hyperechoic to the adjacent testicular tissue. The epididymal body and tail are located behind and along the inferior pole of the testicle and are usually isoechoic to the testis. Anatomically, they are located behind and at the inferior pole of the testicle.
Within each hemiscrotum, the testicle and epididymis are enclosed by a fibrous capsule, the tunica albuginea. On ultrasonography, the capsule is seen as a thin echogenic band outlining the testis.
The tunica albuginea is covered by the tunica vaginalis, a remnant of the processus vaginalis, which represents a closed sac of peritoneum consisting of two layers. The visceral layer lines the tunica albuginea of the testis and is separated from the parietal layer that lines the inner aspect of the scrotal wall by a small amount of fluid-containing interspace. The tunica albuginea extends into the posteromedial testis to form the mediastinum testis (Fig. 2), which contains ducts, nerves and blood vessels. The mediastinum is usually seen on ultrasonography as a thin echogenic band. There are several fibrous septa that extend from the mediastinum testis in order to divide the testicle into multiple small lobules. These lobules contain seminiferous tubules, which converge to form the tubuli recti, testicular ducts that open into the rete testis. In about 20% of patients, the rete testis can be identified as a hypoechoic area adjacent to the mediastinum testis [1].
Efferent ductules exit the rete testis and drain into the epididymal head. From the epididymal head, the ducts converge into a single duct within the epididymal body that exits the epididymal tail as the vas deferens. The vas deferens then courses superiorly within the inguinal canal as part of the spermatic cord. In addition to the vas deferens, the spermatic cord contains nerves, lymphatic ducts, arteries (testicular artery, deferential artery, and cremasteric artery) and the pampiniform venous plexus. On ultrasonography, the spermatic cord appears as a highly echogenic band within the inguinal canal.
The pampiniform venous plexus continues as the testicular vein in the deep inguinal canal. The left testicular vein drains via the left renal vein into the inferior vena cava (IVC) whereas the right testicular vein drains directly into the IVC.
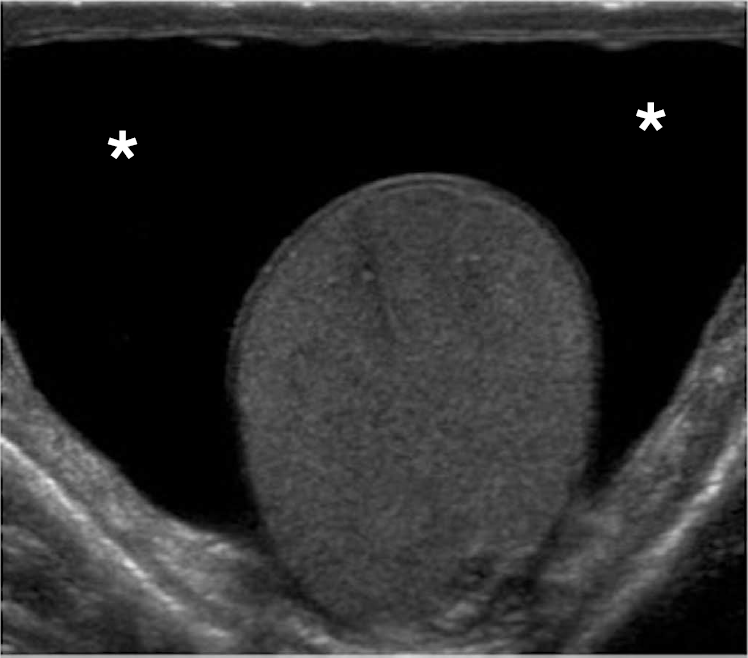
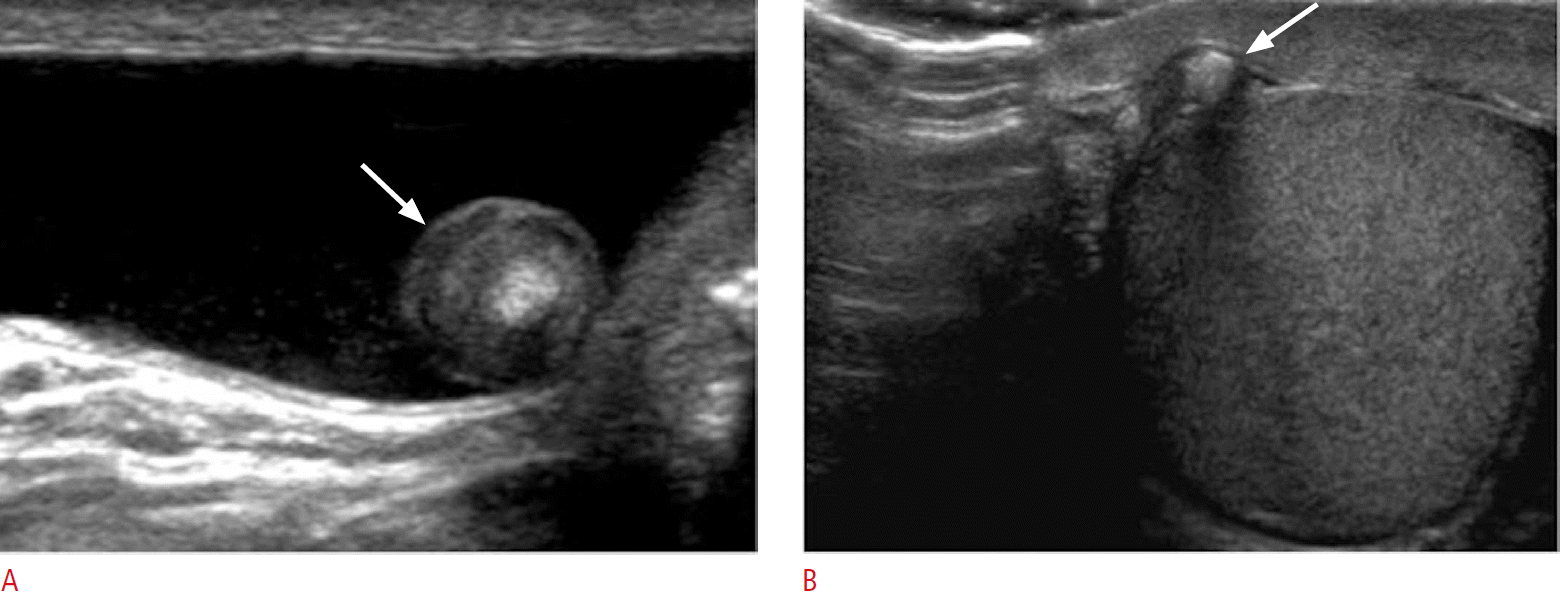
Epididymal and testicular appendages represent embryologic remnants that can be identified on ultrasonography, especially when a hydrocele is present. The appendix testis (hydatid of Morgagni) is seen as an isoechoic, oval structure located between the epididymis and testis (Fig. 3). An appendix epididymis is an often-pedunculated structure arising from the epididymal head, which also appears isoechoic to testicular tissue (Fig. 4).
Technique and Scanning Protocol
Ultrasonography of the scrotum includes greyscale and color Doppler evaluation of testicles, epididymides, and the scrotum. Spectral Doppler evaluation is performed to demonstrate appropriate waveforms within the testicular artery and vein. Usually, a high frequency, broad bandwidth 17-5 MHz or 12-5 MHz transducer is used. The testicles and scrotum are elevated and supported with a towel placed underneath the scrotum. The patient holds another towel to retract and cover the penis.
Many scanning protocols begin with a side-by-side, large field-of-view image including both testicles using both grayscale and color Doppler techniques. This allows for comparison of testicular echogenicity and perfusion. Longitudinal images of each testis in the medial, mid, and lateral portions and transverse images of the upper, mid and lower poles of each testis are then obtained. Each testicle should be measured consecutively in three dimensions (length, height, and width). Cineloops of each testis in the sagittal and transverse planes can provide more thorough diagnostic evaluation. Evaluation of the epididymides includes longitudinal and transverse images including the head, body, and tail. Color Doppler survey of the testicles and epididymides should be performed bilaterally with documentation of at least the capsular and centripetal arteries. Spectral waveforms that include both arterial and venous flow should be documented for each side. Color and spectral Doppler analysis should be optimized in attempts to depict low velocity venous flow. Specific evaluation for testicular torsion can be addressed by additional color Doppler imaging documenting several vascular planes and comparison with the contralateral, asymptomatic testis.
The scrotum should be surveyed for any extratesticular finding such as a hydrocele or scrotolith. Veins of the pampiniform plexus should be specifically evaluated as to diameter and augmentation with either the Valsalva maneuver or upright positioning of the patient. The scrotal skin should also be assessed for thickening, edema and symmetry.
Any extra- or intratesticular pathology (diffuse or focal) should be characterized by gray-scale ultrasonographic techniques and supplemental vascular imaging, as appropriate. Focal lesions can be measured consecutively in three dimensions: length, height, and width. The pathology can be characterized ultrasonographically for the presence of cystic, solid, complex-cystic, or calcific components. Obtained images should be labeled with regards to the location of the lesion (upper, mid, and lower), image orientation (longitudinal and transverse) and the patient’s position (supine, decubitus, and standing). Images obtained during performance of any maneuvers (i.e., Valsalva maneuver) should also be specifically labeled.
Acute Scrotal Pain and Swelling
Epididymitis and Epididymo-orchitis
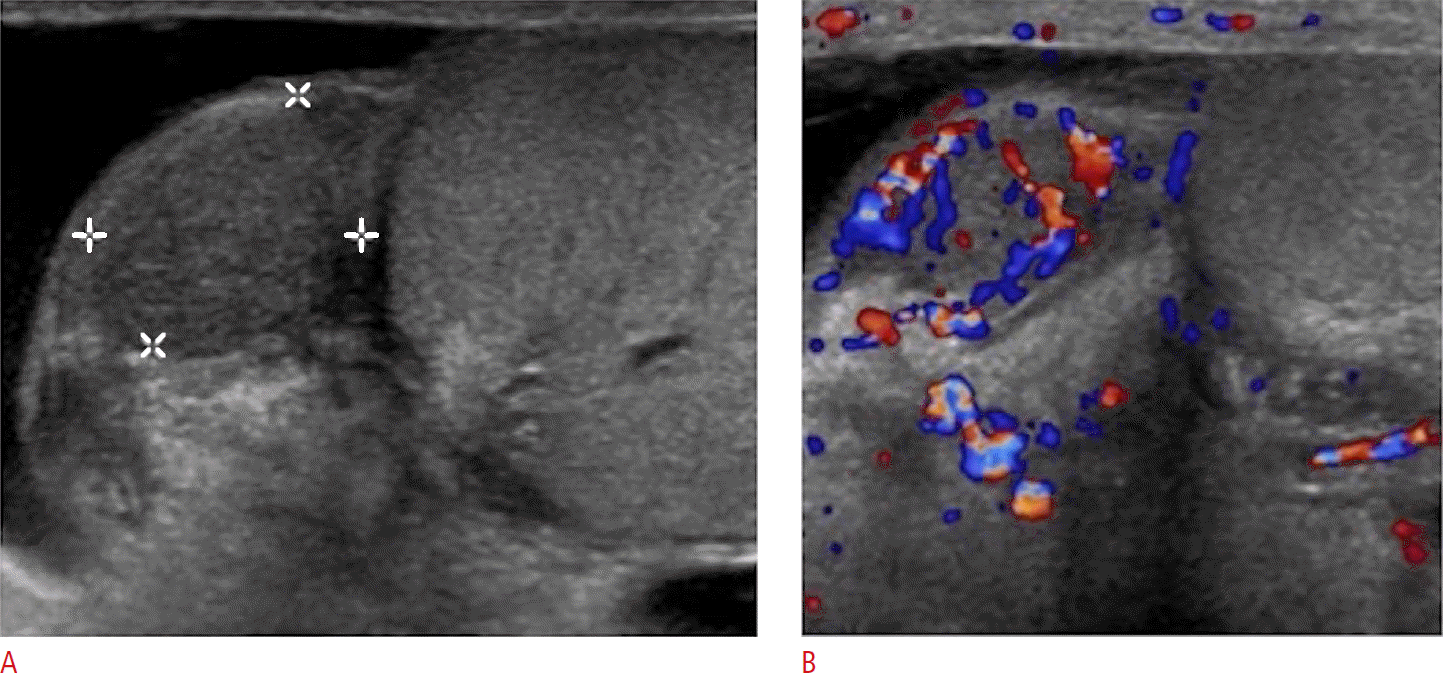
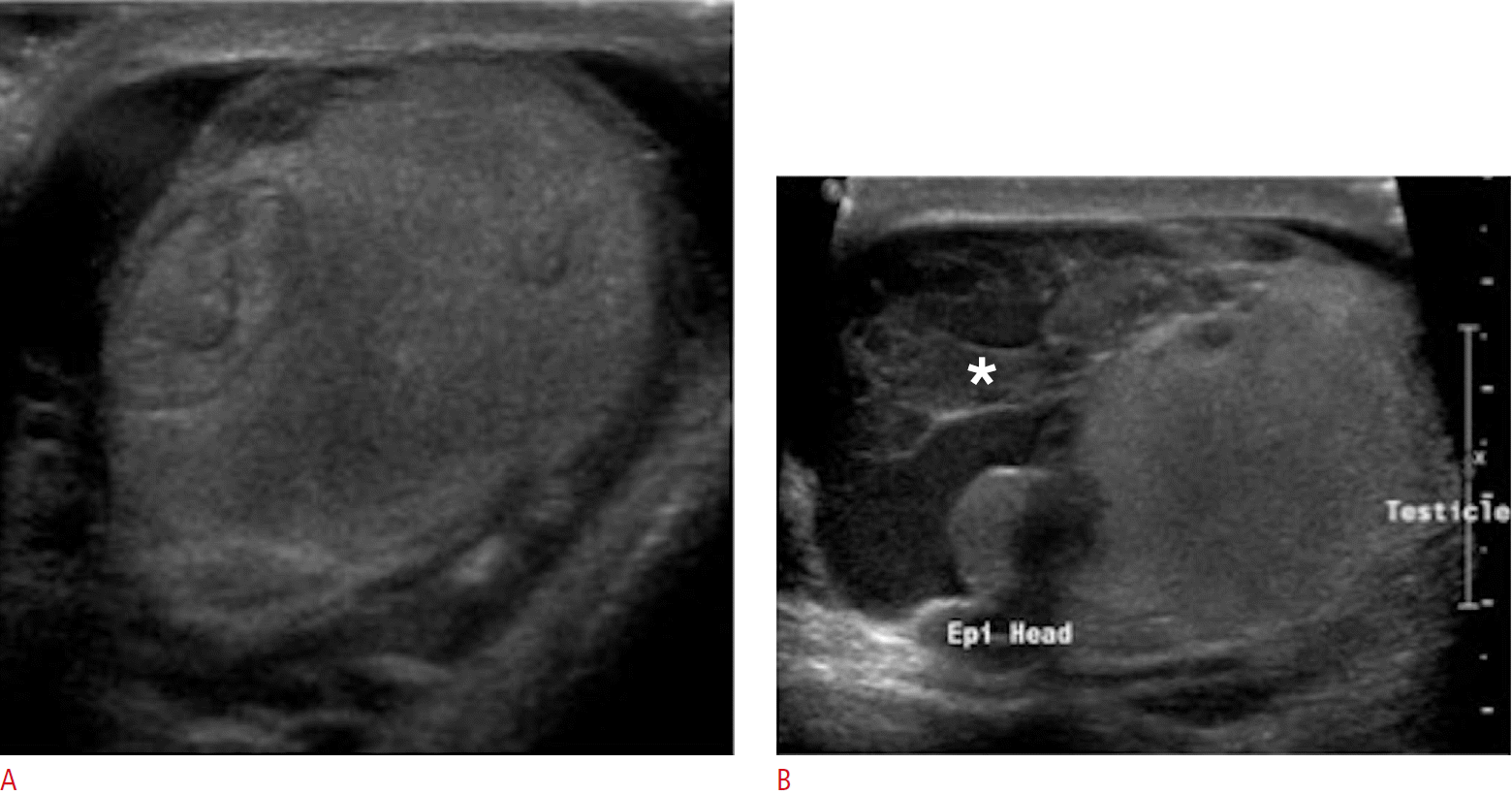
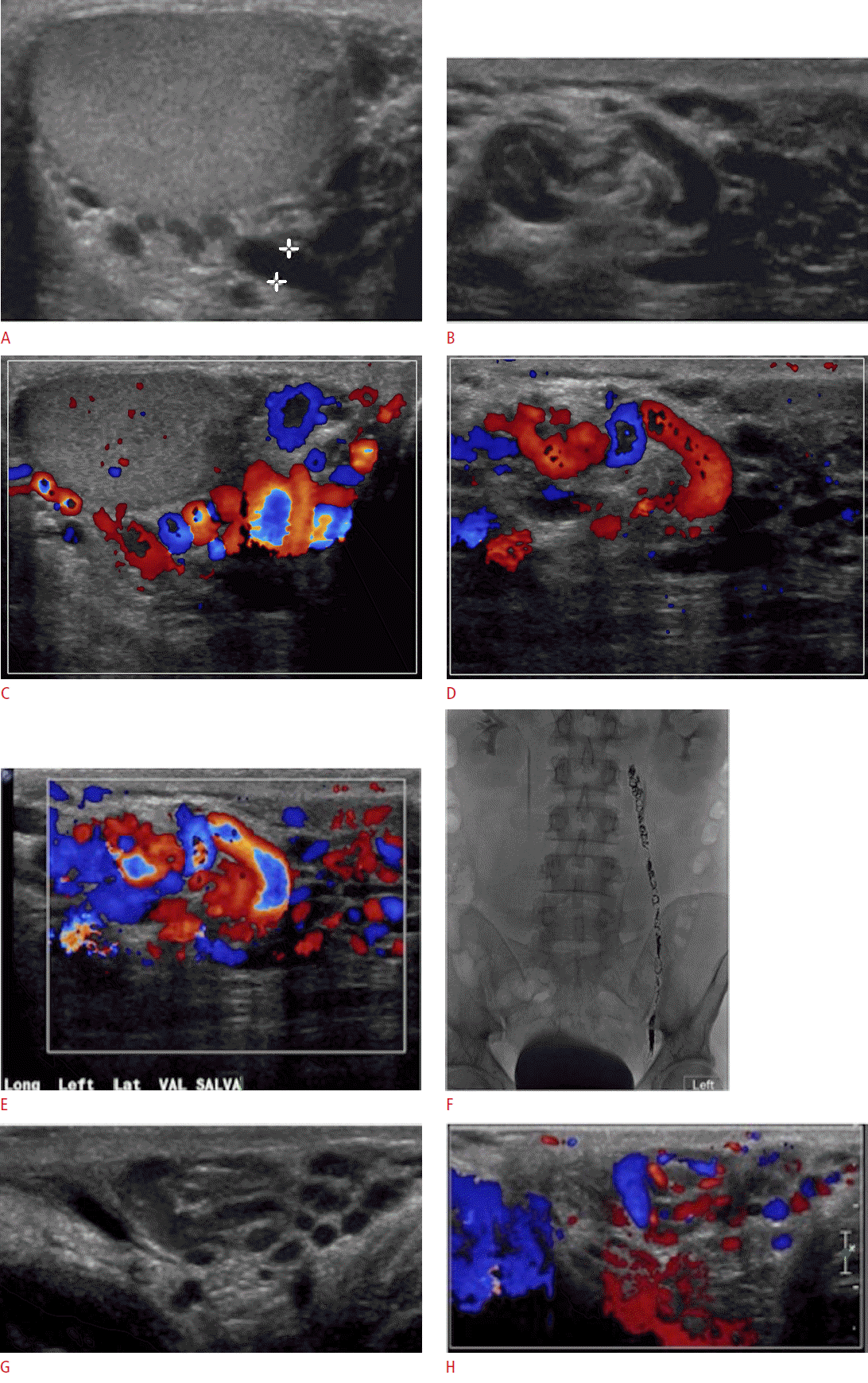
A common cause of acute scrotal pain in adolescent boys and male adults is epididymitis, which is usually the result of an acute bacterial infection. Extension of the infection to the testis, then termed epididymo-orchitis (Fig. 5), occurs in about 20% to 40% of cases due to direct spread of the infection [2]. Ultrasonographic findings of acute infection of the epididymis include an enlarged and hypervascular epididymis with an inhomogeneous echotexture, most often hypoechoic in appearance (Fig. 6). Color Doppler ultrasonographic evaluation has a sensitivity of almost 100% in detecting acute inflammation and is thus a well-established imaging technique for the diagnosis of epididymitis [3-5]. Associated findings include hydrocele or pyelocele, scrotal wall thickening, fistula formation and calcifications [6]. Abscess formation may complicate acute epididymitis and appears as an avascular hypoechoic area within the epididymis.
Orchitis
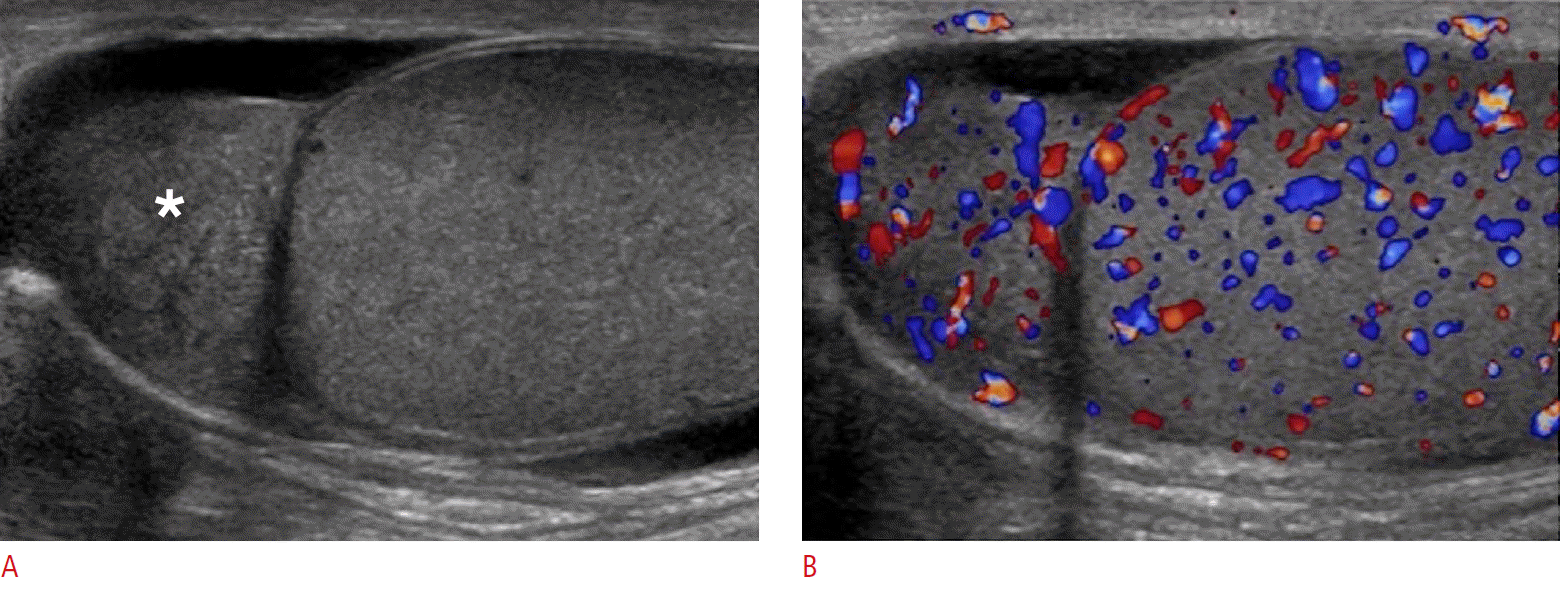
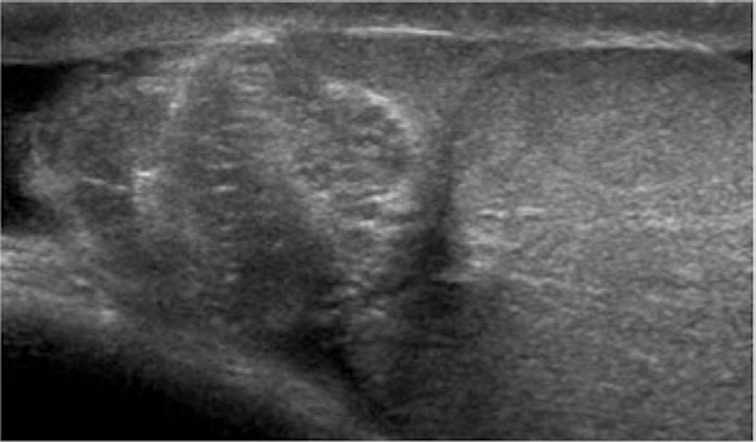
Isolated orchitis without involvement of the epididymis is rare and most commonly secondary to paramyxovirus infection (mumps) [2]. Orchitis most often appears as diffuse testicular involvement. However, it may only involve a focal area. Clinically, orchitis can present with only mild tenderness or evolve into a severe and febrile condition. Markedly increased flow on color Doppler, with an enlarged and heterogeneous appearance of the affected testicle due to diffuse edematous changes, is a pathognomonic ultrasonography finding. In cases of only focal involvement of the testicle, other conditions need to be considered and follow-up ultrasonography should be performed to document resolution and safely exclude infarction, tumor or metastatic disease.
Torsion
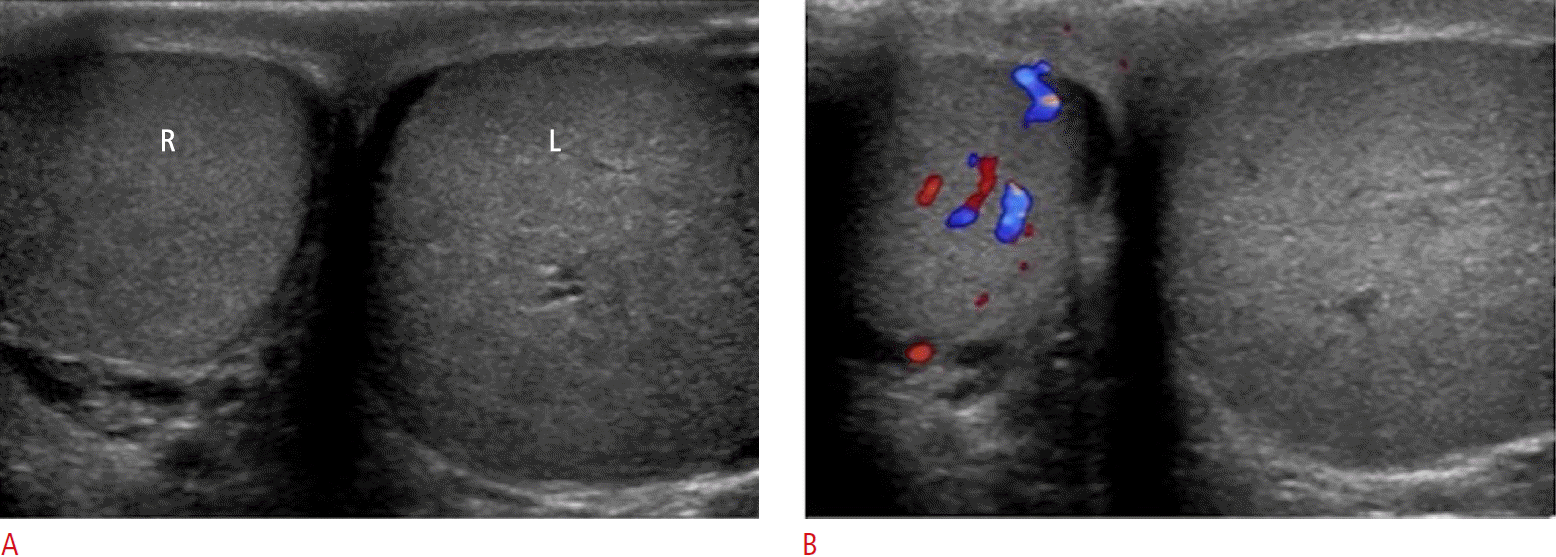
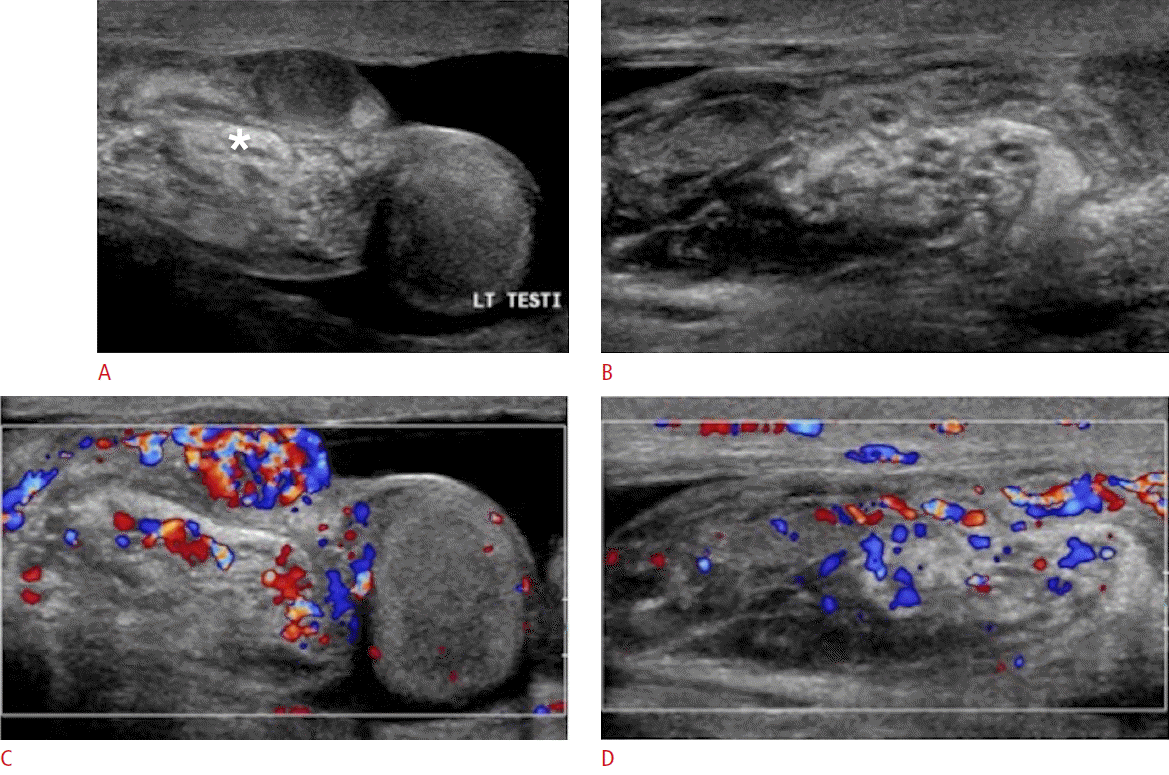
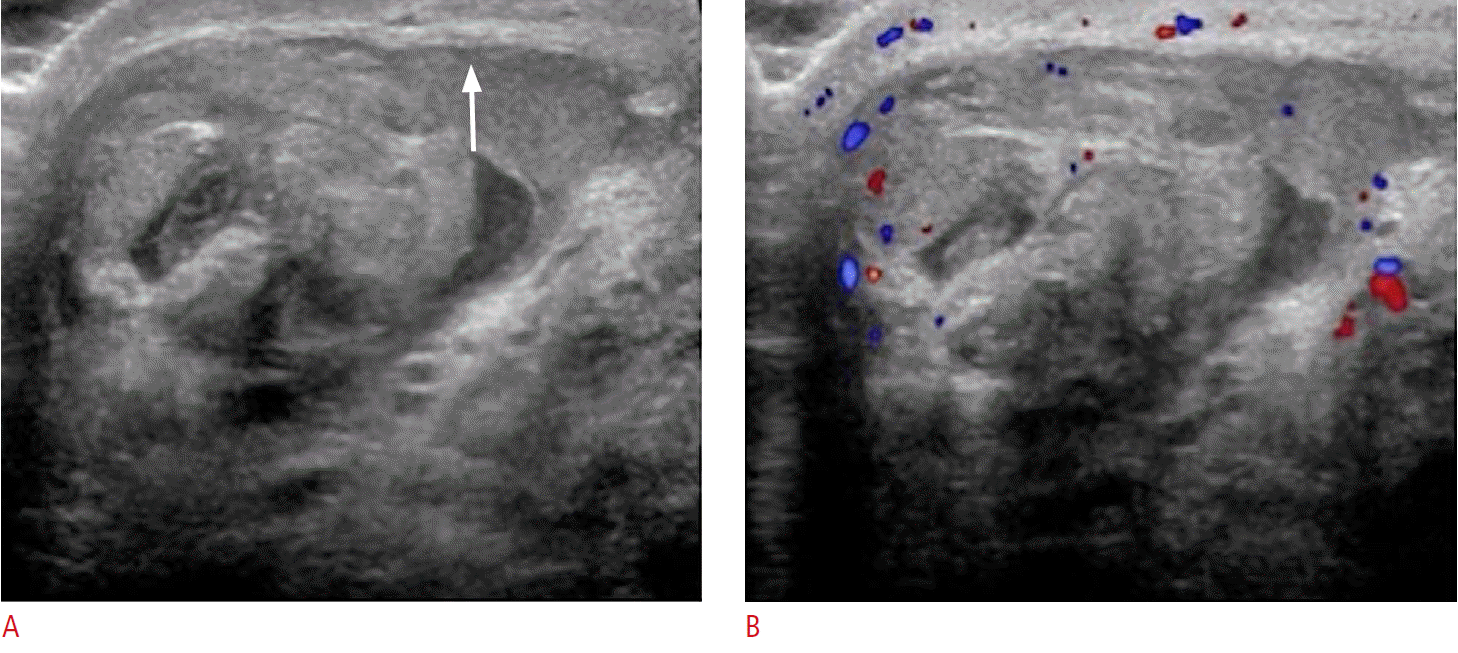
Testicular torsion is most commonly seen in adolescent boys, though it can occur at any age. Normally, the tunica vaginalis fixates the posterior aspect of the testicle. If the tunica vaginalis, however, joins high on the spermatic cord, it leaves the testicle free to rotate within the scrotal sac (bell clapper deformity). Most often, the bell clapper deformity is found bilaterally [7]. Thus, surgical orchiopexy is usually performed bilaterally even if only one testicle has torsed. A sensitive and specific sign for torsion is the so-called real-time whirlpool sign, which is characterized by a spiral twist or rotation of the spermatic cord (Fig. 7). Following rotation of the spermatic cord, blood flow to the testicle is compromised leading to severe ischemia and acute pain. Testicular torsion is a surgical emergency that requires prompt diagnosis and treatment. Ultrasonographic appearance of a torsed testicle varies depending on the duration and degree of torsion. In the early phases, vascular compromise may only affect venous outflow and testicular echogenicity may appear normal. Progressive enlargement and heterogeneity of the testicle is seen in later phases due to edematous changes and arterial obstruction. Definitive diagnosis of complete testicular torsion is made when color Doppler fails to detects blood flow to the torsed testis with normal blood flow to the unaffected testis (Fig. 8). Surgical intervention is reported to be successful in 100% of cases if performed within 6 hours of symptom onset. Success rates, however, decrease to 0%-20% if symptoms have been present for 12-24 hours [8].
Intermittent testicular torsion should be considered in patients presenting with recurrent acute testicular pain with rapid onset and rapid spontaneous resolution. In these patients, surgery may be indicated in order to relieve pain and prevent future infarction of the testicle [9].
Cellulitis
Scrotal wall cellulitis is a cause of inflammatory scrotal wall edema. It is often seen in patients with diabetes, obesity or immunosuppression. Grayscale ultrasonography shows an increased scrotal wall thickness with a hypoechoic appearance and increased vascular flow on color Doppler evaluation. A scrotal wall abscess may form as a complication from scrotal wall cellulitis (Fig. 9). This should be suspected if a loculated fluid collection with irregular walls and low-level internal echoes is found.
Vasitis
Acute vasitis describes an inflammatory process of the vas deferens that usually results from retrograde spread of pathogens from the prostate, prostatic urethra or seminal vesicle. The most common pathogens are Haemophilus influenza and Escherichia coli [10]. Ultrasonography reveals a heterogeneously hypoechoic mass within the inguinal canal, possibly extending towards the scrotal segment, which demonstrates increased vascular flow (Fig. 10).
Trauma
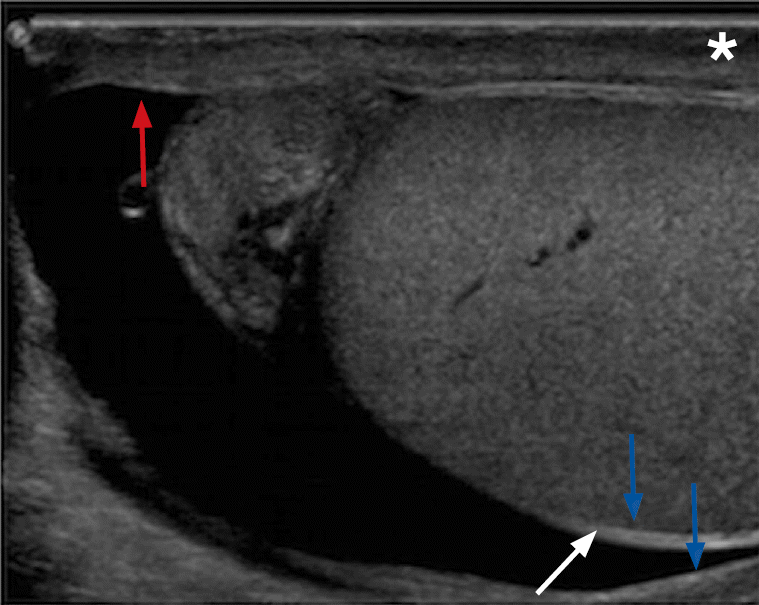
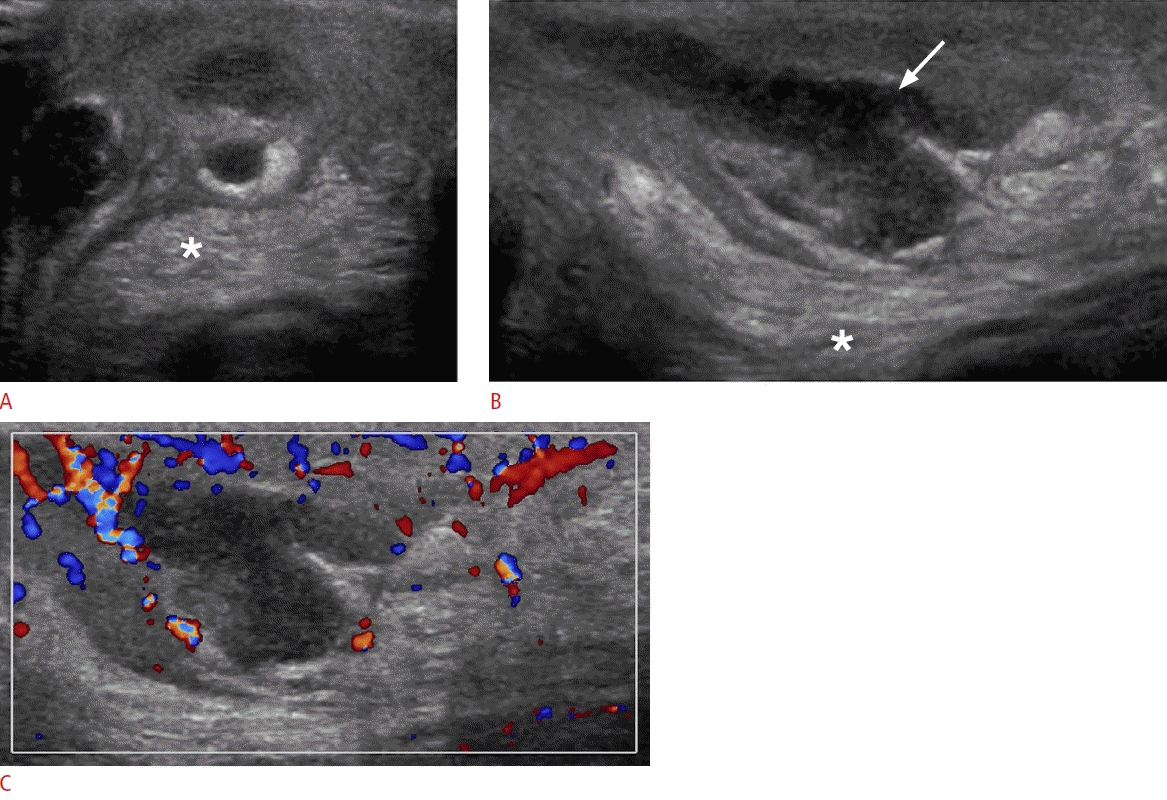
Testicular trauma can manifest as fluid collections (hematocele, hydrocele, or hematoma), testicular disruption (fracture or rupture) or vascular injury. Ultrasonographic evaluation of an injured testicle is crucial in determining conditions that require immediate surgical intervention. Heterogeneous appearance of the testicle, irregular contour abnormality with or without visualized interruption of the tunica albuginea, and loss of focal or diffuse vascular flow are signs consistent with testicular rupture (Figs. 11, 12) [11,12]. Emergent surgical repair performed within 72 hours has a high testicular salvage rate (>80%) [13,14].
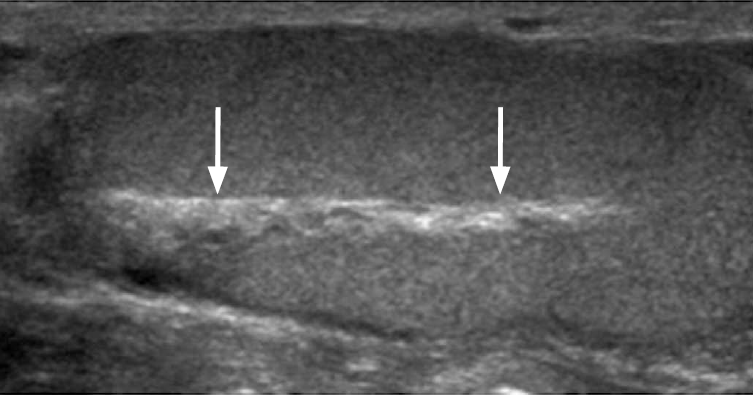
A discontinuity in the usual testicular parenchyma is considered a testicular fracture. It is identified as a hypoechoic, linear stripe within the testicle that does not demonstrate vascularity. Visualization of such a fracture line has only been reported in 17% of cases [15]. Testicular fractures may but do not necessarily have to be associated with a tunica albuginea rupture. Post-traumatic hematomas can be seen in the testicle or in extratesticular locations such as the epididymis, scrotal wall or between the testicles. Acute hematomas have a hyperechoic appearance on ultrasonography. Over time, the hematoma appears increasingly hypoechoic with potentially complex and cystic components. Color Doppler ultrasonography demonstrates no flow within these lesions. Hematoceles are blood collections between the two layers of the tunica vaginalis, which appear echogenic in the acute phase. Older hematoceles appear more hypoechoic and may demonstrate fluid-fluid levels or septations.
Palpable Lumps and Incidental Findings
Epididymal Cyst
Epididymal cysts can occur anywhere within the epididymis and appear as well-circumscribed anechoic lesions (Fig. 13). The cysts demonstrate posterior acoustic enhancement due to their clear serous fluid content. Unless symptomatic, these cysts are clinically irrelevant and no treatment is necessary.
Testicular Cyst
Simple cysts in the parenchyma of the testicle are usually incidental findings. They are solitary, anechoic, well circumscribed, round to oval lesions with increased through-transmission [16] and measure from 2 to 20 mm. Their etiology is often idiopathic; however, they may represent sequelae from prior trauma or inflammation. Careful examination for solid or mural components is advised in order to not miss a potentially malignant cystic lesion.
Epidermoid Cyst
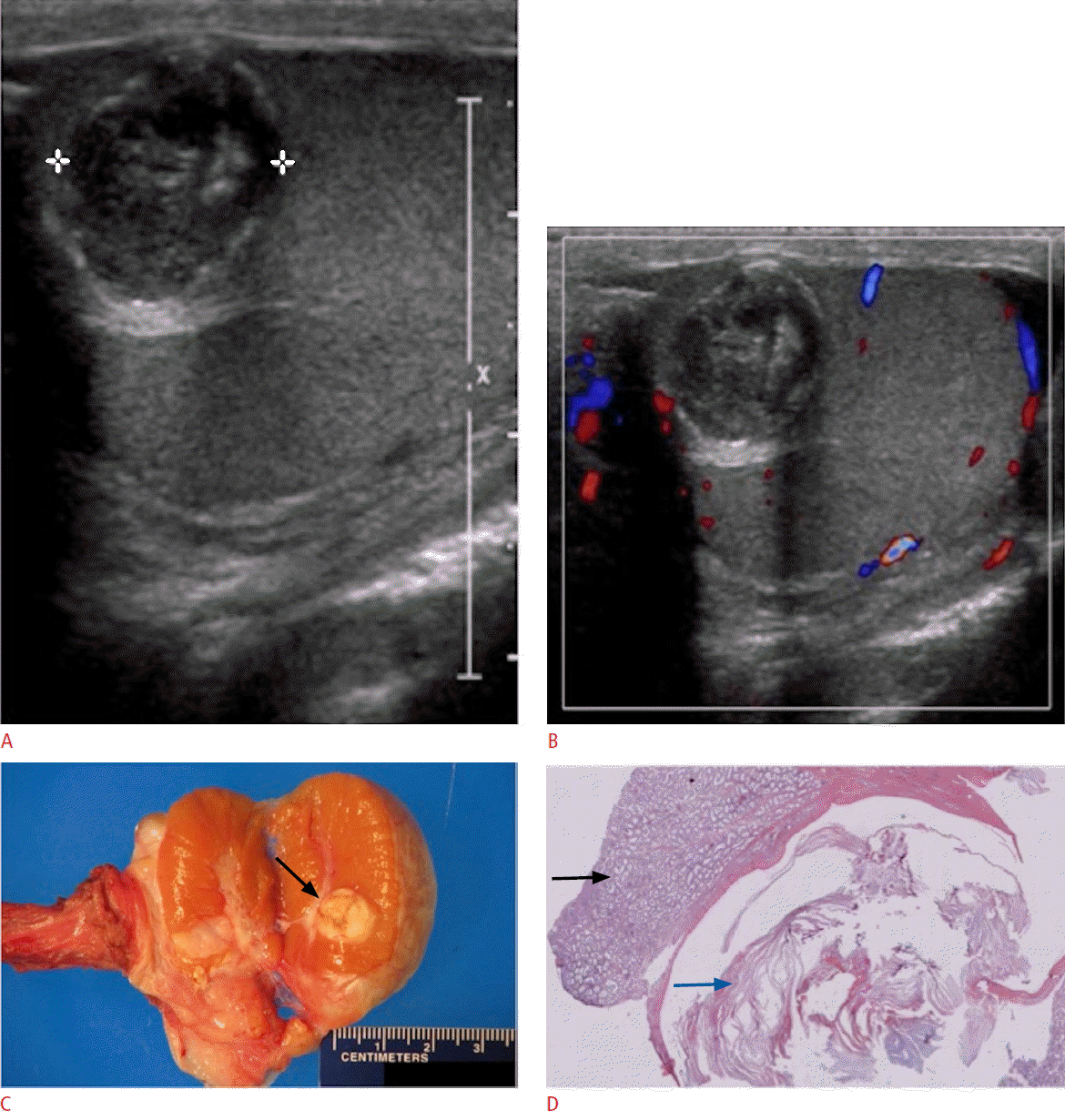
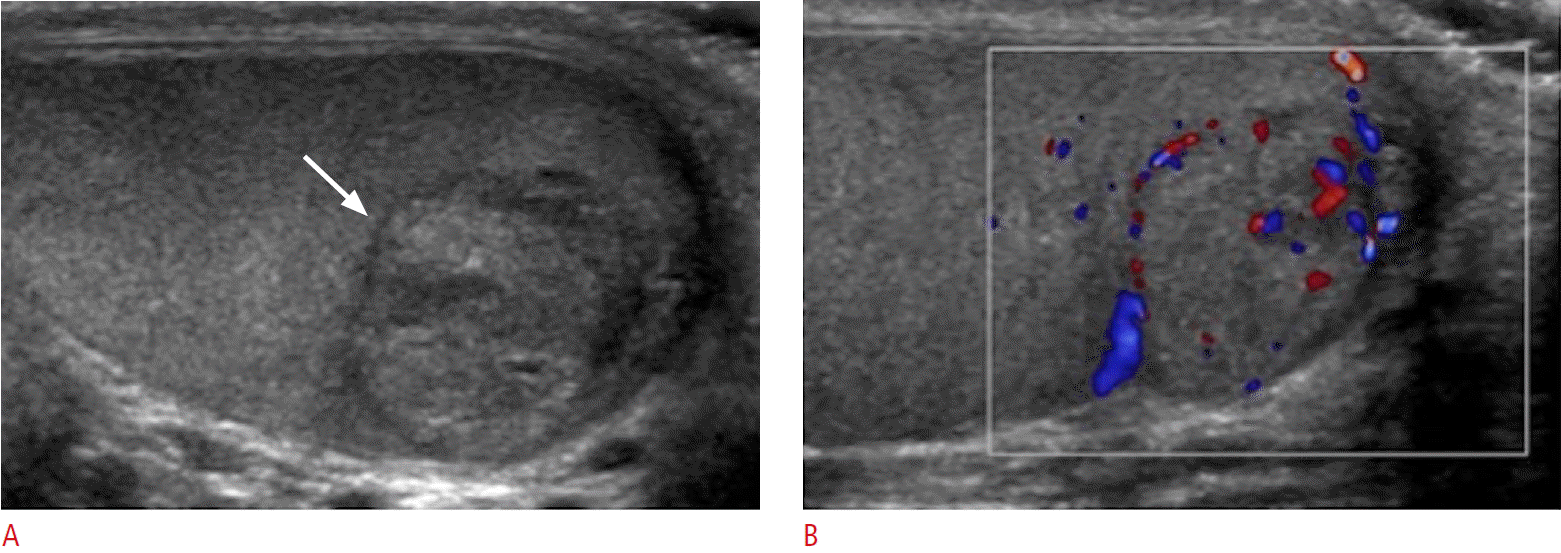
Epidermoid cysts often present as a non-tender small testicular nodule. They represent the most common benign testicular masses (1%-2% of testicular tumors) and have no malignant potential. Epidermoid cysts are often referred to as keratocysts due to their characteristic intraluminal keratin contents. The echogenic keratin can lead to a solid appearance on ultrasonography. Doppler evaluation, however, does not demonstrate internal vascularity (Fig. 14). Epidermoid cysts show different ultrasonographic appearances depending on their maturation. A lamellated pattern of alternating hypoechoic and hyperechoic layers forming an onion-ring/skin pattern is a classic presentation of a maturing epidermoid cyst [17,18]. This appearance grossly corresponds to the multiple intraluminal layers of keratin within the cyst [2,17,19]. Despite being a benign lesion, epidermoid cysts can often not be distinguished from malignant neoplasms such as teratomas, which may present with a similar ultrasonographic appearance. In the presence of an avascular lesion with typical ultrasound features and negative tumor markers, testicular enucleation can be considered rather than orchiectomy [19-22].
Spermatocele
Spermatoceles almost always arise in the epididymal head and are caused by cystic dilatation of the tubules of the efferent ductules [23]. Ultrasonographically they are indistinguishable from epididymal cysts. However, spermatoceles tend to be larger in size and may present as a multilocular cystic lesion with internal echoes representing proteinaceous fluid and spermatozoa [24]. Some literature reports a higher incidence of spermatoceles in patients after vasectomy, whereas epididymal cysts are reported to be more common in the general population [25-28].
Varicocele
A varicocele is seen in approximately 15% of adult men, making it the most common palpable mass of the spermatic cord [29]. Varicoceles form due to impaired drainage of blood from the spermatic cord causing abnormal dilatation of the pampiniform plexus [19,30]. Cases of idiopathic varicocele are simply caused by incompetent venous valves. However, secondary varicoceles are due to an increase of pressure in the spermatic veins caused by an extratesticular process such as cirrhosis, hydronephrosis or an abdominal/pelvic mass [2,19]. Clinically, palpation of the scrotum may reveal a mass that is often described as a “bag of worms.” It shows multiple hypo- or anechoic tubular structures greater than 2 to 3 mm in diameter. Occasionally detected low-level echoes within these veins result from slow blood flow. During the Valsalva maneuver the varicocele may enlarge and it may demonstrate flow reversal on color Doppler imaging depending on grade. Varicocele embolization has been shown to be as effective as surgical ligation (Fig. 15).
Varicoceles are most commonly found on the left side. The left testicular vein is longer and connects to the left renal vein at a 90° angle, resulting in increased pressure compared to the right testicular vein, which drains directly into the IVC. A newly diagnosed unilateral right-sided varicocele raises concerns of a secondary cause such as pelvic or abdominal malignancy. Compression of the left renal vein by the superior mesenteric artery, sometimes referred to as the Nutcracker syndrome, can also be a non-malignant cause of left-sided varicoceles, with increased pressures transmitted into the left pampiniform plexus [31].
Hydrocele
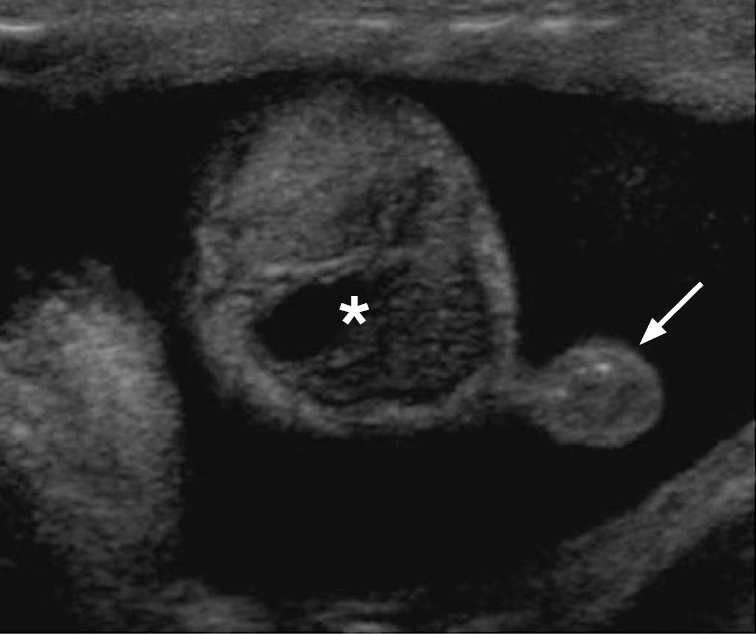
A hydrocele is a large collection of fluid between the visceral and parietal layers of the tunica vaginalis and the most common cause of painless scrotal swelling [32]. Of note, a small amount of serous fluid between the layers of the tunica vaginalis is a benign finding and should not be mistaken for a hydrocele. Hydroceles can be congenital or acquired. Congenital hydroceles are due to a patent processus vaginalis, which permits accumulation of peritoneal fluid in the scrotal sac. Acquired hydroceles are either idiopathic due to overproduction or impaired absorption of serous fluid. They may be secondary due to infection, torsion, trauma, or tumor [2,19].
Microlithiasis
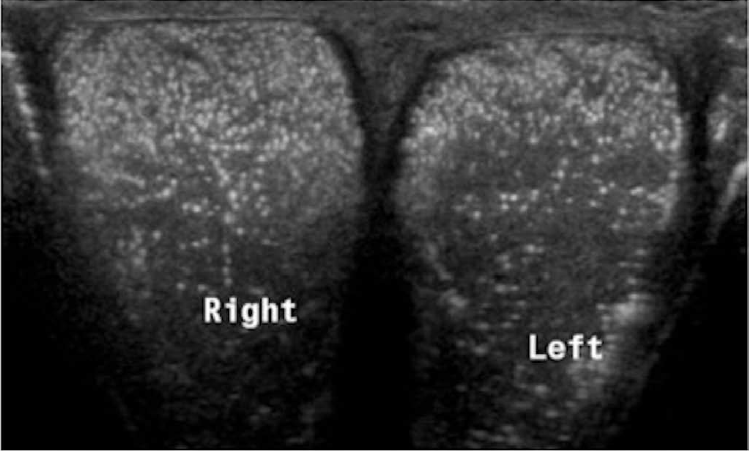
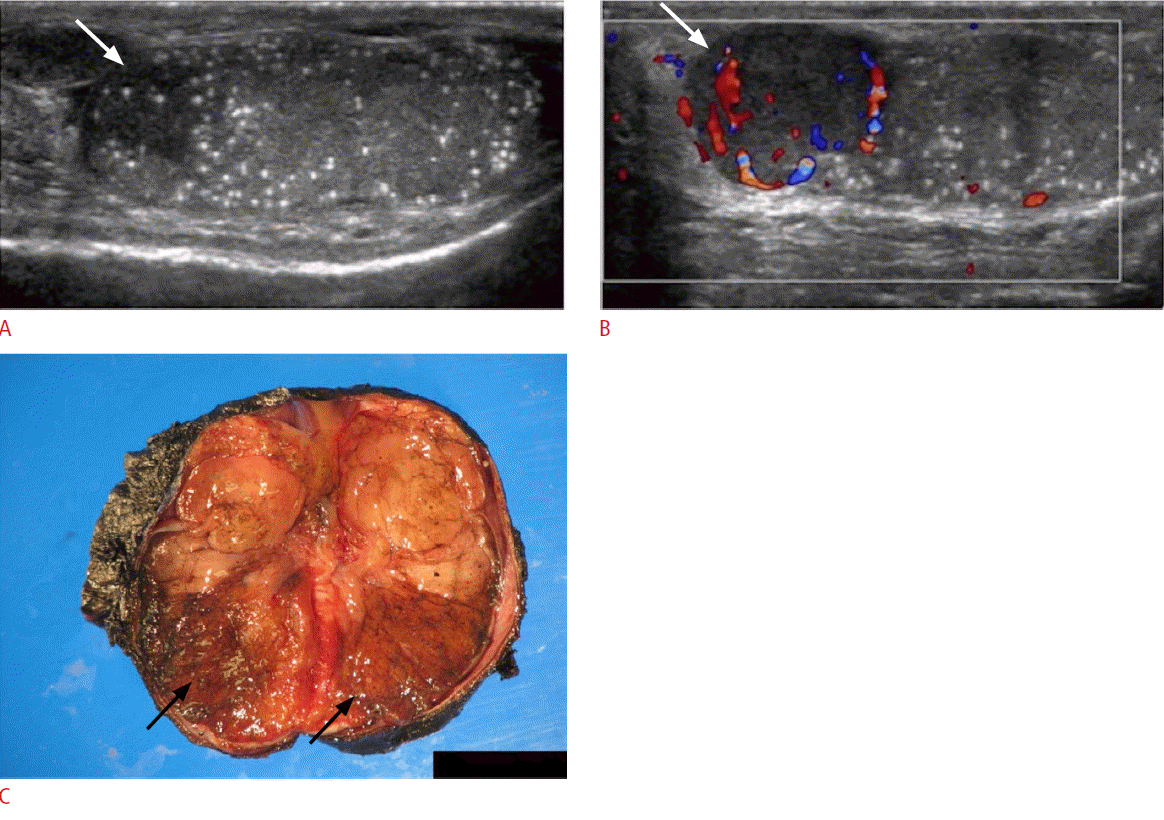
Testicular microcalcifications are usually found incidentally and are only seen in about 5% of males between the age of 17 and 35 [35]. Ultrasonography demonstrates intra-tubular calcifications of 2-3 mm in size as multiple, non-shadowing small echogenic foci that are randomly distributed throughout the testicle (Fig. 17) [36,37]. Five or more calcified foci per transducer field in one testis is considered abnormal. In 18% to 75% of cases, microlithiasis has been associated with testicular neoplasms (Fig. 18) [38,39]. The current literature does not provide any proof that testicular microcalcifications can be regarded as a premalignant condition or causative agent. Patients diagnosed with microcalcifications should undergo annual ultrasonography screening, especially when symptomatic. However, some literature suggests that intensive screening in asymptomatic patients may not be cost-effective and would do little to improve outcomes associated with testicular cancer [40-42].
Scrotolith
Scrotoliths, scrotal pearls or scrotal calculi are mobile calcifications in the scrotum and represent calcified loose bodies that result from torsion of the appendix epididymis/appendix testis or reactive fibrous proliferation during intrascrotal inflammation [33,43]. On ultrasonography, they appear as free-floating, echogenic foci measuring up to 10 mm with posterior acoustic shadowing and are located outside of the testicle (Fig. 19). The presence of a small amount of fluid or a hydrocele (50% association) facilitates their ultrasonographic identification. Overall, these calcifications have no clinical significance.
Adenomatoid Tumor
Adenomatoid tumor is a benign neoplasm that most commonly arises from the epididymal tail [44]. Accounting for approximately 30% of extratesticular tumors, it is the most common solid neoplasm of the epididymis. Ultrasonography assessment reveals a well-circumscribed hypoechoic, rounded mass with a usually homogeneous echotexture. Because the ultrasonographic appearance can vary, the tumor is often resected [28,44]. There are currently no documented cases of recurrence or metastatic spread following excision [45].
Germ Cell Tumors
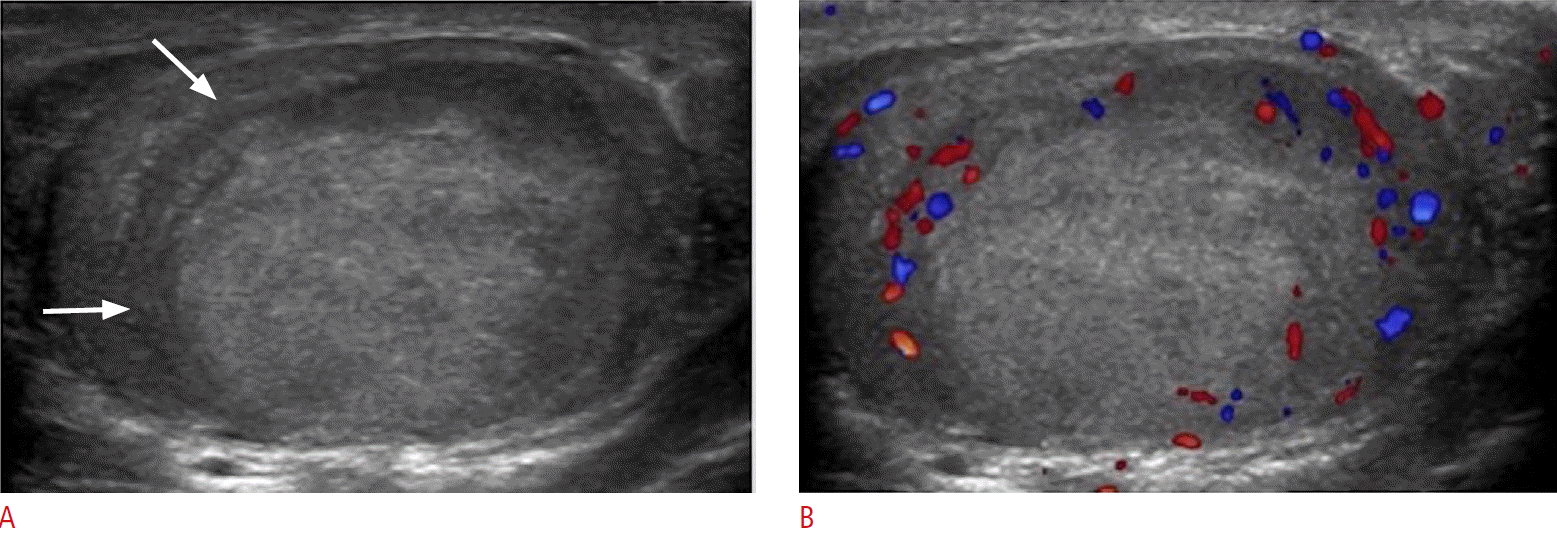
Germ cell tumors account for approximately 90-95% of all testicular tumors. They are further divided into seminoma and non-seminomatous germ cell tumors (NSGCTs), which is important in determining treatment and prognosis. Among germ cell tumors, seminomas are the most common testicular malignancy (35%-50% of all cases) [46]. Because of their high sensitivity to radiation and chemotherapy, seminomas have the best prognosis among germ cell tumors. On ultrasonography, seminomas appear as hypoechoic solid lesions with internal blood flow, which can range from small lesions to large masses that replace the entire testicle (Fig. 20) [47]. Metastases to the brain, lung and retroperitoneal lymph nodes via hematogenous and lymphatic spread are seen in approximately 25% of patients at the time of presentation [48].
Overall, NSGCTs are considered the most common testicular neoplasm (60% of cases) [36]. Pure NSGCTs are rare and most often encountered in the pediatric population [46]. They include teratoma, embryonal cell carcinoma, choriocarcinoma, yolk sac tumor and mixed subtypes [2,46]. The majority of NSGCTs manifest with advanced disease [49].
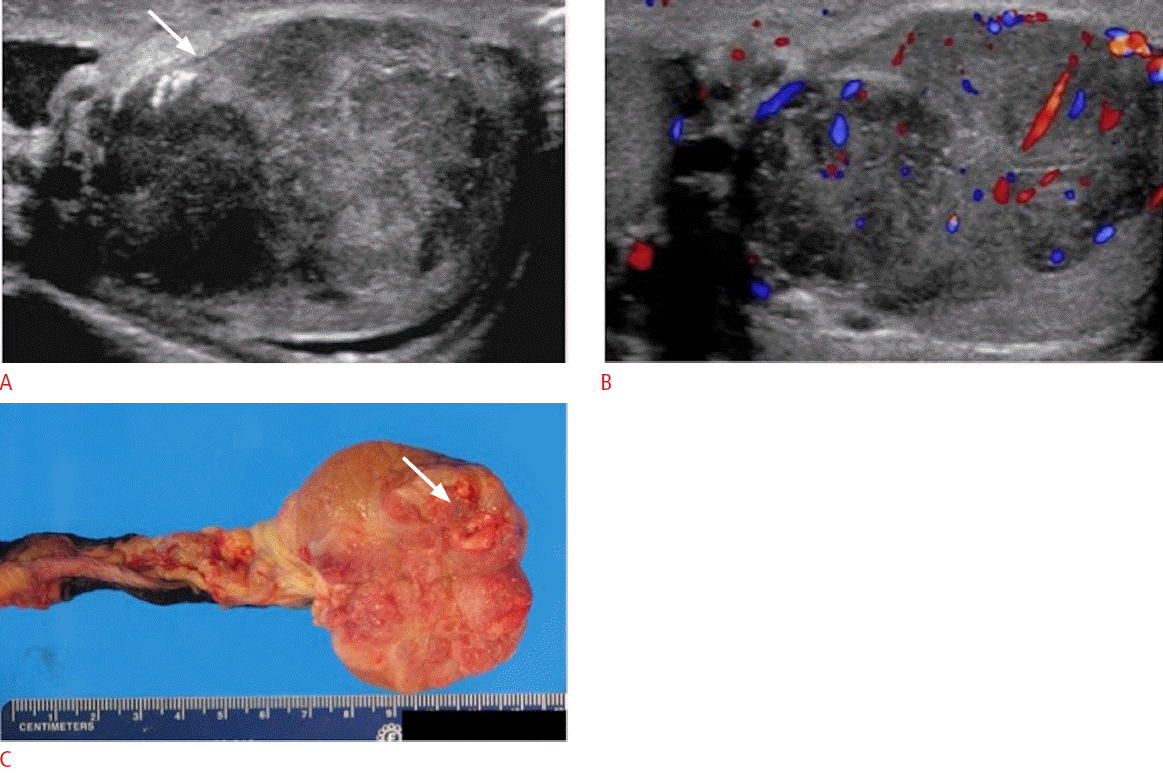
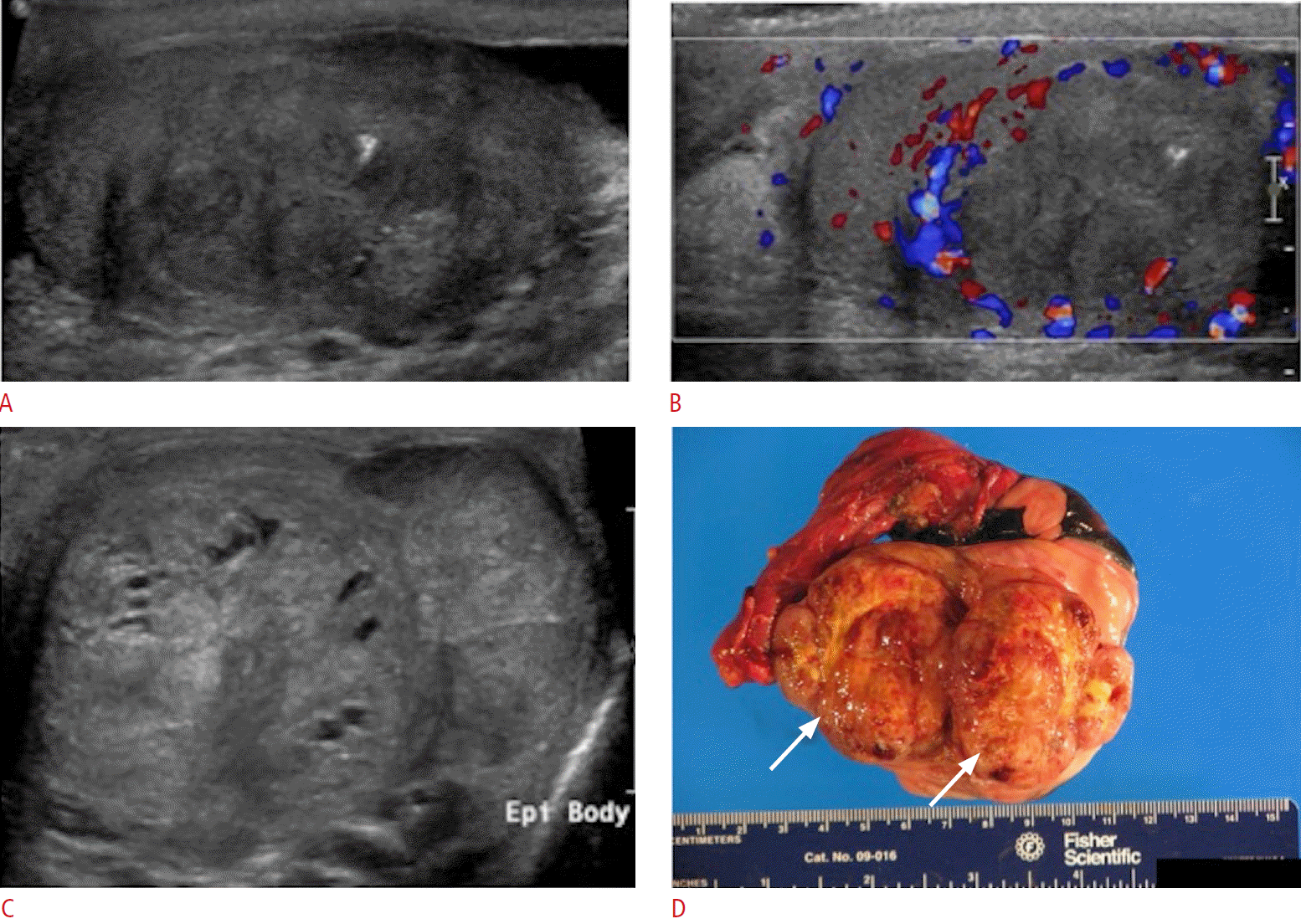
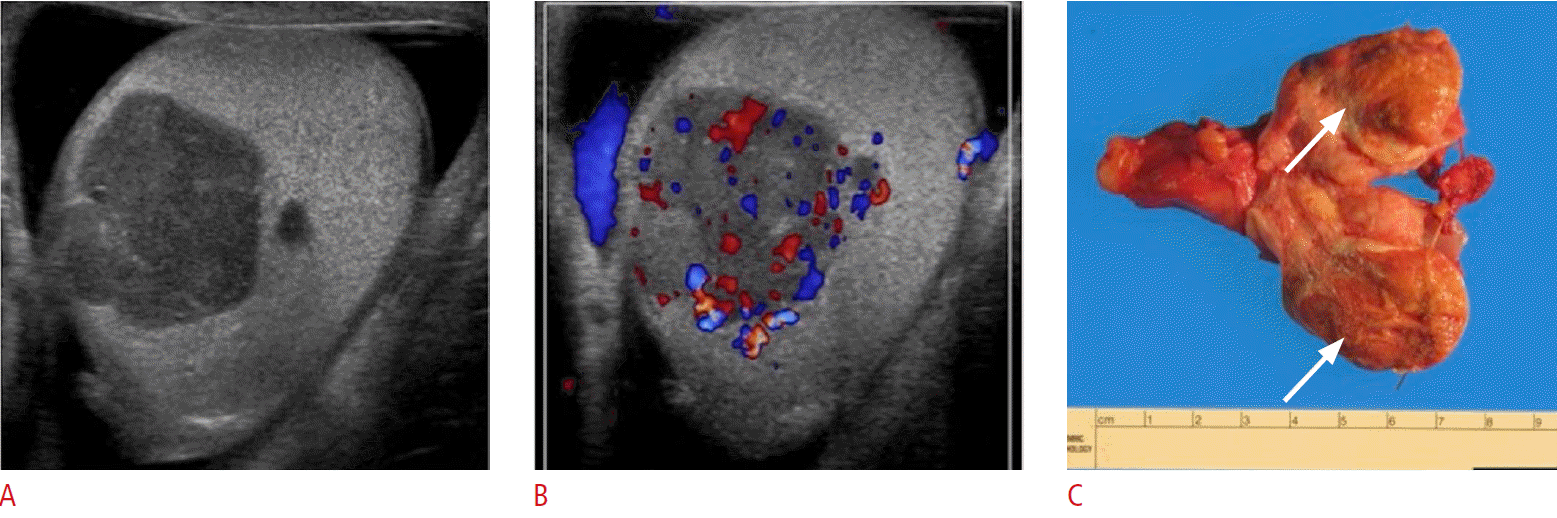
NSGCTs present ultrasonographically as heterogeneous and cystic masses with irregular margins (Figs. 21, 22). Echogenic foci within the mass may be seen, which can represent calcification, hemorrhage, or fibrosis. In some cases, the tumor may present with increased vascularity mimicking acute testicular inflammation. However, the underlying testicular parenchyma demonstrates an inhomogeneous appearance rather than a regular echotexture. Ultrasonographic follow-up evaluations are recommended to help differentiate true inflammatory states from tumors mimicking inflammation (Fig. 23).
Non-Germ Cell Tumor
Sex cord stromal tumors account for the majority of non-germ cell tumors (non-GCTs). These tumors are benign in about 90% of cases and usually found incidentally due to their small size. Frequently encountered non-GCTs are Sertoli cell tumors and Leydig cell tumors (Fig. 24); far rarer are granulosa cell tumors, fibromathecomas and mixed sex cord stromal tumors. These tumors do not exhibit specific ultrasonographic characteristics but appear as well-defined hypoechoic lesions. Given the nonspecific appearance on ultrasonography, orchiectomy is usually performed.
Summary
Ultrasonography remains the first-line imaging modality for evaluation of acute or chronic scrotal diseases. It is a safe and reliable tool for demonstration of scrotal anatomy, localization of testicular lesions and assessment of vascularity. As several testicular pathologies have characteristic ultrasonographic appearances, ultrasonography is able to appropriately guide patient management and potentially prevent unnecessary surgical intervention.



 Print
Print facebook
facebook twitter
twitter Linkedin
Linkedin google+
google+


 Download Citation
Download Citation PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC




